Main Points
- Terbinafine (Lamisil) is the most effective prescription treatment for toenail fungus, with a cure rate of about 70-80% when used as directed.
- Prescription treatments are significantly more effective than over-the-counter options for moderate to severe toenail fungus infections.
- Most toenail fungus treatments require patience, as visible improvement can take 3-6 months and complete clearing can take 9-12 months.
- Combination therapy using both oral and topical prescription medications often provides better results than either treatment alone.
- Prevention strategies are crucial after successful treatment, as recurrence rates remain high without proper foot hygiene and preventive measures.
Toenail fungus affects nearly 10% of adults worldwide. If you’ve tried over-the-counter remedies without success, prescription treatments offer your best chance at clearing the infection completely. While natural remedies have their place in early or mild cases, moderate to severe infections typically require medical intervention.
This all-inclusive guide dives into the top prescription choices on the market today, giving you a better idea of what to expect from treatment and which options may be best for your individual needs. Keep in mind that all prescription treatments necessitate a conversation with a healthcare provider who can evaluate the severity of your infection, your overall health, and any possible medication interactions.
Understanding Toenail Fungus Before Seeking Treatment
Toenail fungus, or onychomycosis in medical terms, is a condition that occurs when fungal organisms, usually dermatophytes, penetrate the nail bed through minuscule cracks or separations between the nail and the nail bed. If left untreated, the infection can lead to progressive changes in the nail’s appearance and structure as the fungus spreads deeper into the nail over time.
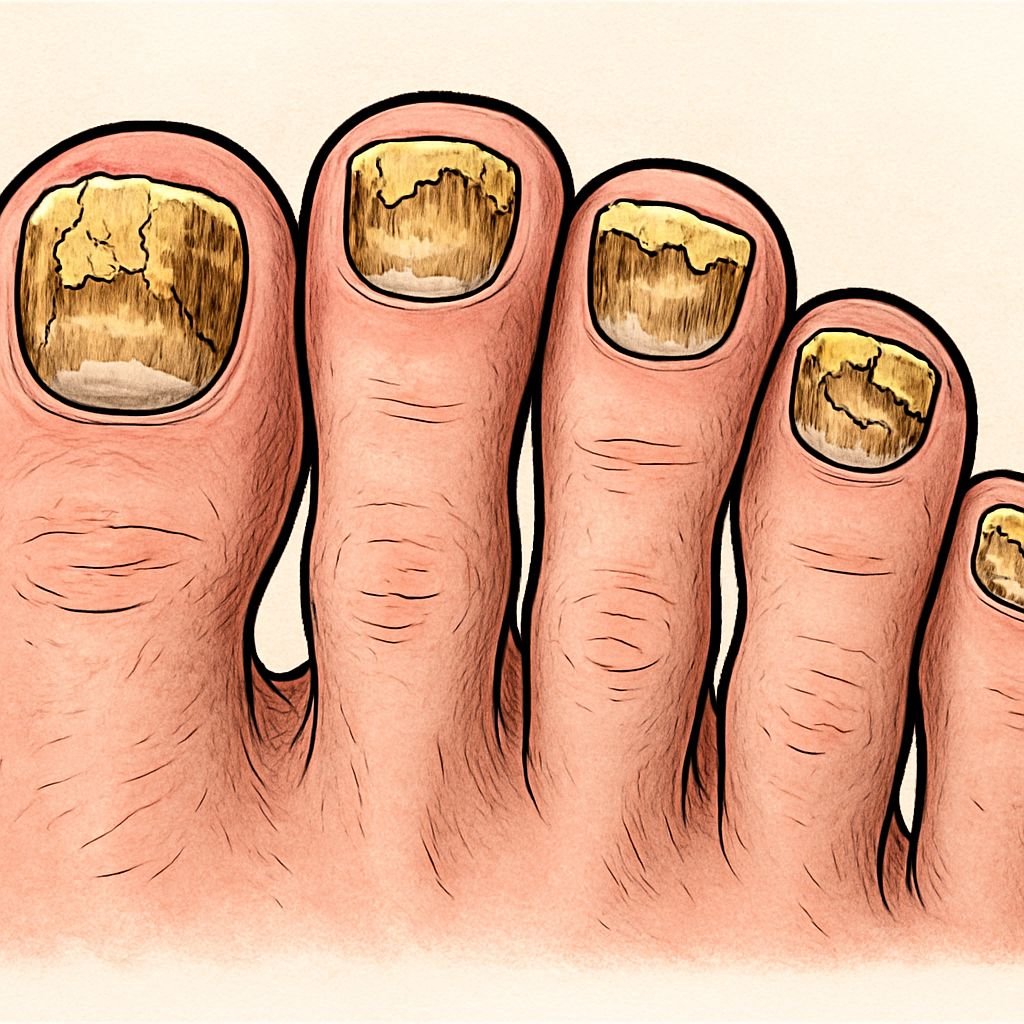
Many individuals are unaware that toenail fungus isn’t just an aesthetic issue—it’s a real infection that hardly ever goes away on its own. The nail provides an ideal environment for fungus to grow: dark, warm, and damp places where fungi flourish. As the infection worsens, the nails become more and more damaged, which can lead to pain, walking difficulties, and secondary bacterial infections in extreme cases.
How to Tell if You Have a Toenail Fungal Infection
Spotting toenail fungus early can greatly increase the success of treatment. The first signs are often so slight that you might not think anything of them—a tiny white or yellow spot at the tip of your nail. But as the infection gets worse, the symptoms become more obvious. Your nail might get thicker, start to crumble or become misshapen, lose its shine, or start to look strange.
Severe fungal infections can cause your nails to darken and they may appear yellow, brown, or even greenish-black. The nail may separate from the nail bed (onycholysis), creating a gap where debris accumulates. In some cases, you might notice a slightly foul odor or experience discomfort when wearing shoes or walking. If you observe any of these changes, particularly if they persist or worsen, consulting a healthcare provider becomes crucial for proper diagnosis and treatment.
The Advantages of Prescription Treatments Over OTC Options
One primary issue with over-the-counter antifungal treatments is that they have a hard time breaking through the nail plate to get to the infection. The human toenail is extremely tough, as it’s meant to shield the soft tissue underneath. Unfortunately, this protective feature also keeps most topical OTC solutions from effectively getting to the fungus, particularly when the infection has burrowed deep into or under the nail.
Prescription treatments are superior because they have stronger active ingredients, better delivery systems, and treatment methods that work from the inside out. Oral prescription drugs circulate through your bloodstream to reach the infection from beneath the nail, while prescription-strength topicals have more potent antifungal agents with enhanced penetration capabilities. Clinical studies consistently show that prescription treatments achieve significantly higher cure rates—typically 40-80% compared to the 10-20% success rates of over-the-counter products.
- Prescription medications taken orally travel through the bloodstream to reach the infection
- Prescription topicals are more potent with higher concentrations of antifungal agents
- Professional treatments get to the root of the problem, not just the symptoms
- Medically supervised treatments can be adjusted as needed based on your response
- Treatment plans can be tailored to the severity of your infection and your overall health
When to Seek Medical Attention for Your Toenails
While mild cases of toenail fungus might improve with home treatment, there are times when it’s best to seek medical attention. If you’ve tried over-the-counter treatments for 3-6 months without seeing an improvement, it’s time to see a healthcare provider. You should also seek a medical evaluation if you have diabetes, circulation problems, or a weakened immune system, as these conditions can increase your risk of complications from untreated fungal infections.
Other indications that you may need to see a doctor include the infection spreading to other nails, severe pain or discomfort, your nail separating from the skin underneath, or any signs of a bacterial infection, such as warmth, redness, or swelling around the nail. Seeing a dermatologist or podiatrist early on can lead to more successful treatment and help prevent complications. Most healthcare providers can diagnose toenail fungus just by looking at it, but they may take a small scraping from the nail to send to a lab for confirmation before they prescribe treatment.
Best Oral Prescription Treatments for Toenail Fungus
Oral antifungal medications are the most successful treatment for moderate to severe toenail fungus infections. These medications work throughout the body, traveling through your bloodstream to reach the infection from under the nail bed. This method of delivery overcomes the penetration problem that topical treatments have, allowing the medication to attack the fungus from inside the nail.
Usually, a doctor will prescribe oral antifungal medication that you’ll take for a certain amount of time, typically between 6-12 weeks. However, even after you stop taking the medication, the nail will continue to clear for several months as the healthy part of the nail grows. These medications are effective, but they may require monitoring of liver function in some cases and may interact with other medications you’re currently taking. It’s important to give your doctor a full list of all medications and supplements you’re taking before you start treatment.
Terbinafine (Lamisil): The Best Bet
When it comes to oral prescription treatments for toenail fungus, Terbinafine (Lamisil) is the top dog. It’s shown to have the highest cure rates in clinical studies—about 70-80% when taken properly. Unlike other antifungals that only stop fungal growth (fungistatic), terbinafine actually destroys the fungal organisms (fungicidal), which leads to more thorough and long-lasting results.
Typically, you’ll take 250mg per day for 6-12 weeks, depending on how severe your infection is. Even after you’ve finished your course of terbinafine, it stays in your nail tissue for several months, continuing to work as your healthy nail grows out. This medication is particularly good at fighting off dermatophytes, the most common cause of toenail fungus, which is why it tends to be more effective than other options. For more information on toenail fungus and its treatments, you can visit Cleveland Clinic’s resource page. While most people tolerate it well, side effects can include headaches, upset stomach, and, very rarely, changes in taste or liver problems.
Itraconazole (Sporanox): A Powerful Option
For those who can’t handle terbinafine or have infections from non-dermatophyte molds or yeasts, Itraconazole (Sporanox) is a strong option. This azole class antifungal works by interrupting the formation of the fungal cell membrane. Clinical studies have shown cure rates of about 60-70%, which makes it a little less effective than terbinafine but still much more effective than just using topical treatments.
Your doctor will usually prescribe itraconazole in one of two ways: either 200mg every day for 12 weeks without a break, or in pulse therapy where you take 200mg twice a day for one week every month, repeated for 2-3 months. The pulse therapy method reduces the chances of side effects while still being effective. Itraconazole can interact with more drugs than terbinafine, so your doctor will carefully check your list of medications before prescribing it. Common side effects include feeling sick, pain in your stomach, and in rare cases, making heart failure worse in people who are already at risk. For more detailed information, you can read about toenail fungus treatments.
Fluconazole: A Less Popular Option That’s Occasionally Used
Fluconazole is often a third choice for doctors when patients can’t handle the primary treatments or have reasons they can’t use them. Although it isn’t specifically approved by the FDA for onychomycosis, research shows it’s moderately effective when taken once a week at a dose of 150-300mg for 6-12 months. Some patients prefer this option because they only have to remember to take it once a week instead of every day. For those seeking rapid solutions, prescription medication options are also available.
Fluconazole often has a cure rate of 40-50%, which is lower than both terbinafine and itraconazole, but is still a significant improvement over not treating the fungus at all. This medication is particularly useful against certain types of fungal infections, as it has been shown to be more effective against Candida species than dermatophytes. The side effects of fluconazole tend to be less severe than other oral antifungals, although headaches, nausea, and potential drug interactions are still issues to consider.
Potential Risks and Side Effects of Oral Antifungal Medications
There are potential risks associated with all oral antifungal medications that need to be considered against the benefits they provide. The most significant risk is related to liver function, as these medications are processed in the liver. It is likely that your doctor will conduct initial liver function tests before beginning treatment and may conduct these tests again during treatment, particularly with terbinafine and itraconazole. If you have a pre-existing liver condition, your doctor may suggest alternative treatments.
Oral antifungals often have side effects such as headaches, stomach problems (nausea, diarrhea, stomach pain), and skin rashes. There are also less common but more serious side effects such as liver damage, heart failure (especially with itraconazole in susceptible people), and severe skin reactions. Another important consideration is drug interactions, as oral antifungals can affect the metabolism of many common medications. Always tell your healthcare provider about all medications, supplements, and health conditions before starting treatment.
Doctor-prescribed Topical Treatments for Fungal Infections
Prescription topical treatments offer targeted therapy directly to the site of infection without exposure to the whole system. These medications are most effective for mild to moderate infections, especially those that only affect part of the nail or are in the early stages. They are also great options for patients who can’t take oral medications due to health issues or potential drug interactions.
Today’s prescription topical treatments have come a long way from their predecessors, with better nail penetration and higher success rates. Although they generally have lower cure rates than oral treatments (usually around 15-40%), they have fewer systemic side effects and fewer concerns about drug interactions. For more information on oral treatments, you can explore oral antifungal medication myths. Treatment usually takes longer and often requires daily application for 9-12 months to get the best results.
Jublia (Efinaconazole): Newest Topical Treatment
Jublia (Efinaconazole) is one of the most recent and most successful topical prescription treatments for toenail fungus. This treatment, which was given the green light by the FDA in 2014, uses cutting-edge technology to improve penetration through the nail plate to reach the nail bed, where the infection is located. Clinical trials show that after 48 weeks of treatment, the complete cure rate is around 15-18%, with up to 40-50% of patients seeing a significant improvement in the appearance of their nails.
How Tavaborole (Kerydin) Works
Tavaborole (Kerydin) is a newer treatment option that works differently than other antifungal medications. It targets a specific enzyme (leucyl-tRNA synthetase) that fungi need to produce proteins. This innovative method helps to avoid potential resistance problems that can occur with other types of antifungal treatments. The solution is also made up of small molecules that allow it to penetrate the nail plate and reach the site of infection more effectively than older topical treatments.
Tavaborole is a daily treatment that you apply with the included dropper. You must use it consistently for 48 weeks to get the best results. Clinical studies show that about 7-9% of people are completely cured, and 27-36% of people have significant improvement in nail clearance. These numbers may seem small compared to oral medications. But tavaborole is a good choice for people who can’t tolerate systemic treatment.
- Penetration is enhanced by a low molecular weight formula
- Resistance concerns are addressed by a novel mechanism
- Side effect risks are reduced by minimal systemic absorption
- Application protocol is easy and once-daily
- After drying completely, it is compatible with nail polish
Common side effects are primarily local, including redness at the application site, flaking, or ingrown toenails in rare cases. The medication has minimal systemic absorption, which makes it particularly suitable for patients with multiple health conditions or those taking numerous other medications where drug interactions could be a concern.
The Tried-and-True Ciclopirox (Penlac)
As the first prescription topical treatment for toenail fungus to be approved by the FDA, Ciclopirox (Penlac) lacquer has a proven track record. It’s delivered in a clear nail polish format that’s applied daily to the affected nails. You’ll need to remove this 8% solution weekly with alcohol before starting the next round of applications. This treatment works by blocking various fungal cellular processes and creating a barrier against reinfection as it builds up on the nail surface. For more rapid results, you might consider exploring other prescription medications that are available.
Maximizing the Effectiveness of Topical Solutions
To get the most out of your topical prescription treatments, you need to apply them correctly. Start by washing and drying your feet. If your medication requires it, gently file the surface of your nail to remove any debris and help the medication penetrate. Apply the solution exactly as directed. This usually means applying it to the entire surface of the nail, the edges of the nail, and underneath the nail if possible. Wait for the solution to dry completely before putting on socks or shoes. This usually takes at least 10 minutes, but it can take longer depending on the product. For more information on effective treatments, you can explore rapid toenail fungus treatment options.
Mixing It Up: How Combination Therapy Boosts Success Rates
When it comes to treating a serious or persistent toenail fungus infection, more and more doctors are turning to combination therapy. This approach uses several different treatments at the same time. It’s been found to be more successful than just using one treatment, especially for people who have had the infection for a long time, have a lot of the fungus in their nails, or have tried other treatments that didn’t work. The idea is that by attacking the fungus in several different ways at once, it’s more likely to get rid of the infection. This is because it can tackle any resistance the fungus may have built up, and it can reach more of the fungus.
Many treatment plans combine an oral medication with a topical solution, but some may also include physical or mechanical treatments. Even though this approach can make treatment more complex and expensive, the improved results often make the extra investment worth it for many patients. This is especially true for those with major functional or aesthetic concerns related to their infection.
Doctor’s Opinion: “In my two decades of treating patients, I’ve found that combining oral and topical medications works best for moderate to severe toenail fungus. Typically, the cure rate is 15-20% higher than when using just one type of medication. For those interested in exploring this further, consider looking into rapid toenail fungus treatment options. While this approach does require more of a commitment from the patient, the results are significantly better.”
Usually, the length of time it takes for combination therapy to work is about the same as it is for topical treatments (9-12 months) for total healing, although you will probably see some improvement much sooner than that. Your doctor will keep an eye on how you’re doing during the treatment, and may change the treatment plan based on how you’re responding and any side effects you’re having. For more information on effective treatments, you can explore this comprehensive guide on toenail fungus treatments.
Combining Oral and Topical Medications
Using both oral and topical prescription medications can provide a potent double whammy against fungal infections. Oral medications work from the inside out, carrying antifungal agents through the bloodstream to the nail bed, while topical solutions work from the outside in, attacking the infection right at the nail surface. This all-encompassing method attacks the infection from all sides, greatly increasing success rates compared to using either treatment on its own.
Studies have found that combining terbinafine tablets with ciclopirox nail lacquer or efinaconazole solution can boost the full cure rate by around 15-25% compared to just taking oral medication. Your doctor might prescribe a regular course of oral medication, usually for 6-12 weeks, along with a longer course of topical treatment, for 9-12 months, to make sure the infection is fully wiped out. This approach does require more dedication to sticking with the treatment, but the better results often make the extra effort and cost worthwhile. For more information on effective treatments, you can read about toenail fungus treatment options.
When Nail Removal Might Be Necessary
In some cases, your doctor may recommend that you have part or all of your nail removed (a procedure known as onychectomy). This is usually only suggested if the infection is severe, if the nail has lifted off the nail bed, or if other treatments haven’t worked. Removing the nail can help the doctor apply antifungal drugs directly to the infected area.
There are two ways to remove a toenail: surgical excision or chemical dissolution with a urea compound. Both are usually done under local anesthesia to keep you comfortable. After the nail is removed, antifungal medication is applied directly to the nail bed, which is a very effective treatment. The nail usually grows back in 6-12 months, although it can take longer in older adults or people with circulation problems.
Up and Coming Treatments: Laser and Light Therapy
Laser and photodynamic therapies are the newest advancements in toenail fungus treatment, providing non-drug options for those worried about drug interactions or side effects. These methods use certain light wavelengths to target and kill fungal cells, leaving the healthy tissue untouched. Although they are not usually covered by insurance and are still considered to be supplementary to traditional treatments, these technologies have shown potential in clinical trials.
Treatments using Nd:YAG lasers usually need 3-4 sessions, with several weeks in between each one. The process is generally not painful, and doesn’t require anesthesia or recovery time. Clinical studies have shown that these treatments improve the condition in 30-70% of cases, although complete cures are less common, at 15-30%. These treatments work best when they’re used along with topical antifungals, as part of a comprehensive treatment plan. Your podiatrist or dermatologist can tell you if you’re a good candidate for these new treatments, based on the specific characteristics of your infection.
What You Should Know About Toenail Fungus Treatment
It’s important to understand that treating toenail fungus isn’t a quick process. Unlike many other health issues that can be resolved relatively quickly, toenail fungus treatment takes time and consistent treatment. This is because toenails grow slowly, so even after the fungus has been killed, it takes time for the healthy nail to grow and replace the infected part. That’s why the success of toenail fungus treatment is measured in months, not days or weeks.
What to Expect: The Long Haul
Knowing the usual treatment schedule can help patients stay motivated throughout the long process. In the initial 4-6 weeks of treatment, you might not see much, if any, visible improvement in the nail’s appearance, but rest assured, the medication is working hard to kill the fungus. Usually, around months 2-4, you’ll start to see small areas of healthy nail growing from the cuticle as the new, uninfected nail slowly replaces the old, damaged portion.
It usually takes about 4-6 months of treatment before you start to see a noticeable difference in the health of your toenail. The healthier part of the nail will start to become more visible. Because toenails grow so slowly (about 1mm per month), it usually takes about 9-12 months for the toenail to completely clear up. This is because the treatment doesn’t actually remove the damaged part of the nail. Instead, it prevents new infections from forming while the healthy part of the nail slowly grows in to replace the damaged part. For more information on effective treatments, you can explore toenail fungus treatment options.
While you are being treated, keep doing your usual activities but follow your doctor’s advice about how to care for your nails. For example, keep your nails cut short and straight across. Don’t use nail polish on infected nails unless your healthcare provider says it’s okay. Some types of nail polish can make the treatment less effective or trap moisture, which can help the fungus grow.
Effectiveness of Various Prescription Treatments
Knowing the effectiveness of different treatments can help set realistic expectations for the results of treatment. Oral terbinafine is the most effective prescription treatment, with a complete cure rate of 70-80% in clinical trials. This is followed by itraconazole, which has a complete cure rate of 60-70%, and fluconazole, which has a complete cure rate of 40-50%. Prescription topical treatments are less effective, with efinaconazole having a complete cure rate of 15-18%, ciclopirox having a complete cure rate of 8-12%, and tavaborole having a complete cure rate of 7-9%. However, all treatments have significantly higher rates of “clinical improvement,” which is defined as at least 50% clearance of the infected nail. For more detailed information, you can explore which toenail fungus treatment is best.
Using a combination of treatments usually improves success rates by 15-25% compared to using one treatment on its own. How well a patient responds to treatment can depend on a number of things, including how severe the infection is, how long they had the infection before they started treatment, their overall health, and how well they stick to their treatment plan. Keeping the nails clean and taking steps to prevent re-infection during treatment can also help to make the treatment more successful. This shows that treating toenail fungus successfully is about more than just taking medication.
How to Tell If Your Treatment Is Effective
Knowing that your treatment is working can help you stay motivated during the long treatment process. The first sign of progress usually comes in the form of a small area of clear, healthy nail growing from the cuticle. This clear part will slowly get larger as the nail grows, pushing the infected part toward the tip of the nail. You might see the infected area becoming more specific and contained instead of spreading to healthy nail tissue.
Stop Fungus from Coming Back After Treatment
Even after you’ve successfully treated it, toenail fungus can come back in about 10-50% of people within 1-3 years if you don’t take steps to prevent it. This high rate of recurrence shows how important it is to keep preventing fungus as a key part of managing it over the long term. Most of the time, when the fungus comes back, it’s because you’ve been re-infected, not because the treatment didn’t work. This shows how important it is to make changes in your lifestyle and personal hygiene to keep your nails healthy after you’ve finished your prescription treatment.
Everyday Routines to Prevent Fungus
Preventing the return of fungus requires a consistent focus on the environmental factors that encourage the growth of fungus. Make sure to keep your feet clean and completely dry, especially in the spaces between your toes where moisture can build up. Change your socks at least once a day, and more often if your feet sweat a lot or if you work out. Avoid walking without shoes in public areas like swimming pools, gyms, and showers where fungus can flourish and where it is often transmitted. For more natural solutions, consider exploring essential oil blends that can help prevent fungal growth.
By rotating your shoes, you can ensure they dry out completely between uses, which will help to reduce the damp conditions that fungi love. You might also want to consider using antifungal powders or sprays in your shoes to make them less appealing to fungi. If you go to nail salons, make sure they properly sterilize all their equipment. Even better, bring your own sterilized tools to avoid the risk of cross-contamination.
- Make sure to clean your feet with soap and water every day, making sure to dry them thoroughly, especially between the toes
- Change your socks at least once a day, and try to choose socks that are made from moisture-wicking materials
- Give your shoes at least 24 hours to dry out completely between each time you wear them
- Use an antifungal powder or spray in your shoes once a week
- Try to avoid walking around barefoot in public places like swimming pools and showers
Trimming your toenails properly, straight across, can help to prevent damage that could allow fungal organisms to get in. After each use, disinfect your nail clippers and any other tools you use for a pedicure, to prevent them from becoming recontaminated. Some dermatologists recommend that, as an additional preventive measure after you’ve finished a course of prescription treatment, you should apply an over-the-counter antifungal cream to the area around your nail once a week. This is especially recommended for people who have a history of getting infections repeatedly.
Choosing the Right Shoes and Keeping Feet Clean
What you put on your feet can greatly affect your chances of getting toenail fungus again. Choose shoes that are made of materials that let air in and sweat out. Try to stay away from synthetic materials that keep heat and sweat in, which is the perfect place for fungus to grow. If you’re going to be doing sports or other physical activities, think about getting technical fabrics that are made to pull sweat away from your skin. You can also get special antifungal socks that have silver or copper in them to give you extra protection. These socks make it hard for fungus to grow.
When Maintenance Therapy Might Be Necessary
Patients who have had multiple recurrences or who have significant risk factors may be advised by their healthcare providers to use maintenance therapy after they have completed their initial treatment course. This typically means that they will use a topical antifungal medication intermittently or take oral medication periodically to prevent the fungus from returning. Common maintenance regimens include applying a topical antifungal to the nails once or twice a week or taking a pulse-dose oral antifungal for one week every two to three months. These protocols have been shown to significantly reduce recurrence rates in individuals who are at high risk, but they do require an ongoing commitment to regular treatment.
Common Questions
People often have questions about prescription treatments for toenail fungus, especially about the safety of the medication, how long the treatment will last, and whether their insurance will cover it. Answering these questions can help people decide which treatment option is best for them and know what to expect during the treatment process.
The responses given below are based on the latest medical knowledge and standard practices, but individual cases may differ depending on specific health conditions and circumstances. As always, you should consult your healthcare provider for advice that is personalized to your unique situation.
Is it safe to use prescription toenail fungus treatments if I have liver issues?
Your liver health can significantly affect your treatment options for toenail fungus. This is because oral antifungal medications are processed in the liver. If you have a pre-existing liver disease or abnormal liver function tests, your doctor will likely advise caution with oral antifungals or recommend alternative treatments. Prescription topical treatments such as efinaconazole (Jublia) or tavaborole (Kerydin) are often safer alternatives for patients with liver issues, as they have minimal systemic absorption. Some patients with minor liver issues may still be eligible for oral medications, but with adjusted dosing and careful monitoring of liver function during treatment.
How long does it take for prescription toenail fungus treatments to work?
How long you’ll need to take prescription medication for toenail fungus depends on the type of medication and how severe your infection is. If you’re prescribed oral terbinafine, you’ll usually need to take it once a day for 6 to 12 weeks. But it can take several months for the medication to completely get rid of the fungus. Itraconazole is usually taken once a day for 12 weeks. But it can also be taken in a different way called “pulse dosing.” This means you take it once a day for 1 week per month for 3 or 4 months. Topical prescription treatments usually need to be applied every day for 9 to 12 months. Even after you finish taking the medication, it can take several months for your nail to look better. This is because the nail needs time to grow out. It usually takes about 9 to 12 months for a toenail to fully grow out.
Does insurance cover prescription toenail fungus treatments?
The extent of insurance coverage for toenail fungus treatments varies greatly among providers and specific plans. Most insurance companies cover oral antifungal medications such as terbinafine and itraconazole, although they may require prior authorization to show medical necessity. Coverage for prescription topical treatments is often more limited, with many insurers categorizing these medications as “tier 3” or even non-formulary, leading to higher copays or no coverage. Without insurance, oral terbinafine may cost $10-30 for a full treatment course (generic), while prescription topicals like Jublia or Kerydin can cost $500-1200 for an 8-10mL bottle without coverage.
There are a number of patient assistance programs offered by drug manufacturers that can help to reduce costs for those with limited or no insurance coverage. You can ask your healthcare provider about these programs or look on the drug manufacturer’s website for more information. You may also find that prescription discount cards and mail-order pharmacies can help to significantly reduce your out-of-pocket expenses for these medications.
Is it safe to drink alcohol while taking oral antifungal medications?
The guidelines for drinking alcohol while on antifungal medications differ depending on the specific drug. While terbinafine has very few interactions with alcohol, it is generally recommended by doctors to limit alcohol consumption to moderate levels while on this medication. On the other hand, itraconazole and fluconazole can both cause stress to the liver, and this can be made worse by drinking alcohol. Some people may also experience a disulfiram-like reaction (which can cause flushing, nausea, and headaches) when they drink alcohol while on certain antifungal medications.
For the best results and safety, you might want to avoid drinking alcohol while you’re taking oral antifungal medicines, especially azole antifungals. If you can’t stop drinking completely, talk to your doctor about how much is safe for you to drink while you’re taking this medicine. Your doctor will consider the specific medicine you’re taking, how often you’re taking it, and your overall health. Keep in mind that prescription creams and ointments don’t get into your system much, so they usually don’t interact with alcohol.
How are prescription toenail fungus treatments different from over-the-counter options?
There are a few key differences between prescription and over-the-counter treatments for toenail fungus. Prescription medications have more potent active ingredients at higher doses. Oral prescription medications work systemically, meaning they travel through the bloodstream to treat the infection. Prescription topical treatments have advanced nail penetration technology. According to clinical studies, prescription treatments have a much higher cure rate (40-80%) than over-the-counter treatments (usually 10-20% at most).
Most over-the-counter treatments are topical solutions that contain undecylenic acid, tea tree oil, or low-concentration antifungals. These treatments only work on the surface and may help with very mild or early infections. However, they rarely penetrate deeply enough to treat established infections beneath the nail plate. Prescription treatments are specifically tested and approved by the FDA for onychomycosis. Many over-the-counter products don’t have substantial evidence supporting their effectiveness for nail infections. For more information on effective treatments, you can explore rapid toenail fungus treatment options.
If you’re dealing with a mild, early-stage infection that affects less than half of your nail, it might be worth trying out some high-quality over-the-counter options first. But if you don’t see any improvement after 3-6 months, or if your infection is moderate to severe, you should definitely consider prescription treatments, as they have significantly higher success rates.
Although it takes time and consistency to treat toenail fungus, prescription treatments are your best bet for completely getting rid of the infection and returning your nails to health. It’s important to work with your healthcare provider to choose the treatment that’s best for you, which will increase your odds of success and reduce the risk of side effects or complications.
If you’re looking to dive deeper into all things foot health or if you’re in need of a top-notch podiatrist to help you kick toenail fungus to the curb, head on over to FootHealth.com. We’ve got all the scientifically-backed information you need to take care of those feet.

 Nail Fungus Cures Instant Cures for Painful Nails and Fungus
Nail Fungus Cures Instant Cures for Painful Nails and Fungus