Key Takeaways
- Multiple nail infections typically require systemic oral antifungals, while single nail infections may respond to topical treatments alone
- Treatment duration increases significantly when multiple nails are affected, often requiring 3-6 months longer therapy than single nail cases
- Combination therapy approaches show significantly higher cure rates (up to 80%) for multiple nail infections compared to monotherapy (30-50%)
- The type of nail infection (distal lateral, proximal subungual, or total dystrophic) directly impacts treatment selection and success rates
- Preventive measures post-treatment are crucial as multiple nail infections have a 20-25% recurrence rate without proper maintenance
Why Nail Infections Need Different Treatment When Multiple Nails Are Affected
Nail infections don’t always play by the same rules. When multiple nails become infected simultaneously, the treatment approach requires significant adjustment compared to single nail cases. This distinction isn’t merely about quantity—it reflects fundamental differences in infection severity, causative organisms, and the body’s ability to respond to treatment.
Multiple nail infections often indicate a more robust fungal presence or underlying condition affecting the body’s defense mechanisms. According to clinical studies, patients with infections affecting more than three nails typically have deeper fungal penetration and higher fungal loads throughout the nail apparatus. This increased pathogen burden requires more aggressive therapeutic approaches to achieve complete resolution.
Beyond just the technical aspects of treatment, multiple nail infections frequently serve as indicators of potential systemic issues such as diabetes, immunosuppression, or peripheral vascular disease. For this reason, your healthcare provider may conduct additional testing when multiple nails are affected, treating not just the visible symptoms but potentially addressing underlying health concerns contributing to the widespread infection.
Single Nail Infections: First-Line Treatment Options
When tackling a solitary infected nail, treatment options typically begin with less invasive approaches. Single nail infections, particularly those caught early, often respond well to conservative therapies that avoid systemic medication exposure. The typical treatment journey starts with proper diagnosis confirmation through microscopic examination or fungal culture to identify the specific pathogen.
For most patients with a single affected nail, especially with less than 50% nail plate involvement and no matrix infection, topical antifungal therapy serves as the primary approach. These medications can penetrate the nail plate to reach the infection site while avoiding potential systemic side effects associated with oral medications.
Single Nail Treatment Decision Matrix
• Less than 50% nail involvement: Topical therapy first line
• No matrix involvement: Topical therapy appropriate
• Superficial white onychomycosis: High topical success rate
• Distal lateral subungual affecting less than half the nail: Topical options viable
• Immunocompetent patient: Can start with conservative approach
Topical Medications: When They Work Best
Topical antifungal medications provide targeted treatment directly to the infection site without systemic exposure, making them ideal first-line options for isolated nail infections. Products containing ciclopirox 8%, efinaconazole 10%, or tavaborole 5% penetrate the nail plate to reach underlying fungal elements. These solutions work best when the infection affects less than half the nail surface and doesn’t involve the nail matrix (growth center). For a deeper understanding of these conditions, explore our definitive guide on onychomycosis.
Application typically continues for 48 weeks, requiring consistent daily application to achieve results. To enhance efficacy, gentle filing of the infected nail surface before application can improve medication penetration. Clinical studies show success rates between 15-40% for single nail infections treated solely with topical therapy, with higher success rates for superficial white onychomycosis compared to deeper infections.
The primary advantage of topical therapy remains its excellent safety profile and minimal drug interaction potential. This makes topical options particularly valuable for patients with multiple medical conditions or those taking medications that might interact with systemic antifungals. However, patient compliance with the lengthy treatment regimen often presents a significant challenge to successful outcomes. For more insights, explore this comparison of oral vs topical nail fungus treatment.
Oral Antifungals for Single Nail Treatment
When a single nail infection penetrates deeply or affects more than 50% of the nail plate, oral antifungal medications often become necessary. Terbinafine stands as the gold standard oral therapy for dermatophyte infections, with a typical treatment duration of 6-12 weeks for fingernails and 12-16 weeks for toenails. This medication achieves high concentration in the nail bed and continues working even after the treatment course ends.
Alternative oral options include itraconazole, which can be prescribed as daily therapy or as “pulse therapy” where medication is taken for one week each month for 2-3 months. Fluconazole, though not FDA-approved specifically for nail infections, is sometimes used off-label with weekly dosing. Each of these medications carries specific considerations regarding potential drug interactions and side effects, making proper patient selection crucial.
Laboratory monitoring of liver function becomes important with oral therapy, particularly for patients with pre-existing liver conditions or those taking multiple medications. Despite these considerations, oral therapy for single nail infections delivers substantially higher cure rates (50-70%) compared to topical options, with shorter overall treatment durations.
Success Rates of Monotherapy in Single Nail Cases
Single nail infection treatment with monotherapy demonstrates varied success rates depending on the specific approach. Clinical studies consistently show mycological cure rates of 50-70% for oral terbinafine monotherapy in isolated nail infections, making it the most effective single-agent treatment. Itraconazole follows with approximately 40-60% effectiveness, while fluconazole shows slightly lower rates at 30-50% for single nail cases.
Topical monotherapy demonstrates more modest results, with ciclopirox 8% achieving 15-30% complete cure rates and newer agents like efinaconazole reaching 15-40% effectiveness for isolated infections. The treatment success varies significantly based on the specific type of infection, with superficial white onychomycosis responding better than proximal subungual or total dystrophic forms. For those interested in a deeper understanding of treatment strategies, the clinical efficacy and management of onychomycosis treatments provides valuable insights.
Patient adherence significantly impacts these success rates, with studies showing a direct correlation between consistent application/ingestion and positive outcomes. Real-world effectiveness often falls below clinical trial results due to compliance challenges, particularly with topical treatments requiring daily application for nearly a year. Even with perfect adherence, single-agent therapy fails to produce complete resolution in a substantial percentage of cases, highlighting the resilient nature of nail infections.
Multiple Nail Infections Require a More Aggressive Approach
When infection spreads to multiple nails, treatment strategies must shift dramatically. Multiple nail involvement typically indicates a more robust fungal presence, potentially higher resistance to treatment, and often signals underlying health concerns that must be addressed concurrently. Dermatologists and podiatrists generally consider cases with three or more affected nails as requiring aggressive systemic therapy from the outset.
The presence of multiple infected nails significantly alters the treatment calculus by indicating a higher total fungal burden throughout the body. This increased pathogen presence requires medications that can reach therapeutic levels not just in one targeted area but throughout the nail system. Local topical treatments simply cannot address this widespread infection adequately.
Studies consistently show that when multiple nails are affected, the success rates of topical monotherapy plummet to below 10% compared to 15-40% for single nail cases. This stark difference demands a more comprehensive treatment protocol that combines multiple therapeutic approaches for any realistic chance of successful eradication.
Why Multiple Infections Are Harder to Treat
Multiple nail infections present unique treatment challenges stemming from several factors. First, the total fungal load is substantially higher, creating multiple reservoirs of infection that can cross-contaminate even successfully treated nails. Second, infections affecting multiple nails often indicate deeper penetration into the nail matrix, making complete eradication more difficult as the infection becomes embedded in the nail growth center.
The distribution pattern of infected nails provides crucial diagnostic information. For instance, when all toenails show infection but fingernails remain clear, this pattern suggests environmental exposure factors like footwear or community shower facilities as the primary transmission vector. Conversely, when both fingernails and toenails show infection, clinicians must consider potential immune system deficiencies or systemic conditions like diabetes that create favorable conditions for widespread fungal growth.
Perhaps most challenging is that multiple nail infections frequently demonstrate mixed pathogens—different fungal species or even combinations of fungal, bacterial, and yeast organisms affecting different nails simultaneously. This polymicrobial nature requires broader-spectrum therapeutic approaches, as treatments effective against one pathogen may have minimal impact on others. For more detailed insights, explore our definitive guide on onychomycosis.
Systemic Oral Medications as the Primary Solution
For multiple nail infections, oral antifungals become the cornerstone of effective treatment. Terbinafine (250mg daily) stands as the first-line therapy due to its superior nail penetration and high cure rates even in challenging cases. Clinical studies demonstrate mycological cure rates of 50-70% for multiple nail infections when terbinafine is administered for 12-16 weeks for toenails or 6-12 weeks for fingernails.
Itraconazole offers an effective alternative, particularly for non-dermatophyte infections that might respond poorly to terbinafine. This medication can be prescribed as continuous therapy (200mg daily) or as pulse therapy (200mg twice daily for one week per month, repeated for 3-4 months). The pulse therapy approach may improve patient adherence while reducing potential side effects and medication costs.
Both medications require liver function monitoring, especially in older patients or those with pre-existing hepatic concerns. Despite these monitoring requirements, the benefits of systemic therapy substantially outweigh the risks for multiple nail infections, as localized treatments simply cannot achieve therapeutic concentrations throughout all affected nails simultaneously.
Combination Therapy Necessity for Widespread Infections
When multiple nails exhibit infection, combination therapy becomes not just beneficial but necessary for optimal outcomes. Systematic reviews of clinical trials demonstrate that combination approaches increase cure rates from 50-70% with oral monotherapy to 70-80% when multiple treatment modalities are employed simultaneously. This synergistic approach addresses the multifaceted nature of widespread nail infections.
The most effective combinations typically pair oral antifungals with mechanical nail debridement, which physically removes infected nail material while improving medication penetration to the nail bed. For particularly resistant cases, adding topical antifungals creates a three-pronged approach that attacks the infection locally and systemically while reducing the physical burden of infected tissue.
Beyond improving cure rates, combination therapy potentially reduces treatment duration by accelerating the clearance of infected nail material. This time reduction matters significantly for patient compliance and satisfaction, as treatment adherence typically declines dramatically for courses extending beyond six months. For more insights on effective treatment strategies, explore this strategic treatment roadmap.
Treatment Duration Differences Between Single and Multiple Cases
The time commitment required for treating multiple nail infections substantially exceeds that of single nail cases. While isolated infections may respond to 12 weeks of oral therapy or 48 weeks of topical treatment, multiple nail involvement typically extends these timeframes by 30-50%. This extended duration reflects both the higher fungal burden and the varied growth rates of different affected nails. For more information on the different treatment options, you can explore this comparison of oral and topical treatments.
Treatment endpoints also differ significantly between single and multiple nail cases. With isolated infections, complete clearance represents a reasonable goal. However, with multiple nail involvement, success is often measured by improvement in the majority of affected nails rather than complete resolution in all nails. This modified expectation reflects the clinical reality that some nails—particularly thick, dystrophic toenails—may never achieve complete normalization even with extended therapy.
Patient education regarding these extended timeframes becomes crucial for treatment success. Healthcare providers must clearly communicate that visible improvement typically lags behind microbiological cure by several months, particularly in toenails which may require 12-18 months to grow out completely even after the infection has been eradicated. For those seeking more information, understanding the strategic journey to clear nails can be beneficial.
Treatment Success Factors: What the Research Shows
Multiple clinical studies have identified key factors that significantly impact treatment outcomes for nail infections. Among these, the total number of affected nails consistently emerges as one of the strongest predictors of treatment success, with cure rates declining proportionally as the nail count increases. A comprehensive analysis of 30 randomized controlled trials found that patients with more than 50% of their nails infected had cure rates approximately 30% lower than those with fewer affected nails, even when receiving identical treatment regimens.
Nail Type and Location Impact on Treatment Success
The specific nails affected by infection significantly influence treatment outcomes and required approaches. Fingernail infections generally respond more favorably to treatment than toenail infections, with studies showing cure rates 15-25% higher for fingernails across all treatment modalities. This difference stems from several factors, including faster fingernail growth rates (complete replacement every 4-6 months versus 12-18 months for toenails), better circulation to fingertips, and typically thinner nail plates that allow better medication penetration.
Among toenails, the great toenail presents particular challenges due to its thickness and slow growth rate. Infections in this location often require extended treatment courses and may benefit from adjunctive mechanical debridement to reduce nail plate thickness. Lateral toenails, while generally thinner, often experience trauma from footwear pressure, creating entry points for infection that can be difficult to completely resolve without addressing underlying biomechanical factors.
The anatomical pattern of infection across multiple nails also provides important clinical information. Asymmetric patterns often indicate external factors like trauma or specific exposure, while symmetric involvement of corresponding nails on both feet more commonly suggests systemic factors or genetic predisposition influencing susceptibility.
Infection Severity and Treatment Outcomes
The extent and depth of infection within each nail critically determines both treatment selection and likelihood of success. Distal lateral subungual onychomycosis affecting less than 50% of the nail plate typically responds well to topical therapy when only 1-2 nails are involved. However, once this same infection type spreads to multiple nails, oral therapy becomes essential for effective treatment. Proximal subungual onychomycosis—where infection begins near the cuticle—indicates deeper penetration into the nail matrix and almost universally requires oral medications regardless of how many nails show involvement.
Total dystrophic onychomycosis, where the entire nail unit becomes infected and distorted, represents the most challenging presentation. When multiple nails reach this advanced state, combination therapy with oral antifungals, aggressive debridement, and possibly temporary nail removal may be necessary. Clinical studies show that dystrophic involvement of three or more nails reduces cure rates by approximately 40% compared to more superficial infections affecting the same number of nails.
Patient Age and Health Status as Success Predictors
Age and overall health significantly influence nail infection treatment outcomes, particularly when multiple nails are affected. Patients under 50 typically experience 15-20% higher cure rates compared to older individuals, even with identical treatment protocols. This age-related difference stems from faster nail growth rates, stronger immune function, and better peripheral circulation in younger patients, all factors that enhance medication delivery and natural defense mechanisms.
Certain health conditions dramatically reduce treatment success rates for multiple nail infections. Diabetes stands as perhaps the most significant complicating factor, reducing cure rates by 30-40% due to compromised circulation and immune function. Similarly, patients with peripheral arterial disease, HIV/AIDS, or those taking immunosuppressive medications face substantially lower treatment success rates and higher recurrence risks.
Laboratory assessment before treatment initiation helps identify these potential obstacles to successful treatment. For patients with multiple comorbidities, extending treatment duration and implementing more aggressive combination approaches from the outset often provides the best chance for satisfactory outcomes.
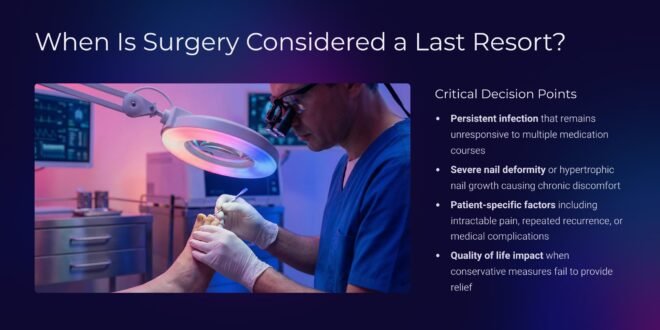
Advanced Treatment Options for Stubborn Infections
When multiple nail infections persist despite conventional oral and topical therapy, specialized interventions become necessary. These advanced options typically aim to increase medication penetration, physically remove infected tissue, or create environments inhospitable to fungal growth. While generally reserved for resistant cases, these approaches may be considered earlier for patients with multiple severe infections or those with underlying conditions that reduce conventional treatment efficacy.
Microdrilling Techniques: Improving Medication Penetration
Microdrilling creates tiny channels through the nail plate to enhance antifungal penetration directly to the infected nail bed. This minimally invasive procedure uses specialized instruments to create microscopic perforations without causing pain or damaging the underlying tissues. Clinical studies examining microdrilling combined with topical antifungals showed significantly improved results compared to medication alone, with one trial demonstrating a 35% improvement in cure rates for multiple infected nails.
The procedure takes just minutes per nail and can be performed in an outpatient setting without anesthesia. For patients with multiple thick, dystrophic nails resistant to conventional therapy, microdrilling dramatically increases medication delivery to infection sites that were previously inaccessible. Some patients report mild discomfort during the procedure, but serious complications remain extremely rare.
The primary limitation involves the need for specialized equipment and practitioner training, making this option less widely available than conventional treatments. However, for appropriate candidates with multiple resistant infections, the improved outcomes often justify seeking providers offering this specialized service.
Photodynamic Therapy Results for Multiple Nail Infections
Photodynamic therapy (PDT) combines specialized photosensitizing agents with targeted light exposure to destroy fungal cells within infected nails. This approach shows particular promise for multiple nail infections by addressing all affected nails simultaneously without systemic medication exposure. The process typically involves applying the photosensitizing solution to all infected nails, allowing penetration time, then exposing the nails to specific wavelengths of light that activate the solution to destroy fungal elements. For a comprehensive understanding of treatment options, you can explore oral vs topical nail fungus treatment strategies.
Research demonstrates that PDT offers comparable efficacy to oral antifungals for multiple nail infections, with mycological cure rates between 40-60% depending on infection severity. The primary advantages include minimal side effects, no drug interactions, and equal effectiveness regardless of the number of nails involved. This makes PDT particularly valuable for elderly patients or those with multiple medical conditions that complicate oral antifungal use.
The major drawbacks include limited availability, relatively high cost (often not covered by insurance), and the need for multiple treatment sessions typically spaced 1-2 weeks apart. Despite these limitations, PDT represents an important alternative for patients with multiple infected nails who cannot tolerate oral medications or have experienced treatment failures with conventional approaches.
Nail Plate Avulsion: When and Why It’s Necessary
Surgical or chemical nail avulsion—the complete or partial removal of the infected nail plate—becomes necessary in cases of severe multiple nail infections resistant to other treatments. This approach physically eliminates the bulk of infected material while providing direct access to the nail bed for topical medication application. Complete nail avulsion is typically reserved for the most severe cases, while partial avulsion targeting only the most heavily infected portions offers a less invasive alternative.
Clinical guidelines recommend considering nail avulsion for multiple nail infections when three or more nails show total dystrophic involvement, when matrix infection persists despite appropriate oral therapy, or when severe pain impairs daily activities. For chemical avulsion, 40% urea preparations applied under occlusion gradually dissolve the nail plate over 1-2 weeks, offering a less traumatic alternative to surgical removal.
Following avulsion, the exposed nail bed requires intensive topical antifungal treatment to prevent reinfection of the newly growing nail. While initially concerning to patients, temporary nail removal significantly improves outcomes in selected cases of severe multiple nail infections, with studies showing 70-80% success rates when combined with appropriate systemic and topical therapy.
Laser Treatments: Effectiveness in Clinical Trials
Laser therapy for nail infections has gained popularity as a non-medication alternative, particularly for patients with multiple infected nails who cannot tolerate oral antifungals. The procedure uses specific wavelengths that selectively heat and destroy fungal elements without damaging surrounding human tissue. Most protocols require 3-4 sessions spaced approximately one month apart, with each session treating all infected nails.
Clinical trial results for multiple nail infections show mixed outcomes, with mycological cure rates ranging from 30-60%. The effectiveness appears highest when laser treatment is combined with topical antifungals rather than used as monotherapy. Factors influencing success include nail thickness, infection depth, and specific laser parameters including wavelength and pulse duration.
The primary advantages include minimal pain, no systemic side effects, and simultaneous treatment of all affected nails. However, high out-of-pocket costs (typically $200-500 per session), limited insurance coverage, and the need for specialized equipment represent significant barriers. For appropriate candidates with multiple infected nails, particularly those with contraindications to oral medications, laser therapy provides a valuable alternative despite its limitations.
Combination Therapy: The Key to Multiple Nail Success
For multiple nail infections, combination therapy has emerged as the definitive standard of care. By simultaneously attacking the infection through different mechanisms, combination approaches overcome the limitations of individual treatments while capitalizing on synergistic effects. Research consistently demonstrates that combination protocols achieve 15-30% higher cure rates for multiple nail infections compared to any monotherapy approach.
Oral + Topical Medication Combinations
Pairing systemic and topical antifungals creates a powerful dual-pronged approach for multiple nail infections. This combination delivers medication both through the bloodstream and directly to the infection site, achieving higher local concentrations than either method alone. The most effective combinations typically pair oral terbinafine (250mg daily) with newer topical solutions like efinaconazole 10% or tavaborole 5%, applied to all affected nails.
Clinical studies demonstrate that this combination increases cure rates for multiple nail infections by approximately 15-20% compared to oral medication alone. The synergistic effect appears most pronounced when oral therapy is provided at full strength while topical applications continue for an extended period, often 4-6 months beyond the completion of oral medication. This extended topical application helps prevent recurrence while addressing residual fungal elements that may survive the oral treatment course.
For patients with mild liver concerns or multiple medications that might interact with oral antifungals, an alternative approach uses pulse-dosed oral medication (one week per month) combined with daily topical application. This modified regimen reduces systemic medication exposure while maintaining effectiveness for most multiple nail infections.
Procedural + Medical Approaches
Combining professional nail debridement with pharmaceutical therapy substantially improves outcomes for multiple nail infections. Mechanical debridement physically removes infected nail material, reducing the total fungal burden while creating pathways for better medication penetration. For maximum effectiveness, debridement should occur at 4-8 week intervals throughout the treatment course, with each session addressing all affected nails.
More advanced combinations incorporate specialized procedures with traditional medications. Microdrilling followed by topical antifungal application shows particularly impressive results for multiple thick toenail infections, with studies demonstrating 25-30% higher cure rates compared to topical treatment alone. Similarly, partial nail avulsion combined with oral antifungals creates direct access to the nail bed, dramatically improving medication delivery to the infection site. For more information on treatment options, explore our guide on oral vs topical nail fungus treatment.
These procedural-medical combinations often allow shorter overall treatment courses, typically reducing therapy duration by 30-40% while maintaining or improving cure rates. This reduced treatment time significantly enhances patient compliance and satisfaction—critical factors for successful management of multiple nail infections requiring months of consistent therapy.
Drug Synergy Benefits in Multi-Nail Cases
Different antifungal medications target various aspects of fungal cell function, creating potential synergistic effects when used in combination. Allylamines (like terbinafine) inhibit squalene epoxidase in fungal cell membranes, while azoles (like itraconazole) block ergosterol synthesis through different mechanisms. When combined thoughtfully, these medications attack fungal organisms at multiple vulnerability points simultaneously.
This multi-target approach proves particularly valuable for multiple nail infections, which often harbor diverse fungal populations with varied susceptibility profiles. Clinical studies demonstrate that combination therapy can effectively address mixed infections containing both dermatophytes and non-dermatophyte molds—a common scenario in patients with multiple infected nails. The synergistic effect also helps prevent the development of antifungal resistance, a growing concern in difficult-to-treat cases.
Beyond pharmaceutical synergy, combining medications with different application methods enhances overall effectiveness. For instance, oral terbinafine achieves high concentrations in the nail bed and growing nail plate, while topical solutions directly target the nail surface and surrounding tissue. This complementary coverage ensures no aspect of the infection escapes treatment attention, particularly important when multiple nails show different infection patterns simultaneously.
Cost vs. Benefit Analysis of Combination Treatments
The financial implications of combination therapy require careful consideration, particularly for multiple nail infections requiring extended treatment. While combination approaches typically increase initial treatment costs by 30-50%, they simultaneously reduce failure rates and recurrences that would necessitate retreatment. One pharmacoeconomic analysis demonstrated that despite higher upfront expenses, combination therapy proved more cost-effective for multiple nail infections by reducing the need for repeated treatment courses.
Insurance coverage varies significantly for different components of combination therapy. Most plans cover oral antifungals with prior authorization, but coverage for newer topical preparations remains inconsistent. Procedural interventions like professional debridement typically receive partial coverage when performed by podiatrists for patients with qualifying conditions like diabetes, but may require out-of-pocket payment when provided in dermatology settings.
For patients weighing treatment options, the total cost consideration should include not just medication expenses but also time investment, potential lost work, and quality-of-life impact from prolonged infection. From this comprehensive perspective, effective combination therapy often represents the most economical approach for multiple nail infections despite higher initial costs.
Preventing Recurrence and Reinfection
Successfully treating multiple nail infections represents only half the battle—preventing their return requires equal attention and diligence. Without appropriate preventive measures, studies indicate recurrence rates of 20-25% within two years of completing treatment. This risk increases substantially for patients with certain risk factors, making post-treatment prevention a critical component of comprehensive care.
Why Multiple Nail Infections Have Higher Relapse Rates
Multiple nail infections demonstrate substantially higher recurrence rates compared to single nail cases, with research showing approximately double the relapse frequency. This increased vulnerability stems from several factors unique to multiple nail involvement. First, when numerous nails have been infected, the likelihood of incomplete eradication in at least one nail increases significantly, creating a reservoir for reinfection. Even microscopically small amounts of viable fungal elements can repopulate and spread to previously cleared nails.
Second, multiple nail infections often indicate underlying susceptibility factors—whether immunological, circulatory, or genetic—that persist even after successful treatment. These predisposing factors create favorable conditions for reinfection from environmental sources or reactivation of dormant fungal elements. Patients with diabetes, peripheral vascular disease, or genetic susceptibility experience recurrence rates nearly three times higher than the general population.
Finally, multiple nail involvement frequently correlates with longer infection duration prior to treatment, allowing fungi to establish more deeply within the nail matrix and surrounding tissues. This deeper penetration increases the likelihood that some fungal elements remain viable despite seemingly successful treatment, eventually leading to clinical recurrence months or years later.
Essential Preventive Measures for Treated Nails
After successfully treating multiple nail infections, comprehensive preventive strategies become essential for maintaining long-term results. Daily foot hygiene practices form the foundation of prevention, including thorough drying between toes after bathing and regular application of antifungal powder to footwear and feet. Rotating between multiple pairs of shoes allows complete drying between wearings, eliminating the warm, moist environment fungi require for growth. For more information on effective treatments, you can refer to this strategic treatment roadmap.
Protective footwear practices significantly reduce reinfection risk. Wearing breathable socks made from moisture-wicking materials helps maintain drier conditions around nails, while avoiding barefoot walking in public areas like pools, showers, and locker rooms eliminates exposure to environmental fungal reservoirs. For individuals with occupational exposure to moisture or trauma, waterproof footwear with adequate toe box space prevents the microtrauma that creates entry points for reinfection.
Regular nail maintenance plays a crucial preventive role after treatment of multiple infections. Keeping nails trimmed straight across and avoiding aggressive cuticle manipulation preserves the nail’s natural protective barriers. For those with biomechanical issues contributing to repeated microtrauma, custom orthotics can redistribute pressure away from vulnerable nails, reducing injury-related infection opportunities.
Maintenance Therapy Options
Prophylactic medication regimens significantly reduce recurrence rates for patients with successfully treated multiple nail infections. Weekly application of antifungal topical solutions to all previously infected nails reduces recurrence by approximately 80% compared to no maintenance therapy. This preventive application typically continues for 6-12 months after apparent cure, with many dermatologists recommending indefinite maintenance for high-risk patients with multiple previous infections.
For those with severe recurrence patterns or significant risk factors, intermittent systemic therapy provides enhanced protection. This approach typically involves pulse-dosed oral antifungals (such as 200mg itraconazole daily for one week every 2-3 months) to suppress fungal reactivation or recolonization. While more intensive than topical maintenance, this strategy shows particular benefit for immunocompromised patients or those with anatomical factors that create ongoing vulnerability. For a detailed comparison, you can read more about oral vs topical nail fungus treatment.
Newer preventive options include antifungal nail lacquers that combine cosmetic benefits with prophylactic properties. These products create physical barriers against fungal invasion while delivering low-concentration antifungals to the nail surface. Though less studied than traditional maintenance approaches, early research suggests they may provide a convenient and acceptable option for long-term prevention, potentially improving compliance through their cosmetic benefits.
When to See a Doctor: Treatment Timeline and Expectations
Multiple nail infections rarely resolve spontaneously and typically worsen without appropriate intervention. Patients should consult healthcare providers promptly when multiple nails show discoloration, thickening, crumbling, or separation from the nail bed. Early assessment allows treatment initiation before infections become deeply entrenched, improving outcomes while potentially reducing treatment duration and intensity. Additionally, because multiple nail involvement often signals underlying health issues, timely evaluation may identify previously undiagnosed conditions requiring attention.
Signs Your Treatment Isn’t Working
While nail infections respond slowly to treatment, certain signs indicate therapy failure requiring reevaluation. If after 12 weeks of appropriate treatment no visible improvement appears in any affected nails, or if previously unaffected nails develop new infection signs, the current approach is likely inadequate. Similarly, worsening symptoms like increasing pain, drainage, or surrounding skin inflammation necessitate prompt reassessment regardless of treatment duration. For more information on treatment options, consider exploring the clinical efficacy and management of onychomycosis treatments.
Laboratory evidence of treatment failure includes positive fungal cultures from nail samples collected during therapy. For this reason, follow-up evaluations often include repeat mycological testing to verify treatment efficacy, particularly when clinical appearance remains concerning. When treatment failure occurs, comprehensive reevaluation should include medication adherence assessment, confirmation of the infecting organism, and evaluation for conditions that might impair response.
For multiple nail infections showing partial response—with some nails improving while others persist unchanged—treatment modification rather than complete strategy revision may suffice. Options include extending therapy duration for resistant nails, adding targeted interventions like partial nail avulsion for particularly stubborn infections, or incorporating adjunctive treatments to enhance medication penetration specifically to areas showing inadequate response.
What to Expect During the Recovery Process
Recovery from multiple nail infections follows a predictable timeline patients should understand to maintain realistic expectations. During the first 4-8 weeks of treatment, minimal visible improvement typically occurs despite effective therapy, as medications require time to reach therapeutic concentrations throughout infected tissues. Many patients notice reduced symptoms (like pain or drainage) before visible nail changes appear.
As treatment continues, clear nail growth typically begins at the proximal nail fold, gradually advancing forward as the nail grows. Complete clinical cure—defined as a normal-appearing nail—requires sufficient time for the entire infected portion to grow out and be replaced by healthy nail. This process takes 6-9 months for fingernails and 12-18 months for toenails, substantially longer than the actual medication course. For more information on treatment options, you can read about oral vs topical nail fungus treatment.
Even with successful treatment, previously infected nails may never return to completely normal appearance, particularly when long-standing infections have damaged the nail matrix. Setting appropriate expectations helps patients understand that residual nail thickening or minor discoloration may persist despite successful eradication of the infection. This distinction between cosmetic appearance and microbiological cure prevents unnecessary retreatment of successfully treated nails with merely cosmetic imperfections.
Frequently Asked Questions
The management of multiple nail infections generates consistent questions from patients seeking to understand their condition and treatment options. Addressing these common concerns helps patients develop realistic expectations while improving treatment adherence and outcomes. Healthcare providers should proactively discuss these topics during initial consultations to alleviate anxiety and enhance the therapeutic partnership.
Below are responses to the most frequently asked questions regarding multiple nail infection treatment, based on current clinical evidence and expert consensus guidelines.
How long does it take to treat multiple nail infections compared to single nail infections?
Multiple nail infections typically require 30-50% longer treatment duration compared to single nail cases. While a single infected fingernail might respond to 6 weeks of oral therapy, the same medication may need 8-12 weeks when multiple fingernails are involved. For toenails, standard 12-week regimens for single nail infections often extend to 16-24 weeks for multiple nail involvement. This extended duration reflects both the higher total fungal burden and the frequent need to address underlying systemic factors contributing to widespread infection. Complete visual clearance takes even longer—up to 18 months for toenails—as the nail must completely grow out after the infection is eradicated.
Can I use over-the-counter treatments for multiple nail infections?
Over-the-counter products generally prove inadequate for multiple nail infections. Clinical studies show OTC topical treatments achieve less than 5% cure rates for cases involving multiple nails, compared to 40-70% for prescription oral medications. While products containing ingredients like undecylenic acid, tea tree oil, or tolnaftate may help prevent spread to uninfected nails, they rarely resolve established multiple nail infections. The limited efficacy stems from poor nail plate penetration and insufficient antifungal potency against deeply embedded infections. For multiple nail involvement, consultation with a healthcare provider for prescription-strength therapy remains essential for successful outcomes.
Why did my nail infection spread to other nails despite treatment?
Infection spread during treatment typically occurs for several reasons. Insufficient medication strength or penetration represents the most common cause, particularly when using topical treatments alone for infections that require systemic therapy. Cross-contamination through shared nail instruments or inadequate hygiene practices can transfer fungi between nails despite ongoing treatment. Some patients experience spread due to inconsistent medication application, treating only visibly affected nails while overlooking early infection in others. Additionally, underlying health conditions that compromise immune function may allow infection progression despite appropriate therapy. Addressing these factors through comprehensive treatment approaches, improved hygiene practices, and management of underlying health conditions helps prevent further spread.
Are there any natural remedies that work for multiple nail infections?
Natural approaches show limited effectiveness for established multiple nail infections. While some natural compounds demonstrate antifungal properties in laboratory settings, clinical studies show minimal benefit for actual nail infections. Tea tree oil, perhaps the most studied natural option, shows approximately 10% effectiveness for mild single nail infections but negligible benefit for multiple nail involvement. Vinegar soaks, another popular remedy, may help prevent bacterial superinfection but show little effect on fungal organisms within nail tissue. These natural approaches may serve as helpful adjuncts to conventional treatment or for prevention after successful therapy, but they rarely resolve multiple nail infections when used alone. Patients should discuss any natural remedies with healthcare providers to ensure they don’t interfere with prescription treatments.
Will my insurance cover combination therapy for nail infections?
Insurance coverage for multiple nail infection treatment varies significantly between plans and providers. Most insurance programs cover oral antifungals with prior authorization demonstrating medical necessity, particularly when multiple nails are affected. However, coverage for newer topical prescription medications remains inconsistent, with many plans requiring documented failure of oral therapy before approving these often expensive alternatives. Procedural interventions like professional debridement typically receive coverage for patients with qualifying medical conditions (like diabetes) but may require out-of-pocket payment for others. Patients should work closely with healthcare providers and insurance representatives to determine specific coverage details for their planned treatment approach, as combinations of multiple therapies may involve different coverage structures under the same insurance plan.
Treating nail infections, especially when multiple nails are involved, requires patience, consistency, and the right therapeutic approach. By understanding the differences between single and multiple nail treatment requirements, patients can work more effectively with healthcare providers to achieve successful outcomes.
HealthyNails has been helping patients achieve fungal-free nails for over two decades with our comprehensive treatment programs designed specifically for challenging multiple nail infections.

 Nail Fungus Cures Instant Cures for Painful Nails and Fungus
Nail Fungus Cures Instant Cures for Painful Nails and Fungus