Key Points
- Jublia (efinaconazole) and Kerydin (tavaborole) are both topical prescription treatments for nail fungus, but Jublia offers a higher complete cure rate of 15-18% compared to Kerydin’s 6.5-9%
- Both treatments require daily application for a full 48 weeks before final results can be evaluated
- Topical treatments are a safer alternative to oral antifungals, as they have fewer systemic side effects and drug interactions
- Proper nail preparation and consistent application can significantly improve the success rates of both medications
- These prescription treatments can be expensive, with costs potentially reaching thousands of dollars for a complete treatment course
Nail fungus can be a stubborn, unsightly, and sometimes painful condition. If you’re considering your treatment options, prescription topical solutions have become effective alternatives to oral medications.
Choosing the best treatment strategy involves learning about how these modern topical drugs work, what outcomes to anticipate, and if the advantages outweigh the expense. This detailed guide compares two top FDA-approved topical treatments: Jublia and Kerydin.
Understanding Nail Fungus Infections
Onychomycosis, or nail fungus infections, is a condition that affects around 10% of the population and up to 50% of individuals over the age of 70. It usually starts as a white or yellow spot under the tip of the nail and progressively spreads deeper, leading to discoloration, thickening, and crumbling of the nail. If left untreated, it can cause pain and may spread to other nails or the skin.
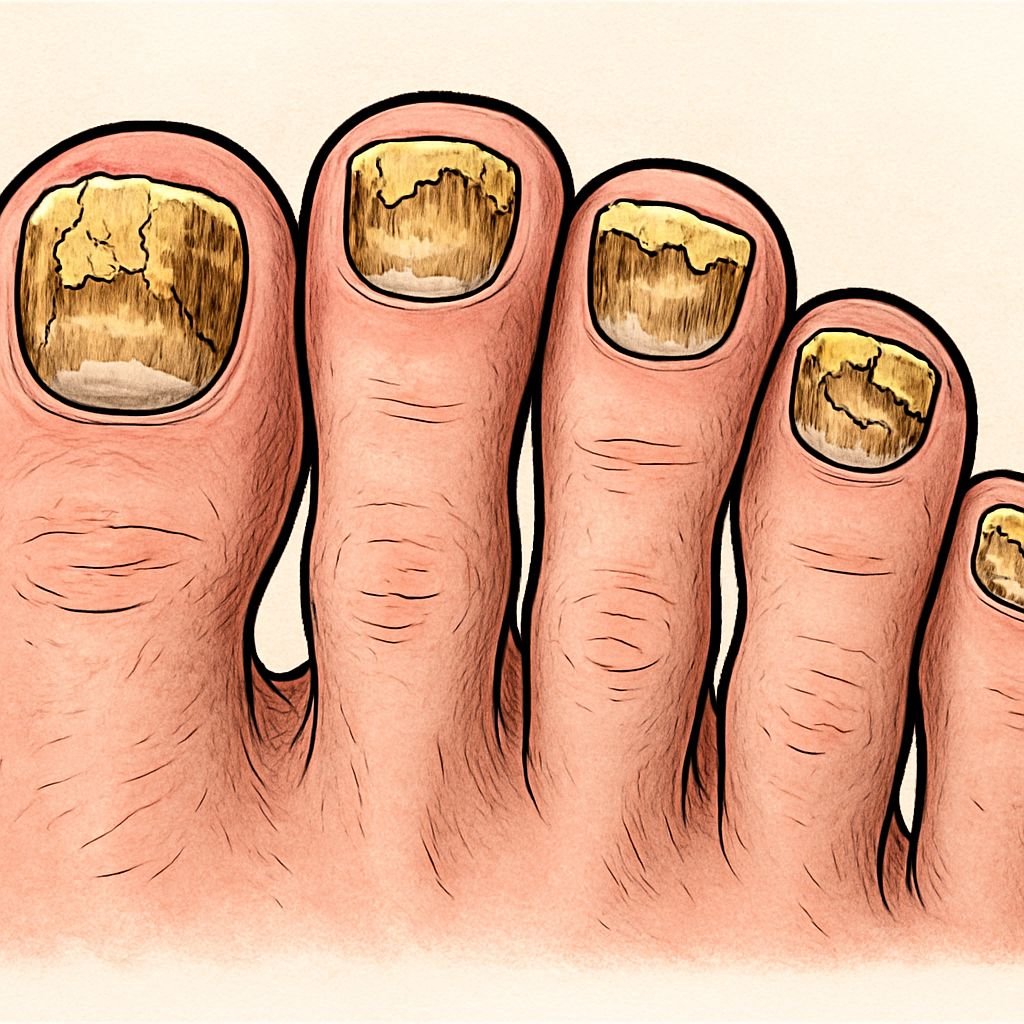
Nail infections are caused by fungi that love warm, damp places, which makes it hard to avoid them. You’re more likely to get an infection if you’re older, have poor blood flow, have a weak immune system, or if your feet are often wet. Athletes, swimmers, and people who use public showers are especially at risk. For those looking to understand more about prevention and treatment, here is a nail fungus treatment guide that might be helpful.
Older treatments have typically used oral antifungals such as terbinafine (Lamisil) and itraconazole (Sporanox). These treatments work throughout the entire body, but they can cause side effects and interact with other drugs. As a result, people have been looking for effective topical treatments that don’t have these problems.
Topical Prescription Solutions: The Latest Treatment Trend
The FDA has given its stamp of approval to two prescription-strength topical treatments designed to fight toenail fungus: Jublia (efinaconazole) and Kerydin (tavaborole). These medications are a big step up from earlier topical options, which had trouble getting through the nail plate effectively.
Today’s topical solutions are designed to deliver treatment straight to the infection site without spreading throughout the whole body. This targeted approach lessens the chance of systemic side effects and drug interactions that can happen with oral medications. For patients with liver problems, diabetes, or those on multiple medications, these topical options offer a beneficial alternative. Learn more about the differences between oral vs topical nail fungus treatment.
How Topical Treatments Fight Fungal Infections
Topical antifungal medications fight by directly targeting the fungal cells at the site of the infection. They infiltrate the nail plate to get to the nail bed where the fungus lives. The active ingredients mess with the fungal cell membranes or mess with important cellular processes, stopping the fungus from growing and reproducing. For a deeper understanding of the differences between oral and topical treatments, consider this comparison of oral vs topical nail fungus treatment.
Jublia and Kerydin both contain special carriers that boost their power to break through the thick, tough keratin structure of the nail. This ability to penetrate is a huge step up from older topical treatments, which often didn’t work because they couldn’t get to the root of the infection. For a comprehensive understanding of treatment options, check out this strategic treatment roadmap for nail fungus.
These topical solutions work best when applied consistently over a long period of time. Unlike oral medications, which work continuously through the bloodstream, topical treatments need to be applied every day to maintain therapeutic concentrations at the site of the infection.
Why Choose Topical Over Oral Antifungal Medications?
Topical treatments have a few clear benefits over oral treatments. The most important one is safety – you’re putting the medication right on the nail that’s infected, so you don’t have to worry about systemic side effects like liver damage that can happen with oral antifungals. This means that more people can use topical treatments, like people who have liver problems or are taking medications that could interact with oral antifungals.
Moreover, topical treatments do away with the need for regular liver function monitoring, something that’s usually required with oral antifungal therapy. They can be used for longer treatment periods without increasing systemic risks, which is beneficial for stubborn infections that require extended therapy.
There is a balance between effectiveness and convenience. Oral medications usually have higher cure rates (terbinafine has reported full cure rates of 38-76%), but they require strict adherence to shorter treatment protocols. Topical treatments require consistent daily application for almost a year, but can be safely continued if the initial treatment does not completely resolve the infection.
Getting to Know Jublia (Efinaconazole)
Jublia is a medication that uses efinaconazole as its active ingredient. This antifungal medication is part of the azole class of drugs. The FDA approved Jublia in 2014 to specifically treat onychomycosis of the toenail. The medication is a 10% concentration solution. It comes in a bottle that has a built-in brush applicator. This design is meant to help with precision when applying the medication.
Effectiveness: 6.5-9% Total Cure Rate
When studying Kerydin, clinical trials have shown total cure rates ranging from 6.5-9% after a year of treatment. While these numbers may seem low, they are a significant improvement over no treatment or over-the-counter options for stubborn nail fungus. Total cure is defined as both clinical cure (clear nail with no residual signs of infection) and mycological cure (negative fungal cultures), which is a stringent standard for success.
Typical Side Effects
Kerydin is generally well-tolerated with limited side effects. The most frequently reported problems include reactions at the application site such as redness, itching, swelling, burning, or irritation at the treated nail. These side effects usually stay localized to the application area and seldom necessitate discontinuation of treatment.
Since Kerydin is a topical treatment and is not absorbed into the system, it doesn’t usually cause the severe side effects that oral antifungals can. This makes it a good option for patients who have other health problems or are on other medications that could react with systemic antifungals.
Cost and Insurance Factors
Both Jublia and Kerydin can be quite expensive. Without insurance, a 4ml bottle of Kerydin (about a month’s supply) can cost anywhere from $500 to $700. Many insurance plans consider Kerydin a Tier 3 drug, which means you’ll likely have a high copay. There may be manufacturer discounts or patient assistance programs available to help with the cost, but you should check to see if you’re eligible for these programs before you start treatment.
Side by Side: A Look at Jublia and Kerydin
When you put Jublia and Kerydin side by side, a few key differences pop out that can help patients and doctors make the best choice. Both of these topical treatments for nail fungus are FDA-approved and require the same amount of time for treatment (48 weeks) and the same frequency of application (once a day). However, they have different efficacy rates and mechanisms of action, and sometimes they differ in cost.
Both Jublia and Kerydin are available as liquids, complete with applicators for easy application on infected nails. They have comparable safety profiles, with very little systemic absorption. This makes them suitable options for patients who can’t take oral antifungals due to potential liver effects or drug interactions.
But, how they get through the nail and fight off the fungus, which ultimately affects how well they work, is influenced by the differences in their chemical make-up. Knowing these differences can help you decide which one might be best for your particular situation.
Why Jublia Works Better (Efficacy Differences)
It’s been shown time and time again in clinical trials that Jublia works better than Kerydin in terms of completely curing patients. Jublia completely cures 15-18% of patients, while Kerydin only completely cures 6.5-9% of patients. This is a significant difference, and it’s likely due to the fact that Jublia is better at penetrating the nail and its method of action. Efinaconazole (Jublia) works by stopping the production of ergosterol, which is an important part of the cell membranes of fungi, while tavaborole (Kerydin) stops the production of protein by targeting the aminoacyl-transfer RNA synthetase of fungi.
Comparing Side Effects
The safety profiles of both Jublia and Kerydin are quite similar, with most side effects being localized. About 16% of patients reported application site reactions after using Jublia. The most common of these were ingrown toenails (2.3%), pain at the application site (2.2%), dermatitis at the application site (1.6%), and vesicles at the application site (1.6%). Kerydin has a slightly lower overall rate of application site reactions, but the difference is not significant enough to make the side effect profiles the deciding factor between these two medications for most patients. For more information on treatment options, check out this guide to your treatment options.
Price Breakdown and Worth Evaluation
When you weigh the cost against the benefits, Jublia’s higher success rate might make it worth the extra money. If a patient is footing the bill themselves, the extra $100-200 per bottle for Jublia could be a good investment considering the chances of a full recovery are almost double. However, the amount of coverage you get from your insurance can vary greatly, and in some cases, one drug might be covered more than the other, making it the more cost-effective choice despite the difference in effectiveness. Patients should look into their specific insurance coverage for both drugs before making a final decision.
What Patients Say
Patients seem to prefer Jublia, probably because it works better. Lots of patients say their nails look better, even if they aren’t completely cured. That helps them feel good about the treatment. Both drugs are expensive, and some people don’t like that. But more people like Jublia because it’s easy to use and it makes their nails look better. But everyone is different. Some people say Kerydin works great, even though it doesn’t work as well for most people.
Does the Price Justify the Results?
Given the high price tag of both Jublia and Kerydin, it’s reasonable to question their worth. With full cure rates of 15-18% for Jublia and 6.5-9% for Kerydin after a year of treatment, patients need to seriously consider whether the cost is worth the possible results.
For some people, especially those with severe infection, significant discomfort, or professional/social concerns about the appearance of the nail, the modest success rates may be worth pursuing. It’s crucial to keep in mind that these medications also provide mycological cure (elimination of the fungus) at higher rates than complete cure (perfect nail appearance plus negative cultures).
Choosing between these prescription topical treatments and alternatives like over-the-counter products (which lack strong evidence of effectiveness) or oral antifungals (which have higher cure rates but also carry more systemic risks) can be tricky. You should consider your individual health circumstances, budget, and treatment objectives when making this choice. For more information, check out this comparison of oral vs topical nail fungus treatments.
Why Are These Medications So Expensive?
There are a few reasons why Jublia and Kerydin are so pricey. For one, they are both relatively new medications that are still protected by patents. In addition, the process of researching, developing, testing, and gaining FDA approval for a new drug is very expensive, and the manufacturers need to make back their investment through the prices they charge for prescriptions.
Moreover, these are not your run-of-the-mill creams or lotions. These solutions use cutting-edge pharmaceutical technology to penetrate the nail plate effectively. They need specific carriers and delivery mechanisms to get to the site of infection beneath the nail. This contributes to their higher production costs and, ultimately, their higher retail price.
Calculating the Full Cost of Treatment
The total price of treatment goes beyond the cost per bottle. A full course of treatment requires 48 weeks of daily application, which means patients will need around 12 bottles (at 4ml per bottle, which lasts about 4 weeks each). Without insurance or discount programs, this could mean a total treatment cost ranging from $6,000 to $9,600, depending on the medication and local pricing. This large investment should be considered against the likelihood of success and the importance of getting rid of the infection to the patient.
What to Expect with Insurance Coverage
When it comes to insurance, coverage for these medications can vary a lot depending on your provider and plan. Many insurance companies put both Jublia and Kerydin in the Tier 3 or specialty medications category. This means they require prior authorization and can come with high copayments. Some insurance companies may even require proof that more affordable alternatives didn’t work before they’ll approve coverage. To explore treatment options and find out the specifics of your coverage, including copayment amounts, prior authorization requirements, and any quantity limitations, you should contact your insurance provider directly.
How to Choose the Right Treatment
- Think about how severe and widespread your nail fungus infection is
- Look at your medical history and any reasons why you might not be able to take oral antifungals
- Find out what your insurance will cover for both medications
- Think about whether you can commit to applying the medication every day for a full year
- Talk to your healthcare provider about what you can realistically expect from treatment
You should talk to a healthcare provider who knows your full medical history before you decide whether to use Jublia, Kerydin, or a different treatment. The best option for you will depend on things like how severe your infection is, whether you’ve tried other treatments before, any other health conditions you have, and any other medications you’re taking.
Oral antifungals like terbinafine are often the first choice for people with mild to moderate infections who don’t have any other health issues. This is because they tend to have higher cure rates and require a shorter course of treatment. However, if you have liver problems, are on multiple medications, or have other health conditions that make taking oral antifungals risky, then topical treatments are usually the better option, even though they don’t work as well. For more information, you can explore this comparison of oral vs topical nail fungus treatment.
Many doctors suggest a combined treatment approach, which includes both topical treatments and periodic debridement (professional thinning of the infected nail). This multi-pronged approach could potentially lead to better results than either treatment could achieve on its own.
Why Choose Jublia?
Jublia might be a better choice for patients who value a higher success rate and can handle the possible higher cost. It’s also ideal for those with a lot of nail involvement who need the superior penetration capabilities that Jublia provides. Patients who have tried other topical treatments without success might find that Jublia works for them because of its unique way of working and its superior ability to penetrate the nail.
Why Choose Kerydin
For patients who have experienced irritation or adverse reactions to Jublia, Kerydin may be a better option. Some people have found that Kerydin’s formulation causes less irritation at the application site. Another reason to consider Kerydin is if your insurance covers it more favorably than Jublia, potentially making it a more affordable option despite its lower efficacy rate. Patients with milder infections or those using Kerydin as part of a combination therapy approach (alongside professional nail debridement) may still find it effective.
Other Treatment Options to Consider
Apart from Jublia and Kerydin, there are several other treatments for nail fungus. Oral antifungals such as terbinafine (Lamisil) and itraconazole (Sporanox) have higher cure rates (38-76%) and require a shorter treatment duration, but they also have a higher risk of side effects and drug interactions. Ciclopirox nail lacquer (Penlac) is an older topical prescription option that is somewhat effective. Laser treatments are a newer technology that has shown promise in some studies, although the results vary widely. Natural remedies such as tea tree oil, vinegar soaks, and over-the-counter products have limited scientific evidence supporting their effectiveness, but they remain popular because they are easy to obtain and less expensive.
How to Get the Most Out of Your Treatment
While topical treatments may not always be successful, there are ways to increase their effectiveness. By using the medication correctly and consistently, you can create the best possible environment for the treatment to work. Research shows that patients who follow the instructions for application and stick to their treatment schedule are more likely to see positive results than those who are inconsistent with their treatment.
When you pair prescription topical treatments with consistent professional nail debridement (which is the thinning of the nail by a podiatrist or dermatologist), you can significantly boost the effectiveness of the treatment. The thinner nails allow the medication to better penetrate and reach the fungus that’s hiding beneath the nail plate. Some studies have shown that this combo approach can up the success rates by 15-20% compared to just using medication.
How to Prepare Your Nails Correctly
Before you apply Jublia or Kerydin, make sure your nails are clean and completely dry. You should wash the area with soap and water, then dry it thoroughly with a clean towel. If there’s any moisture trapped under or around the nail, it can dilute the medication and create an environment where the fungus can grow. If you want to get the most out of the medication, you might want to file the surface of the infected nails gently to remove any loose material and create a slightly rough surface that might help the medication absorb better. However, you should avoid filing aggressively because it could cause pain or bleeding, which could create opportunities for the infection to spread or make the inflammation worse.
Sticking to a Routine
Choose a time to apply your medication every day that works best for you, this way it’ll be easier to remember to do it. A lot of people choose to do it at bedtime, because it gives the medication several hours to soak into the nail without being disturbed. Make sure to apply the medication exactly as the instructions say to – for Jublia, use the brush that comes with it to apply it to the whole nail, the bottom of the nail (if you can reach it), and the skin right around the nail. For Kerydin, use the dropper to apply it to the toenail that’s affected, making sure to get the solution to drop between the nail and the nail bed if you can. For more detailed guidance, consider exploring this patient guide on treating nail fungus.
Try setting daily reminders on your phone or put the medication bottle somewhere you can easily see it as part of your daily routine. If you miss applications, it reduces how effective the medication is and it takes longer to see improvement. If you forget to apply a dose, put it on as soon as you remember, but don’t double up on applications to make up for missed doses.
Keeping Reinfection at Bay While Undergoing Treatment
Without the necessary precautions, fungal nail infections can come back even while you’re still under treatment. Maintain cleanliness and dryness in your feet, replacing your socks every day or more often if you have sweaty feet. Opt for socks that are made of natural fibers or special materials that wick away moisture. Give your shoes a day off in between use to let them dry out completely, and think about using antifungal powders in your shoes. When you’re in public places like gyms, pools, and shower rooms, always wear flip-flops or water shoes to avoid going barefoot. Sanitize your nail clippers and other pedicure tools after each use, and avoid sharing these tools with other people. These preventive measures are important during treatment and should be kept up even after treatment to prevent the infection from coming back.
Final Thoughts on Prescription Topical Nail Fungus Treatments
Jublia and Kerydin have significantly improved the topical treatment of nail fungus, providing viable options for patients who cannot take oral antifungals. While their complete cure rates might seem low – 15-18% for Jublia and 6.5-9% for Kerydin after a full year – they offer mycological cure (removal of the fungus itself) at higher rates and often show visible improvement in the appearance of the nail even without complete cure. Their excellent safety records make them suitable for long-term use with minimal risk of systemic side effects or drug interactions.
It’s important to consider the significant cost of these treatments, your own personal priorities, what your insurance will cover, and how much the nail fungus is affecting your quality of life. For a lot of people, using these prescription topicals along with proper nail care and professional debridement is the safest and most effective option. But, you should make the final decision with your healthcare provider. They can look at your specific situation and help you come up with a treatment plan that’s just right for you.
Common Questions
Those thinking about treating their nail fungus often have the same questions about what they can expect from topical prescription medications. These common questions address usual worries about how long treatment will take, changes they’ll have to make in their lives, and what can affect how successful the treatment is.
When can I expect to see results from Jublia or Kerydin?
Some changes may be noticeable within a few months, but it usually takes 6-9 months to see substantial results. The entire nail needs to grow out to reveal the healthier nail growing from the base, which can take a while due to the slow growth rate of toenails. Many people see the infected part of the nail slowly shrinking as the new, healthy nail grows from the cuticle. The full results can only be properly assessed after the full 48-week treatment course, as shown in clinical trials.
Even if you notice your nails looking better, make sure to keep using the treatment for as long as your doctor recommended. If you stop too soon, the fungus might come back. This is because there might still be some fungus under your nail, even if you can’t see it.
Can I wear nail polish while I’m treating my nail fungus with these medications?
The makers of both Jublia and Kerydin recommend not wearing nail polish while you’re treating your nail fungus. The polish can form a barrier that prevents the medication from getting through to the nail. If you have to wear nail polish for a special event, put on the medication first. Let it dry completely, which should take about 10 minutes. Then you can put on the polish. Take off the polish as soon as you can after the event and put the medication on again. For the best results, don’t wear nail polish at all while you’re treating your nail fungus. This will let the medication come into contact with the nail as much as possible.
Why do these medications have such low complete cure rates?
The low complete cure rates for these medications are due to several challenges involved in treating nail fungus. The nail plate is dense and hard for medications to penetrate, which limits direct contact with the fungus underneath. Toenails grow slowly (about 1mm per month), so even after the fungus is eliminated, it takes months for the damaged nail to grow out completely. Also, clinical trials define “complete cure” very strictly, requiring both perfect nail appearance and negative laboratory cultures. Many more patients achieve significant improvement or mycological cure (elimination of the fungus) without meeting all criteria for complete cure. Finally, reinfection during treatment can happen if preventative measures aren’t consistently followed.
Do Jublia or Kerydin have any drug interactions?
Topical treatments are great because they are absorbed systemically in minimal amounts, which means they have very few drug interactions. Neither Jublia nor Kerydin have any significant known interactions with other medications when used as directed. This makes them good choices for patients who are taking a lot of different medications or who have complex medical conditions that could be made worse by oral antifungals. But you should always let your healthcare provider know about all the medications, supplements, and topical products you’re using to make sure there aren’t any potential concerns that are specific to you. For more information on managing nail fungus, check out this guide on the clinical efficacy and management of onychomycosis treatments.
Why do treatments often fail?
Treatments usually fail due to inconsistent application, stopping treatment too soon, or the medication not reaching the infection site. If patients miss doses or stop treatment when the infection appears to be improving, the fungus often grows back. The success of treatment also depends on how severe and long-standing the infection is – it is generally harder to treat long-standing, extensive infections than newer, limited ones. Some patient factors, such as poor circulation, diabetes, or immune compromise, can make treatment less effective. Lastly, getting reinfected during treatment from contaminated footwear, nail tools, or exposure to fungi in public areas can undo the benefits of treatment. Patients can increase their chances of success by sticking to the application schedule, completing the full treatment course, and following preventive measures.
Before you decide on a treatment plan for nail fungus, it’s important to discuss your options with a healthcare provider who can evaluate your individual condition, medical history, and treatment objectives. They can guide you in deciding if Jublia, Kerydin, or a different treatment plan is best for you.

 Nail Fungus Cures Instant Cures for Painful Nails and Fungus
Nail Fungus Cures Instant Cures for Painful Nails and Fungus