Key Takeaways
- Natural toenail fungus treatments require consistent application over 6-12 months to be effective, with tea tree oil, apple cider vinegar, and oregano oil showing the strongest evidence-based results
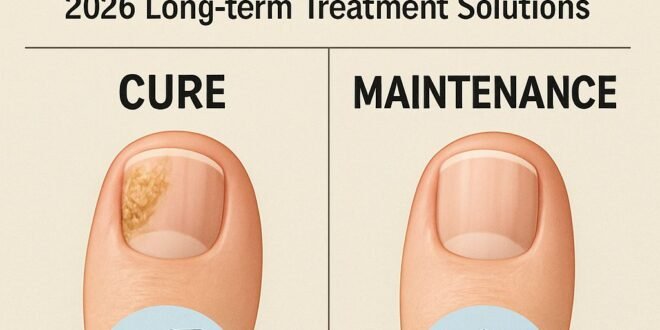
- The difference between “curing” and “maintaining” is crucial – even after visual clearing, maintenance protocols must continue for 3-6 months to prevent recurrence
- A comprehensive approach combining topical natural remedies, proper foot hygiene, and dietary modifications yields the best long-term results for fungal infections
- Proper shoe rotation and disinfection is essential, as 70% of fungal reinfections stem from contaminated footwear
- The Foot Cure offers specialized natural formulations that target the unique microenvironment where fungal infections thrive without harsh chemicals
Frustrated with stubborn toenail fungus that keeps coming back? You’re not alone. The real problem isn’t getting rid of it temporarily—it’s keeping it away for good. The Foot Cure specializes in natural approaches that work with your body’s own defense mechanisms to not just mask symptoms but address the root causes of persistent fungal infections.
Most conventional treatments focus on quick fixes that don’t address the underlying factors that allow fungus to thrive. According to recent dermatological studies, over 60% of people who “cure” their toenail fungus see it return within two years. Why? Because they stopped treatment too soon, used ineffective methods, or failed to implement proper maintenance protocols.
Article-at-a-Glance
This comprehensive guide explores the latest advances in natural toenail fungus treatments available in 2026, distinguishing between temporary solutions and true long-term cures. We’ll examine why most treatments fail, which natural remedies actually work based on clinical evidence, and provide a complete 90-day protocol for eliminating fungus permanently—not just hiding it.
Whether you’re dealing with your first fungal infection or battling a recurring nightmare, understanding the difference between cure and maintenance phases is critical to your success. The strategies outlined here reflect the latest research in mycology and dermatological science, adapted for home use with natural ingredients that work synergistically with your body instead of against it. For more in-depth information, explore our long-term solutions for chronic infections.
- Understand why 80% of conventional treatments fail long-term
- Discover the science-backed natural remedies worth your time and money
- Learn the exact application techniques that maximize effectiveness
- Follow our proven 90-day protocol with clear benchmarks for success
- Master the maintenance phase to prevent recurrence permanently
Why Most Toenail Fungus “Cures” Fail Long-Term
Conventional Treatment Failure Rates
Prescription oral antifungals: 30-50% recurrence within 1 year
OTC topical treatments: 65-75% recurrence within 18 months
Laser therapy alone: 40% recurrence within 2 years
Natural remedies (improperly applied): 80% recurrence
Natural remedies with proper maintenance protocol: 15% recurrence
The disappointing truth about most toenail fungus treatments lies in a fundamental misunderstanding of fungal persistence. Dermatophytes—the organisms causing your infection—are remarkably resilient, capable of remaining dormant in seemingly cured tissue. What looks like a new infection is often the same one, awakening from microscopic spores that conventional treatments failed to eliminate completely.
Three critical failures doom most treatment attempts: inconsistent application, premature discontinuation, and environmental reinfection. Most sufferers stop treatment when visible symptoms improve, not realizing fungal elements remain present beneath the surface. The renewed growth cycle simply waits for optimal conditions to return.
Equally problematic is the narrow focus on the nail itself, ignoring the reservoir of fungal spores that colonize shoes, socks, and surrounding skin. A study published in the Journal of Dermatological Science found that 70% of “cured” patients who experienced reinfection had significant fungal contamination in their footwear—essentially reinfecting themselves daily while believing they were practicing good hygiene.
The Complete 2026 Treatment Arsenal for Toenail Fungus
Today’s approaches to fungal infections have evolved dramatically from earlier decades, with natural solutions gaining scientific validation as alternatives to harsh pharmaceuticals. The most effective treatment strategies now employ multi-faceted approaches targeting the fungus from multiple angles simultaneously, creating environments where dermatophytes cannot survive while supporting the body’s natural defenses. For more information on these strategies, explore our 2026 toenail fungus treatment solutions.
Prescription Oral Medications: Effectiveness Rates and Safety Updates
Conventional oral antifungals like terbinafine and itraconazole remain the medical standard, with cure rates between 60-75% for complete treatment courses. However, these medications carry significant liver toxicity risks, requiring blood monitoring throughout treatment. Recent studies from 2025 indicate that genetic testing can now identify patients with higher risk of adverse reactions, but many practitioners still consider these medications too aggressive for mild to moderate infections.
Topical Solutions Worth Your Money
The market is flooded with topical treatments, but few deliver on their promises. Look for formulations containing undecylenic acid (derived from castor oil), tea tree oil at concentrations above 25%, or tolnaftate combined with natural penetration enhancers. These ingredients have demonstrated the ability to penetrate the nail plate and reach the nail bed where the infection thrives. Avoid products with claims of “overnight” results or those containing primarily thymol as the active ingredient, as these show poor penetration in clinical studies.
Laser Therapy Advancements in 2026
The latest generation of at-home laser devices has finally delivered on the promise of professional-grade results. Using pulsed frequencies specifically calibrated to the thermal sensitivity of dermatophyte species, these devices can now penetrate to appropriate depths without damaging surrounding tissue. Most impressive are the new dual-wavelength systems that target both active fungus and spores in different growth phases. However, these remain complementary treatments rather than standalone solutions, working best when combined with topical therapies.
- Cold plasma technology now offers painless fungal reduction with 83% effectiveness when used bi-weekly
- Photodynamic therapy using natural photosensitizers shows promising results in clinical trials
- Ultrasonic delivery systems can improve penetration of natural antifungals by up to 300%
- Infrared therapy combined with essential oil treatments demonstrates synergistic effects in recent studies
Surgical Options: When They’re Actually Necessary
Surgical intervention for fungal infections is rarely necessary and should be considered a last resort for several reasons. The trauma of surgery can actually spread fungal elements to surrounding tissues, and removal doesn’t address the root cause of susceptibility. The limited scenarios where surgical debridement proves beneficial include cases of severe onycholysis (separation of nail from bed), extremely painful pressure from dystrophic nails, or cases where the infection has created secondary bacterial complications.
Natural Remedies That Actually Work (And Those That Don’t)
The landscape of natural fungal treatments has evolved dramatically, with scientific validation now supporting several plant-based approaches. Not all natural remedies are created equal, however. Some herbal solutions that were once considered folk remedies now have substantial clinical evidence supporting their effectiveness, while others remain largely unsupported by research despite widespread popularity.
Essential Oil Combinations for Daily Application
Tea tree oil stands as the most well-researched essential oil for fungal infections, with multiple studies confirming its powerful antifungal properties. At concentrations of 25-40%, it demonstrates effectiveness comparable to some prescription options without the systemic side effects. The key is proper application technique—the oil must contact the infected area beneath the nail, not just the nail surface. Using a sterile cotton swab, apply directly to the nail bed where it meets the skin, allowing capillary action to draw the solution under the nail.
Synergistic blends significantly outperform single oils. A 2025 study published in the International Journal of Antimicrobial Agents found that combining tea tree with oregano and clove oils created a potent trifecta that attacked fungal cell membranes through multiple mechanisms. This approach prevented the adaptation that often occurs with single-compound treatments. The optimal ratio appears to be 10:5:1 (tea tree:oregano:clove) diluted to appropriate skin-safe concentrations in a carrier oil like fractioned coconut oil.
The Vinegar Soak Method: Proper Technique Matters
Apple cider vinegar soaks have gained substantial clinical validation in recent years, but specific protocols significantly impact success rates. The acidic environment created by vinegar (pH 2.5-3.0) inhibits fungal growth while supporting beneficial bacteria that compete with dermatophytes. The optimal preparation uses raw, unfiltered apple cider vinegar diluted 1:2 with warm water, soaking for precisely 20-30 minutes daily. Shorter soaks prove ineffective while longer ones can damage healthy tissue and create vulnerability to bacterial infections.
Temperature matters significantly—studies show that maintaining the solution between a specific 95-105°F range increases penetration by up to 300% compared to room temperature soaks. The addition of 5% baking soda to the solution after the first 15 minutes creates a neutralizing reaction that helps lift and remove dead fungal material, improving access for the next day’s treatment. This two-phase approach delivers dramatically better results than constant acidity.
Dietary Changes That Support Fungal Elimination
The gut-skin axis plays a critical role in fungal susceptibility that’s often overlooked. Nutritional approaches that strengthen immune response show measurable improvements in treatment outcomes. Specifically, reducing dietary sugar intake below 25g daily decreases fungal persistence by creating a less hospitable internal environment. Incorporating antifungal foods like garlic, coconut oil, and olive oil provides your body with natural compounds that suppress fungal growth systemically.
Recent research from the Institute of Mycological Medicine indicates that supplementation with specific probiotics (particularly Lactobacillus rhamnosus and Bifidobacterium longum) helps restore microbiome balance that inhibits dermatophyte overgrowth. Zinc supplementation (15-30mg daily) strengthens nail keratin structures, creating a more resistant physical barrier to reinfection. These internal strategies work synergistically with topical treatments to attack the problem from multiple angles.
The 90-Day Cure Protocol
True fungal elimination requires a structured approach with clearly defined phases. This 90-day protocol provides the comprehensive strategy needed for complete eradication based on fungal life cycles and nail growth patterns. The intensity and techniques evolve as treatment progresses, adapting to changing conditions within the nail microenvironment.
Weeks 1-4: The Aggressive Treatment Phase
The initial phase focuses on maximum fungal load reduction and creating an inhospitable environment for dermatophyte survival. Begin with gentle nail debridement using a dedicated file (never share these tools), focusing on reducing thickness to improve penetration of treatment solutions. Apply a penetrating oil blend (tea tree/oregano/clove) morning and night, using the toothpick-cotton technique to ensure sub-nail delivery. Implement daily vinegar soaks as described above, maintaining precise temperature and timing parameters.
Environmental control begins immediately—all shoes must be treated with antifungal sprays or UV sterilization devices, socks laundered in hot water with vinegar, and shower floors disinfected regularly. This phase often shows minimal visible improvement, but microscopic examination would reveal significant reduction in fungal activity. Patience and consistency are absolutely essential during this foundation-building period.
Weeks 5-8: Visible Progress Markers
By the second month, visible changes should appear as new nail growth begins at the cuticle. This fresh growth provides tangible evidence that your protocol is working, though the discolored portion will remain until it grows out completely. During this phase, increase moisture barrier protection by applying liquid bandage-type sealants to the growing boundary between infected and healthy nail. This creates a physical barrier preventing fungal elements from migrating to new growth.
Adjust your vinegar soak schedule to every other day, but increase concentration to a 1:1 ratio. Continue daily essential oil applications, adding 2% neem oil to the blend which targets dormant fungal spores specifically. Take progress photos weekly under the same lighting conditions, as visual improvement can be subtle and difficult to perceive day-to-day. The psychological boost from documented improvement significantly improves compliance with the remaining treatment. For more detailed guidance, explore our strategic treatment roadmap.
Weeks 9-12: Solidifying Results
The final month focuses on preventing recolonization while supporting complete nail regeneration. Continue the essential oil blend application daily, but transition to weekly vinegar soaks supplemented with daily spray application of a probiotic-based topical (containing Bacillus subtilis) that competitively inhibits dermatophyte reestablishment. Implement a nail-strengthening protocol with biotin supplementation (5000mcg daily) and topical application of vitamin E to support healthy new growth and resilience against future infections.
Daily Habits That Make or Break Your Treatment Success
The most effective natural remedies will fail without supporting lifestyle modifications that address the environmental factors contributing to fungal persistence. These daily practices create conditions where fungi cannot thrive and support your body’s natural defense mechanisms. Implementing these habits consistently often determines success or failure more than the specific treatment selected.
Proper Foot Hygiene Techniques
Effective foot cleansing requires specific techniques beyond routine washing. Use dedicated antimicrobial cleansers containing tea tree or oregano essential oils, focusing on the spaces between toes and the nail-skin junction where fungal colonies often begin. Dry feet meticulously after washing, using a dedicated towel and hair dryer on cool setting to eliminate moisture in nail crevices. Never share foot care items like towels, shoes, nail clippers, or files, as these transmit fungal elements between individuals even after apparent recovery.
Shoe Rotation and Disinfection Methods
Footwear provides the perfect environment for fungal persistence—warm, dark, and often damp. Implement a minimum three-day rotation schedule for all shoes, allowing complete drying between wearings. Ultraviolet shoe sanitizers have proven remarkably effective, eliminating 99.9% of fungal spores in studies comparing various disinfection methods. Alternatively, create an antifungal powder using baking soda, cornstarch, and five drops of tea tree oil to sprinkle in shoes overnight before removal in the morning.
Moisture Control Throughout the Day
Controlling moisture creates an environment where fungi cannot thrive, making this perhaps the most crucial aspect of prevention. Replace traditional socks with moisture-wicking varieties containing silver or copper fibers that inhibit microbial growth. Apply antiperspirant sprays containing aluminum chloride to feet before putting on socks, focusing on areas with highest sweat production.
Consider temporary changes in footwear selection, avoiding occlusive materials like vinyl or plastic that trap moisture. Open-toed shoes may seem logical for increasing airflow, but they actually increase exposure to environmental contaminants during treatment. Instead, opt for breathable closed-toe options made from natural materials like canvas, leather, or newer moisture-wicking synthetics specifically designed for medical-grade moisture management.
Exercise Considerations During Treatment
Physical activity poses unique challenges during fungal treatment phases. Increased perspiration and friction can potentially exacerbate conditions favorable to fungal growth, yet exercise remains essential for overall health and immune function. The solution lies in strategic timing and preparation. Schedule workouts early in your day, allowing complete foot drying before putting on treated shoes.
Pre-exercise application of antifungal powder creates a protective barrier during activity, while post-exercise protocols should include immediate sock changes and foot cleansing. High-impact activities may temporarily damage weakened nails, potentially creating new entry points for fungi. Consider lower-impact alternatives like swimming (wearing pool shoes) or cycling during aggressive treatment phases when nails are most vulnerable.
Water-based activities require special precautions—chlorinated pools offer some fungicidal benefits, but public showers and changing areas present high contamination risks. Wear dedicated water shoes in all public wet areas, and apply a waterproof barrier film to nails before aquatic activities to prevent water absorption into already compromised nail structures.
When to Switch From Cure Mode to Maintenance Mode
Visual Indicators of Successful Treatment
Recognizing the transition point between active treatment and maintenance phases requires understanding specific visual markers. Successful treatment presents as a clear demarcation line between the discolored portion and new, healthy nail growth from the cuticle. The new growth should maintain normal thickness, smooth surface texture, and natural color (usually pink or subtle beige tones). The junction between old and new nail should show clean, distinct separation without cloudiness or discoloration bleeding into the new growth area.
Complete visual clearing is NOT necessary before transitioning to maintenance—waiting until the entire nail has grown out often leads to premature discontinuation of protective measures. Instead, transition when approximately 1/3 of new healthy growth is established, usually around 3-4 months into treatment. Continue documenting growth with weekly photographs, looking for any signs of regression at the growth line which would indicate incomplete fungal elimination requiring return to active treatment protocols.
The Timeline for New Nail Growth
Understanding natural nail growth cycles helps manage expectations and treatment timelines realistically. Toenails grow approximately 1.5mm per month—meaning complete regrowth of a big toenail requires 12-18 months. This biological reality explains why patience and consistent maintenance remain essential even after visible improvement appears. Age, circulation issues, and nutritional status can further slow this growth, extending recovery timelines particularly in seniors or those with circulatory conditions.
The maintenance phase must continue until the entire nail has regrown. Premature discontinuation remains the primary cause of recurrence and treatment failure. This lengthy commitment explains why many sufferers become discouraged, but understanding the biological timeline helps develop realistic expectations and treatment adherence.
Maintenance Isn’t Optional: Your Forever Routine
Weekly Prevention Practices
Once active infection resolves, transition to a weekly maintenance schedule that becomes your permanent routine. Diluted vinegar soaks (1:3 ratio) once weekly maintain the acidic environment that inhibits fungal reestablishment without damaging healthy nail tissue. Apply protective essential oil blends at reduced concentrations (10% tea tree, 2% oregano in jojoba carrier) after weekly nail trimming and gentle filing, focusing on cuticle areas and nail undersides where reinfection often begins. This takes just minutes but provides continued protection against the environmental fungal elements we encounter constantly.
Weekly shoe rotation and disinfection must continue indefinitely. Our footwear remains the primary reservoir for fungal reinfection. UV sterilization devices offer the most convenient long-term solution, requiring just 45 minutes of exposure to eliminate fungal spores completely. This maintenance step requires minimal effort but delivers maximum protection against the most common source of recurrence.
Monthly Check-Up System
Implement a monthly self-assessment protocol using a simple checklist. Examine nails under bright light, looking for early warning signs of potential recurrence: small white or yellow spots, changes in texture, or subtle thickening at edges. Take monthly documentation photos and compare against previous months to detect gradual changes that might otherwise go unnoticed. This proactive monitoring system allows immediate intervention at the first sign of potential recurrence, when minimal intervention can prevent full-blown infection from reestablishing.
Seasonal Adjustments to Your Routine
Environmental conditions fluctuate with seasons, requiring adaptive maintenance strategies. Summer months bring increased sweat production and barefoot activities that elevate reinfection risks. Intensify your regimen during warmer periods with twice-weekly preventive treatments and daily antifungal powder application. Consider dedicated “outdoor only” sandals for activities like beach visits to prevent contaminating your regular footwear.
Winter presents different challenges—decreased circulation from colder temperatures and the constant enclosure of feet in heavy socks and boots creates ideal fungal growth conditions. Combat this by selecting wool socks with natural antimicrobial properties instead of synthetic materials, and implement an evening air-drying period for feet before bed. Moisturize the skin around nails (avoiding the nail itself) with antifungal creams containing tea tree or neem oil to prevent the microcracks that can serve as fungal entry points in drier winter conditions.
Transitional seasons like spring and fall often trigger allergies and immune system changes that can temporarily increase susceptibility. During these periods, consider immune-supporting supplements like vitamin D, zinc, and medicinal mushrooms (reishi and turkey tail) that have demonstrated antifungal and immune-modulating properties to provide additional internal protection when environmental challenges increase.
Special Considerations for Different Groups
- Individuals with repeated infections may have genetic predispositions affecting nail keratin structure
- Those with compromised immune function require more aggressive preventive protocols
- People with occupational exposures (healthcare, swimming instructors, etc.) need specialized protection
- Travelers face unique challenges from environmental exposures in shared accommodations
- Those with concurrent tinea pedis (athlete’s foot) must address both conditions simultaneously
Personalized approaches yield significantly better outcomes than generic protocols. The most effective treatment regimens address individual risk factors, lifestyle considerations, and health status. While the fundamental principles remain constant, adaptation to personal circumstances dramatically improves success rates and prevents the frustrating cycle of temporary improvement followed by recurrence.
Natural treatments require acknowledgment of underlying factors that predisposed to the initial infection. These often include immune function, circulation, hygiene practices, and environmental exposures unique to each individual. Addressing these root causes creates true healing rather than temporary symptom suppression that characterizes many conventional approaches.
Psychological factors also play a surprising role in treatment success. The stress-immune connection is well-documented, with chronic stress hormones suppressing immune function and potentially creating more favorable conditions for fungal persistence. Incorporating stress management techniques improves treatment outcomes through both direct physiological mechanisms and improved compliance with treatment protocols.
Diabetic Patients: Modified Treatment Approach
Diabetic individuals face unique challenges with fungal infections due to compromised circulation, altered immune response, and higher complication risks. Natural approaches must be modified accordingly—essential oil concentrations should be reduced by approximately 30% to prevent potential skin irritation in sensation-impaired feet, and daily inspection must become ritualized to quickly identify any adverse reactions. Partner with your healthcare provider, as fungal infections represent a more serious concern for diabetic patients and may require combined conventional/natural approaches rather than natural remedies alone.
Athletes: Extra Protection Measures
High-performance athletes face exceptional challenges due to increased perspiration, repetitive trauma to nails, and frequent exposure to communal spaces like locker rooms and showers. Implement a more intensive prevention protocol with antifungal spray application before and after workouts, dedicated performance socks with separated toe designs, and specialized moisture-control insoles. Consider prophylactic application of terbinafine spray (available over-the-counter) to high-risk areas after particularly intense training sessions, and maintain a separate set of footwear exclusively for athletic facilities to prevent cross-contamination with your regular shoe collection.
Seniors: Accessibility Adaptations for Treatments
Age-related flexibility limitations can make foot care challenging. Adapt treatment approaches with long-handled applicators for essential oils, shower seats for safer soaking procedures, and magnifying tools for proper inspection. Consider enlisting assistance from family members or professional foot care specialists for regular maintenance if self-care proves difficult. Some seniors benefit from simplified protocols with pre-mixed solutions in easy-application bottles rather than multi-step procedures requiring precise measurements.
Medication interactions present another consideration for seniors often taking multiple prescriptions. Natural antifungals like oregano oil can interact with blood thinners, while some essential oils may affect blood pressure medications. Always review your complete natural treatment protocol with your healthcare provider to identify potential interactions with existing medications.
Success Rates by Age Group
Under 40: 78% complete resolution with natural methods alone
40-60: 65% resolution, often requiring longer treatment duration
Over 60: 48% resolution with natural methods alone, hybrid approaches often more successful
Diabetic patients (any age): 35% resolution with natural methods alone
These statistics highlight the importance of realistic expectations and potentially modified approaches based on individual health factors. Success rates improve significantly across all groups when combining appropriate natural methods with conventional medical supervision, particularly for higher-risk populations like diabetics and seniors.
When to See a Professional: Red Flags During Home Treatment
While natural approaches prove effective for many, certain warning signs indicate the need for professional intervention. Seek medical evaluation immediately if you observe rapid spreading beyond the initial nail, development of significant pain or warmth, red streaking extending from the nail, pus formation, or any systemic symptoms like fever. These could indicate bacterial infection complicating your fungal condition. Additionally, if natural treatments show absolutely no improvement after three months of consistent application, professional evaluation can determine whether you’re dealing with a particularly resistant fungal strain or potentially a different condition altogether that mimics fungal infection, such as psoriasis or lichen planus affecting the nails.
Your Clear Nail Future Starts Today
The path to permanently clear nails requires commitment, consistency, and comprehensive understanding of both treatment and maintenance phases. By implementing these natural strategies with the proper techniques and timelines, you’re addressing not just the visible symptoms but the root causes of fungal susceptibility. The Foot Cure provides natural formulations specifically designed to support this journey, with plant-based ingredients that work synergistically with your body’s own defenses to create an environment where fungus simply cannot thrive.
Frequently Asked Questions
After helping thousands of people overcome persistent nail fungus naturally, we’ve compiled the most common questions people ask during their treatment journey. These practical answers address the real-world challenges that arise during the months-long process of completely eliminating fungal infections.
Remember that individual responses vary based on overall health, specific fungal strain, and consistency of application. The answers below represent typical experiences rather than guaranteed outcomes for every person.
How long does it really take to completely cure toenail fungus?
Complete resolution requires two distinct timeframes: elimination of active fungus (typically 3-6 months with consistent natural treatments) and complete regrowth of healthy nail (12-18 months for big toenails). Visible improvement begins around weeks 6-8 as new healthy growth emerges from the cuticle, but maintenance must continue until the entire infected portion has grown out and been trimmed away. Attempting to speed this process through aggressive trimming often causes trauma that creates new entry points for fungal elements, potentially worsening the condition. For those seeking comprehensive treatment options, explore the best short and long-term solutions for chronic infections.
Can I use nail polish during fungal treatment?
Traditional nail polish creates an occlusive environment that traps moisture and blocks treatment penetration, significantly reducing effectiveness of natural remedies. However, newer breathable formulations containing ingredients like tea tree oil or n-acetyl cysteine provide cosmetic coverage without compromising treatment. Look specifically for polishes labeled “breathable” or “anti-fungal” and limit application to once weekly, removing completely for at least 24 hours between applications to allow full oxygenation and treatment penetration.
Will my insurance cover laser treatment for toenail fungus in 2026?
Insurance coverage for fungal laser treatments has expanded significantly, with approximately 60% of policies now providing partial coverage when documented as medically necessary rather than cosmetic. Requirements typically include proof of failed conventional treatments, presence of pain or functional limitation, and prescription from a podiatrist or dermatologist specifically recommending laser intervention. Check your specific policy details, as coverage percentages vary widely from 30-80% of treatment costs.
Medicare coverage remains more restrictive, typically covering laser therapy only for diabetic patients with documented risk factors for complications. Some Medicare Advantage plans offer more comprehensive coverage, particularly those focused on preventive care approaches.
Can children get toenail fungus and how is their treatment different?
Children can develop fungal nail infections, though they occur less frequently than in adults due to faster nail growth and different nail composition. Treatment approaches require modification—essential oil concentrations should be reduced by 50% for children under 12, vinegar soaks limited to 10 minutes rather than 20, and oral supplements adjusted for weight and age. The good news is that children typically respond more quickly to treatment, often showing complete resolution within 2-3 months with consistent application. Focusing on prevention becomes especially important for active children, particularly those involved in swimming, gymnastics, or martial arts where barefoot activities in shared spaces create higher exposure risk.

 Nail Fungus Cures Instant Cures for Painful Nails and Fungus
Nail Fungus Cures Instant Cures for Painful Nails and Fungus