Key Takeaways
- Up to 1 in 10 salon-goers may experience a fungal nail infection without proper precautions, making prevention crucial for foot health.
- Autoclave sterilization is the gold standard for nail tool sanitation – always ask if your salon uses this medical-grade method.
- Morning appointments significantly reduce your infection risk as foot baths and tools are typically at their cleanest early in the day.
- Bringing personal pedicure tools eliminates cross-contamination risk and is recommended by leading podiatrists.
- Post-pedicure home care including thorough drying and using antifungal powder can prevent fungal spores from gaining a foothold.
That relaxing pedicure shouldn’t come with an unwanted souvenir – nail fungus. Every year, thousands of salon-goers unknowingly expose themselves to fungal infections during routine pedicures. At Pinnacle Dermatology, we’ve seen firsthand how a single visit to an unsanitary salon can lead to months of treatment for stubborn nail fungus. The good news? With proper awareness and a few preventative steps, you can enjoy your pampering without the health risks.
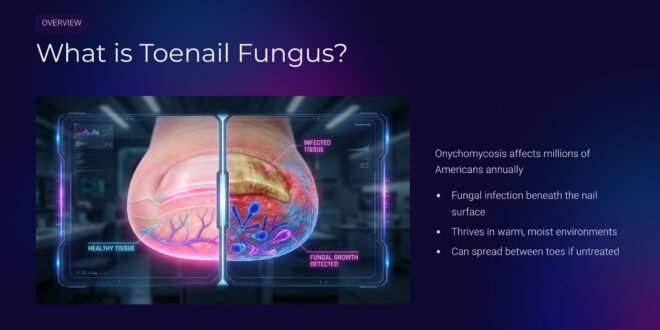
Nail fungus (onychomycosis) thrives in warm, moist environments – precisely the conditions found in many nail salons. When tools aren’t properly sterilized between clients or foot baths aren’t thoroughly disinfected, fungi can easily transfer from one person to the next. What begins as a small white or yellow spot under your nail can quickly develop into a painful, unsightly infection that’s notoriously difficult to treat.
Nail Fungus Lurks in Unsafe Salons: What You Need to Know
The environment of a nail salon creates the perfect storm for fungal transmission. Warm water in foot baths, shared tools, and the constant flow of clients provide ample opportunity for fungi to spread. These microscopic organisms can survive on surfaces for days, waiting for the opportunity to infect a new host through tiny cuts or nail separations you might not even notice.
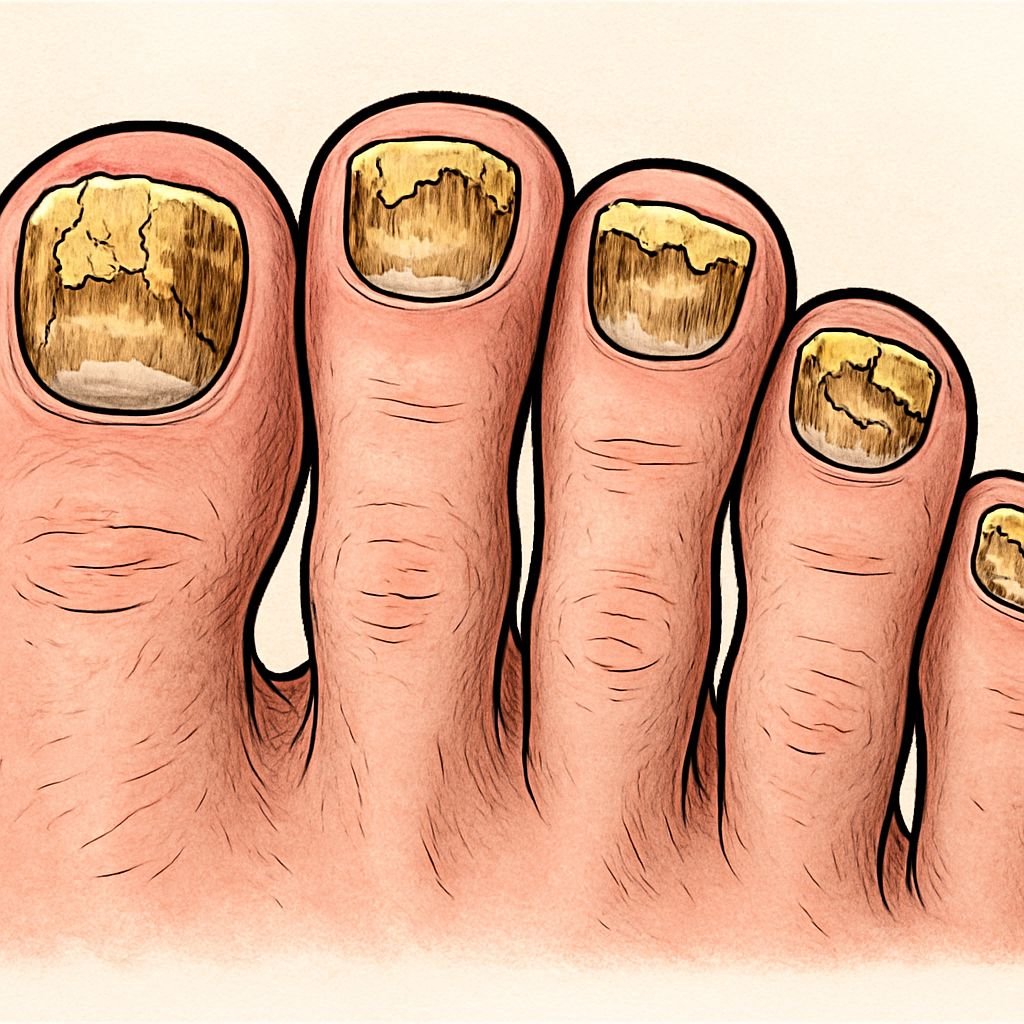
Fungal nail infections don’t just affect appearance – they can become painful as the nail thickens, crumbles, and potentially separates from the nail bed. For people with diabetes or compromised immune systems, what starts as a cosmetic concern can evolve into a serious health risk. Prevention is always easier and more effective than treatment, which often requires months of oral or topical antifungal medications.
Many salons prioritize quick turnover rather than thorough cleaning between clients. When choosing a salon, remember that cleanliness isn’t just about appearances – it’s about practices you might not immediately see. Medical-grade sterilization methods and single-use tools are your best defense against picking up an unwanted infection during your self-care routine. For more information on maintaining nail health, check out this guide to preventing toenail fungus recurrence.
7 Warning Signs of an Unsanitary Nail Salon
Your first line of defense against nail fungus begins before you even sit down for your pedicure. Train your eyes to spot these telltale signs of poor hygiene practices that increase your risk of infection.
Dirty Foot Baths and Standing Water
Foot baths should be thoroughly disinfected between each client – no exceptions. Look for visible debris in corners, stains on surfaces, or cloudy water. Quality salons disinfect with hospital-grade solutions and run cleaning cycles on jetted tubs between every client. If you notice the technician only giving the tub a quick rinse or spray, that’s a major red flag for potential fungal contamination.
“The jets in pedicure tubs can harbor bacteria and fungi for weeks if not properly cleaned. We recommend clients request to see the cleaning log for foot baths and ask about the specific disinfectant used.” – American Podiatric Medical Association
Reused Files and Buffers
Porous items like emery boards, buffers, and wooden tools cannot be adequately sterilized between clients. These items should be single-use only or dedicated to you personally. If you see a nail technician pull used files from a drawer rather than opening new ones, politely request fresh tools or consider finding another salon. These porous surfaces can harbor fungal spores even after surface cleaning. For more information on maintaining healthy nails, check out this strategic journey to clear nails.
Unsterilized Metal Tools
Metal implements like nippers, clippers, and pushers must undergo proper sterilization – not just a quick dip in disinfectant. Look for an autoclave (a medical sterilization device) on the premises or sealed packages of pre-sterilized tools being opened in front of you. Blue liquid disinfectant alone isn’t sufficient to kill all fungal spores and bacteria that cause nail infections.
Poor Ventilation and Strong Chemical Smells
While not directly related to fungal infections, a salon’s air quality speaks volumes about its overall hygiene standards. Proper ventilation systems remove airborne contaminants and chemical fumes. Overwhelming chemical odors often indicate poor air circulation, which can allow airborne particles – including fungal spores – to settle on surfaces throughout the salon.
Visibly Unclean Workstations
Counters, chairs, and floors should be clean and free of dust and debris from previous clients. Nail clippings, skin particles, or spilled products are breeding grounds for microorganisms. Additionally, technicians should be wiping down all surfaces between clients with appropriate disinfectants.
Quality salons maintain strict cleaning schedules for all surfaces and have visible evidence of their sanitation protocols. If you notice dried polish on tables, dust on shelves, or unswept floors, consider these warning signs of potentially dangerous shortcuts in more critical sanitation practices.
Technicians Who Don’t Wash Their Hands
Hand hygiene is fundamental in infection prevention, yet it’s often overlooked in busy salon environments. A professional nail technician should wash their hands before beginning work on a new client and should wear a fresh pair of gloves, especially when handling feet. This simple practice dramatically reduces the risk of cross-contamination between clients, a crucial step in preventing nail fungus infections.
Pay attention to whether your technician touches common surfaces—like phones, doorknobs, or payment terminals—during your service without changing gloves or rewashing their hands. These brief moments of cross-contamination can transfer fungi and bacteria directly to your nails and skin.
Missing Licenses and Certifications
Reputable salons proudly display their state licenses and individual technician certifications. These credentials indicate that the establishment and its staff have received proper training in sanitation protocols and safety standards. If you don’t see these displayed prominently, ask to see them. Their absence might signal that the salon is cutting corners in other important areas, including cleanliness.
Your Pre-Appointment Safety Checklist
Being proactive before you even step into the salon can significantly reduce your risk of contracting nail fungus. Taking a few precautionary steps can mean the difference between a relaxing experience and months of dealing with a fungal infection.
Consider your pedicure appointment as a partnership between you and the salon—both parties share responsibility for keeping your feet healthy and fungus-free. While a quality salon maintains rigorous sanitation protocols, your awareness and preparation can provide an extra layer of protection.
Research the Salon’s Reputation
Before booking, check online reviews specifically mentioning cleanliness and sanitation practices. Look for mentions of individual tool packets being opened in front of clients or autoclave sterilization. Salons with higher price points often (though not always) invest more in proper sanitation equipment and procedures.
Don’t hesitate to call ahead and ask specific questions about their sanitation protocols. A reputable salon will welcome these inquiries and proudly explain their processes. If you encounter resistance or vague answers, consider it a warning sign.
Schedule Morning Appointments
Early morning appointments offer the best opportunity to experience equipment at its cleanest. Foot baths in particular are typically most thoroughly cleaned overnight, making the first appointment of the day significantly safer from a fungal perspective. Additionally, staff are often less rushed during morning hours, allowing for more thorough cleaning between clients.
Skip Shaving 24 Hours Before
Tiny nicks from shaving create entry points for fungal organisms to penetrate the skin. Wait at least 24 hours after shaving before your pedicure to allow these microscopic cuts to close. This simple timing adjustment dramatically reduces your infection risk while still allowing you to have smooth legs for your salon visit. For more information on maintaining healthy nails, check out this guide on toenail fungus cure vs. maintenance.
Bring Your Own Tools When Possible
Investing in a personal pedicure kit eliminates much of the cross-contamination risk. Include high-quality metal implements like nail clippers, cuticle pushers, and nippers, as well as your own file and buffer. Most salons are happy to accommodate clients who bring their own tools—it demonstrates your awareness and actually makes their job easier.
Store your personal tools in a clean, dry container and sanitize them with rubbing alcohol after each use. This small investment provides significant protection against not just fungal infections but other communicable conditions as well.
10 Essential Questions to Ask Your Nail Technician
Knowledge is power when it comes to salon safety. Don’t be shy about asking these important questions—your health is worth more than momentary discomfort. Professional technicians respect clients who prioritize safety and will gladly address your concerns.
1. How Do You Sanitize Your Tools Between Clients?
The correct answer should include methods beyond the blue liquid disinfectant you commonly see. Listen for mentions of an autoclave (heat sterilization), UV sanitizers, or hospital-grade disinfectants with specific dwell times. The technician should be able to explain their process confidently and in detail, not just offer vague reassurances about cleanliness. For more on maintaining nail health, consider reading about the strategic journey to clear nails.
2. Are These Tools From a Newly-Opened Package?
For non-metal implements like files, buffers, and wooden sticks, the only acceptable answer is yes. These porous items cannot be properly sterilized and must be single-use or dedicated to you personally. Some premium salons offer clients the option to purchase and store their own set of these tools for future appointments.
3. How Often Do You Clean Your Foot Baths?
The proper protocol includes removing and cleaning all removable parts, disinfecting with an EPA-registered hospital disinfectant, and running a cleaning cycle between every client. Additionally, deeper cleaning procedures should be performed daily, with special attention to jets and drains where biofilm can accumulate. If the technician seems uncertain or indicates that cleaning happens only at day’s end, consider this a significant red flag.
4. What Disinfectant Do You Use?
Professional salons use hospital-grade disinfectants that are EPA-registered and specifically labeled for killing fungi, bacteria, and viruses. The disinfectant should be mixed at the proper concentration and allowed to remain on surfaces for the full contact time specified by the manufacturer—typically 10 minutes. If the technician doesn’t know the name of their disinfectant or its contact time, this suggests inadequate training in proper sanitization procedures.
5. Is That a New File/Buffer?
This direct question puts the technician on the spot and gives you immediate information about their sanitation standards. Even if you’re told these items are cleaned between clients, remember that porous materials cannot be truly sterilized. Insist on new files and buffers for your service or bring your own.
6. Can I Bring My Own Tools?
Any reputable salon should accommodate this request without resistance. If you encounter pushback or feel the technician is offended by your request, this may indicate the salon prioritizes convenience over client safety. Professional technicians understand and respect a client’s desire to use their own sanitized tools.
7. Do You Have a Protocol for Handling Cuts?
Accidents happen even with skilled technicians. What matters is how they respond to minor injuries. The correct protocol includes stopping the service, applying antiseptic, covering the area with a clean bandage, and either changing gloves or washing hands before continuing. Technicians should also have appropriate first aid supplies readily available.
8. How Do You Handle Clients With Visible Infections?
Ethical salons refuse service to clients with visible fungal infections to prevent transmission to other customers. If the technician hesitates or indicates they would proceed anyway, this reveals a dangerous gap in their safety protocols. Some salons offer specialized services for clients with medical conditions, but these should involve completely separate tools and enhanced precautions.
9. How Often Do You Replace Your Salon Equipment?
Foot baths with cracks or damaged jets cannot be properly sanitized. Quality salons regularly maintain and replace equipment before it deteriorates. Listen for specific timeframes and maintenance schedules rather than vague reassurances.
10. Can I See Your Salon’s Health Inspection Certificate?
Licensed establishments should have recent health inspection certificates available for review. This documentation demonstrates compliance with local health regulations. If the salon cannot produce this documentation or seems reluctant to share it, consider choosing a different establishment for your services.
Proper Sterilization: What to Look For During Your Visit
Once you’re at the salon, stay observant throughout your appointment. Understanding proper sterilization methods allows you to recognize whether the salon is following best practices for preventing fungal infections.
The Autoclave Method
The gold standard in tool sterilization is the autoclave—a machine that uses steam under pressure to kill all microorganisms, including resistant fungal spores. Metal tools should be scrubbed, ultrasonically cleaned, then sealed in pouches and processed in the autoclave. Look for an actual autoclave machine on the premises and for tools being removed from sealed sterilization pouches before your service begins.
If the salon claims to use autoclave sterilization but you don’t see the machine or sterilization pouches, ask for clarification. Some salons contract with medical sterilization services or share equipment with neighboring businesses, but they should be transparent about their processes.
Proper Chemical Disinfection Steps
When chemical disinfectants are used, proper procedure involves multiple steps. First, tools must be thoroughly cleaned of all visible debris and organic matter. Then, they should be fully immersed in properly diluted EPA-registered disinfectant for the manufacturer-specified contact time (usually 10+ minutes). Watch for shortcuts in this process—quick dips or sprays are inadequate for killing fungal spores.
Quality salons often use a three-container system: one for cleaning, one for disinfection, and one for storage of disinfected tools. This systematic approach helps prevent cross-contamination and ensures proper disinfection protocols are followed for each implement.
Single-Use Items That Should Never Be Reused
Certain items should only be used once due to their porous nature, which harbors microorganisms even after cleaning attempts. These include emery boards, wooden tools, pumice stones, toe separators, and buffers. If you see these items being reused between clients, this is a clear indicator that the salon doesn’t follow proper sanitation protocols, regardless of what they might claim.
How Nail Fungus Spreads in Salons
Understanding the transmission mechanisms of nail fungus can help you better protect yourself during salon visits. Fungi are opportunistic organisms that require specific conditions to establish an infection. To learn more about effective treatments, you can explore short and long-term solutions for chronic infections.
The Perfect Breeding Environment
Nail salons inadvertently create ideal conditions for fungal growth: warmth, moisture, and repeated exposure to potentially contaminated surfaces. The fungus that commonly affects nails, dermatophytes, feeds on keratin—the protein that makes up your nails. These organisms can survive for months on surfaces and tools if not properly eliminated through sterilization.
Fungal spores are microscopic and can float in the air or settle on surfaces throughout the salon. A single infected client can potentially contaminate an entire salon environment if proper disinfection protocols aren’t followed rigorously.
Common Transmission Routes
Fungal infections typically enter through tiny breaks in the skin or nail/skin separation—often so small you can’t see them. Aggressive cuticle trimming, cutting nails too short, or accidentally nicking the skin during a pedicure creates entry points for fungi. Shared tools that contact multiple clients’ feet without proper sterilization between uses serve as perfect vehicles for transmission.
Even salon surfaces like chairs, floors, and countertops can harbor fungal spores if not regularly disinfected. Walking barefoot in the salon significantly increases your exposure risk, as does touching your feet after contacting potentially contaminated surfaces.
Why Foot Baths Are Particularly Risky
Pedicure foot baths present one of the highest risks in nail salons, especially those with jets or recirculating systems. The warm water softens skin and nails, making them more vulnerable to infection, while the jets can trap skin cells, nail fragments, and fungi in their complex tubing systems. Studies have found that even properly cleaned whirlpool foot baths can harbor potential pathogens in biofilms that form inside the plumbing.
The most dangerous foot baths are those where you can’t see the cleaning process between clients or where the jets run continuously throughout the day. This continuous use without thorough disinfection between clients creates a perfect environment for fungal proliferation and transmission.
Personal Protection Strategies During Your Pedicure
Beyond choosing a clean salon, you can take personal steps to dramatically reduce your infection risk during pedicure appointments. These simple protective measures create an additional barrier between you and potential pathogens, helping to prevent toenail fungus recurrence.
Bring Your Own Flip-Flops
Never walk barefoot in a salon. Bring dedicated flip-flops that you wear only during your salon visits to prevent picking up fungi from floors. These should be easily washable and disinfectable after each use. Some clients even bring disposable pedicure slippers that can be discarded after a single use for maximum protection.
Request No Cuticle Cutting
Ask your technician to gently push back cuticles rather than cutting them. Cuticles form a natural protective seal between your nail and surrounding skin, and breaking this barrier increases infection risk significantly. If you feel strongly about cuticle removal, have this done by a medical professional or wait until you’ve established complete trust in your salon’s sterilization practices.
Examine Your Feet Before and After
Take a moment before your appointment to check your feet for any cuts, scrapes, or skin conditions that might increase your vulnerability to infection. If you notice any breaks in the skin, consider postponing your pedicure until these have healed. Small injuries you may not even feel can become entry points for fungal spores.
After your appointment, reexamine your feet for any nicks or cuts that may have occurred during the service. If you notice any, clean them immediately with antiseptic and apply an appropriate antibiotic ointment to prevent infection.
Apply Antifungal Cream Preventatively
Consider applying an over-the-counter antifungal cream to your feet and nails before and after your pedicure as an extra precautionary measure. This creates a protective barrier that can help prevent fungal organisms from establishing themselves in your nail tissue. Pinnacle Dermatology often recommends this approach for patients with higher risk factors or those who have previously experienced fungal infections.
Red Flags That Should Make You Walk Out
Sometimes the most important safety decision is choosing to leave. If you observe any of these serious violations during your visit, politely excuse yourself and find another salon. No pedicure is worth risking a fungal infection that could take months or even years to resolve completely.
Watch for technicians using the same tools on multiple clients without proper sterilization between uses, visible dirt or debris in foot baths, or staff members with visibly infected nails providing services. Other concerning practices include cutting cuticles deeply, causing bleeding during the service, or using razors to remove calluses (illegal in many states due to infection risks). Trust your instincts—if something doesn’t look or feel right about the salon’s hygiene practices, it’s better to leave than risk infection.
After Your Pedicure: Home Care to Prevent Infection
Your fungal prevention strategy doesn’t end when you leave the salon. The 24-48 hours following your pedicure are critical for preventing any potential fungal spores from establishing themselves in your nail tissue. For a comprehensive approach, consider following a guide to preventing toenail fungus recurrence to ensure long-term nail health.
Immediate Post-Salon Cleaning Steps
As soon as possible after your appointment, thoroughly wash your feet with antibacterial soap and warm water, paying special attention to the areas between toes and around nails. Follow with a careful drying, especially between toes where moisture can linger. Some podiatrists even recommend using a hair dryer on a cool setting to ensure complete drying in these hard-to-reach areas.
Daily Foot Hygiene Practices
Maintain vigilant foot hygiene for several days after your pedicure. This includes changing socks daily, wearing breathable footwear, and continuing to thoroughly dry between toes after bathing. Applying a thin layer of antifungal powder to your feet can provide additional protection during this vulnerable period.
Moisture Control Techniques
Fungi thrive in moist environments, making moisture control essential in preventing infection. Consider applying cornstarch or antifungal powder between toes and wearing moisture-wicking socks if you tend to have sweaty feet. Alternating shoes daily allows them to fully dry between wearings, further reducing the hospitable environment that fungi need to establish an infection.
For individuals with frequent exposure to wet environments or those who exercise regularly, bringing an extra pair of socks to change into midday can significantly reduce fungal exposure risks. This simple habit helps maintain a dry environment around your feet throughout the day.
Remember that even fresh nail polish can trap moisture against the nail plate, potentially creating favorable conditions for fungal growth if spores are present. Consider leaving nails polish-free for 24 hours after your pedicure to ensure they’re completely dry and sealed before applying polish.
When to See a Doctor: Signs of Nail Fungus Infection
Despite your best preventive efforts, it’s important to recognize the early signs of nail fungus so you can seek treatment promptly. Early intervention significantly improves treatment outcomes and prevents the infection from spreading to other nails.
Visual Changes to Watch For
The earliest sign of nail fungus is often a small white or yellow spot under the nail that doesn’t go away with cleaning. As the infection progresses, nails may become thickened, discolored (yellow, brown, white, or even green), distorted in shape, or develop crumbly edges. The texture often changes, becoming brittle or ragged.
Monitor your nails regularly, especially in the weeks following a pedicure. Take photos if you notice changes to help track progression. Remember that fungal infections typically worsen gradually over time rather than improving, distinguishing them from temporary damage like bruising under the nail.
Physical Symptoms That Shouldn’t Be Ignored
Beyond visual changes, fungal nail infections can cause physical discomfort. You might notice a slightly foul odor from the affected nail, pain when pressure is applied, or a sensation of the nail separating from the nail bed (onycholysis). Some people experience discomfort when wearing shoes or find that the thickened nail catches on socks and bedding. For more information on managing these symptoms, you can explore long-term solutions for chronic infections.
If you have diabetes, poor circulation, or a weakened immune system, any nail changes require immediate medical attention. What might be a cosmetic concern for some can become a serious health risk for individuals with these conditions. For more information on treatment approaches, you can explore this strategic treatment roadmap.
Treatment Options if You’re Already Infected
If you suspect a fungal nail infection, consult a dermatologist or podiatrist promptly. Professional diagnosis is important as other conditions can mimic fungal infections. Treatment typically involves prescription antifungal medications—either topical solutions applied directly to the nail or oral medications that work throughout your body. For severe infections, your doctor might recommend temporary nail removal to apply medication directly to the nail bed.
Treatment for nail fungus requires patience; complete eradication typically takes months as you must wait for the infected portion of the nail to grow out completely. During this time, continuing preventative measures is crucial to prevent reinfection or spread to other nails.
Your Salon Safety Action Plan
Creating a personal salon safety strategy combines all the preventative measures we’ve discussed into a practical approach that becomes second nature over time. This doesn’t mean avoiding pedicures—it means enjoying them safely with minimal infection risk.
- Research salons carefully before booking, focusing on cleanliness reviews
- Schedule morning appointments when equipment is freshest
- Bring personal tools and flip-flops to each appointment
- Ask about sterilization processes confidently
- Watch for proper tool handling and foot bath cleaning
- Implement post-pedicure cleaning and drying protocols
- Monitor nails for changes in the weeks following services
Remember that your health is worth any momentary awkwardness of asking questions or making special requests. Quality professionals appreciate clients who understand and value proper sanitation practices. By following these guidelines, you can enjoy beautiful, healthy nails without risking the pain and frustration of fungal infections.
Your awareness and proactive approach not only protect your health but also encourage higher industry standards. When clients consistently demand proper sanitation, salons respond by improving their practices—creating safer environments for everyone.
Frequently Asked Questions
Clients commonly have questions about nail fungus and salon safety. Here are evidence-based answers to help you make informed decisions about your nail care.
How common is it to get nail fungus from a pedicure?
Studies show that approximately 3-8% of pedicure clients may develop fungal nail infections, with risk factors including:
- Frequency of salon visits (higher with more frequent visits)
- Presence of diabetes or compromised immunity
- Previous history of fungal infections
- Age (risk increases after 60)
- Poor salon hygiene practices
While the absolute risk may seem relatively low, the stubborn nature of fungal infections makes prevention particularly important. A single infection can require months of treatment and may recur if not completely eradicated. The prevalence of fungal infections among regular salon-goers increases significantly when clients visit establishments with suboptimal sanitization practices.
Research published in the Journal of the American Podiatric Medical Association found that fungal organisms were present in 37% of sampled foot baths in salons across the US, even in establishments that appeared visually clean. This highlights the importance of choosing salons with rigorous, verifiable disinfection protocols rather than relying on appearances alone.
The good news is that with proper prevention—both in selecting quality salons and implementing personal protective strategies—you can reduce your risk substantially. Most cases of salon-acquired fungal infections are preventable with the right knowledge and precautions.
Can I get a pedicure if I already have nail fungus?
Most reputable salons will refuse service if you have visible signs of fungal infection, and for good reason. Having a pedicure with an active infection risks spreading it to your other nails and to other clients. The professional approach is to seek medical treatment first, receive clearance from your doctor, and then return for nail services when the infection has resolved.
If you’re currently undergoing treatment for nail fungus, consider discussing with your dermatologist or podiatrist whether at-home pedicures might be appropriate during your recovery period. Many professionals can recommend safe ways to maintain foot care while avoiding reinfection or treatment interference.
How quickly does nail fungus appear after exposure?
Nail fungus typically has an incubation period ranging from a few weeks to several months after exposure. This delayed onset often makes it difficult to connect the infection to a specific salon visit, especially for clients who receive regular pedicures. The first visible signs might be subtle—a small discolored spot or slight texture change—and easy to overlook until the infection becomes more established.
The variation in incubation time depends on several factors, including the specific fungal strain, the amount of exposure, your immune response, and whether there were breaks in the skin or nail that allowed easier fungal entry. People with compromised immune systems or diabetes typically develop visible symptoms more quickly and experience more severe infections.
Are gel pedicures safer than regular polish?
Gel pedicures carry their own set of considerations regarding fungal infection risk. The tight seal created by gel polish might temporarily protect nails from external fungal exposure, but it can also trap moisture if fungi are already present. Additionally, the removal process for gel polish can sometimes damage the nail surface, potentially creating entry points for fungi during future exposures.
From a sanitization perspective, the tools and processes used for gel applications versus regular polish make little difference in your infection risk. What matters more is the salon’s overall hygiene practices, tool sterilization protocols, and foot bath cleaning procedures. If choosing between services, consider your personal risk factors and nail health history rather than assuming one type of polish application is inherently safer.
Will nail polish hide fungal infections?
While nail polish may temporarily mask the discoloration of a fungal infection, it cannot hide the infection as it progresses. More concerning, polish creates a sealed environment that can worsen the infection by trapping moisture against the nail. Most dermatologists and podiatrists recommend avoiding polish entirely until a fungal infection is completely resolved.
If you notice nail changes after removing polish, don’t immediately reapply to hide the problem. Instead, leave nails unpolished for several weeks to monitor for improvement or worsening. This observation period can help distinguish between temporary damage from polish products versus an actual fungal infection requiring treatment.
At Pinnacle Dermatology, we specialize in diagnosing and treating nail conditions, including fungal infections acquired from salon visits. Our dermatologists can provide personalized treatment plans and preventative strategies to keep your nails healthy and beautiful while enjoying professional nail services safely.

 Nail Fungus Cures Instant Cures for Painful Nails and Fungus
Nail Fungus Cures Instant Cures for Painful Nails and Fungus