Key Takeaways
- Fungal infections (onychomycosis) are the most common cause of yellow toenails, affecting more adults than children and often requiring consistent treatment.
- Underlying medical conditions like Yellow Nail Syndrome, diabetes, and psoriasis can also turn toenails yellow, signaling potentially serious health concerns.
- Everyday habits including nail polish use without base coat, smoking, and trauma to the nail can result in yellow discoloration even without infection.
- Natural remedies like tea tree oil, apple cider vinegar, and oregano oil can effectively treat mild cases of fungal-related yellow toenails.
- Prevention strategies such as proper foot hygiene, appropriate footwear, and a balanced diet rich in biotin can help maintain healthy, clear toenails.
Yellow Toenails: What’s Really Happening to Your Feet?
Looking down at your feet to find yellow toenails can be alarming. That golden hue isn’t just a cosmetic concern – it’s your body signaling something’s not right. Yellow toenails develop when the nail plate changes color due to various underlying causes, ranging from simple staining to complex medical conditions.
Healthy nails should appear clear or slightly pink, with a smooth, consistent texture. When discoloration occurs, it typically starts at the tip or edge of the nail and gradually spreads toward the base. This progression isn’t just unsightly; it often accompanies other changes like thickening, brittleness, or even nail separation from the bed beneath.
Understanding what’s causing those yellow toenails is the first step toward effective treatment. While you might be tempted to hide discolored nails under polish, addressing the root cause will not only improve appearance but potentially prevent more serious complications down the road.
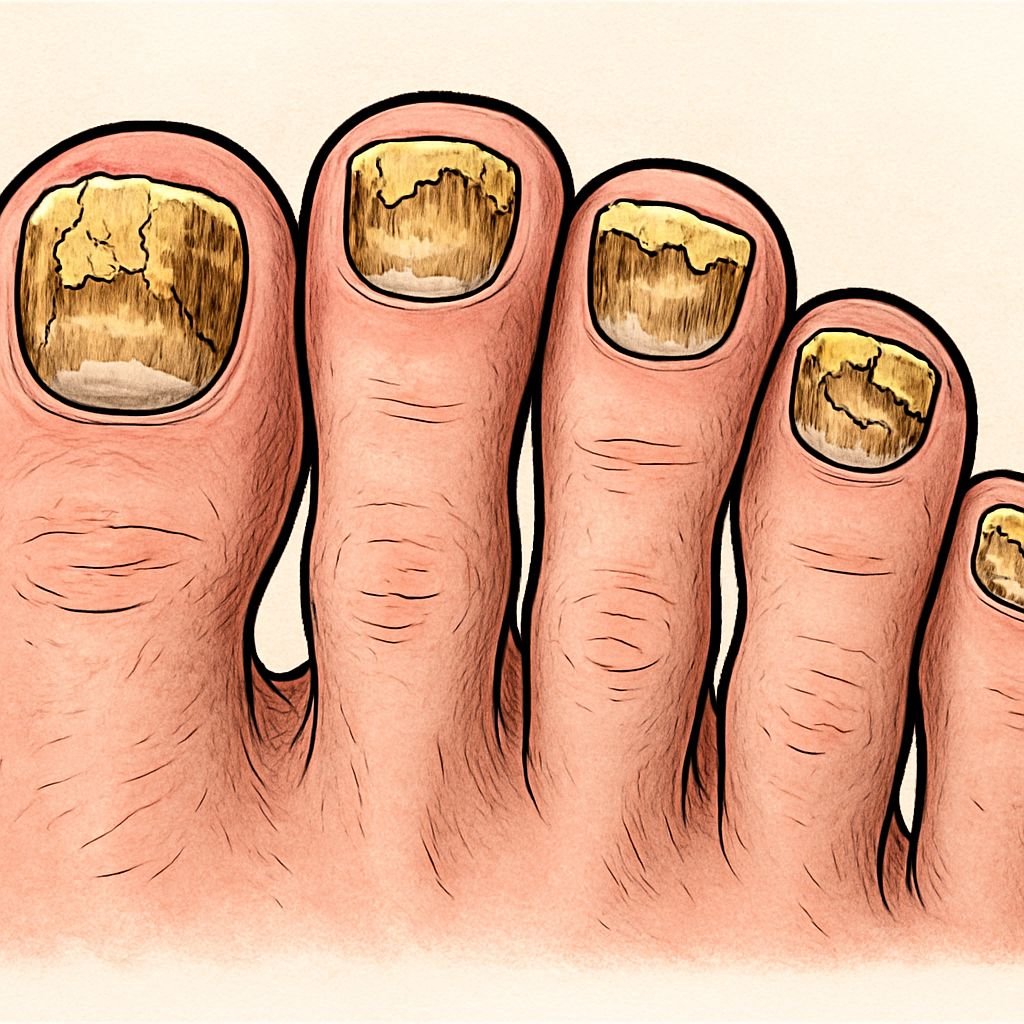
Fungal Infections: The Most Common Culprit of Yellow Toenails
When it comes to yellow toenails, fungal infections lead the pack as the primary cause. These infections, medically termed onychomycosis, affect approximately 10% of the general population and up to 50% of people over age 70. The fungi responsible thrive in warm, moist environments – precisely the conditions often found inside shoes.
How Fungal Infections Attack Your Nails
- Fungi enter through small separations between the nail and nail bed or through tiny cuts in surrounding skin
- They feed on keratin, the protein that forms the hard surface of toenails
- As they multiply, they cause the characteristic yellow discoloration along with thickening
- Without treatment, the infection progressively damages the entire nail structure
- The same fungi may spread to other toenails or even fingernails if not addressed
The infection typically begins with subtle white or yellow spots under the tip of your toenail. This initial stage is where the fungal organisms first gain entry. As the infection progresses, your toenail becomes increasingly yellow, thick, and brittle. Eventually, the nail may become distorted in shape, develop crumbling edges, and emit an unpleasant odor – all signs the infection has become well-established.
Different types of fungi can cause these infections, with dermatophytes being the most common culprits. These specialized organisms have evolved specifically to digest keratin, making your nails the perfect feeding ground. For a deeper understanding of these infections, you can refer to this definitive guide on onychomycosis. Yeasts and non-dermatophyte molds can also infect toenails, though less frequently.
Risk Factors That Make You Vulnerable to Fungal Infections
Certain lifestyle factors and conditions significantly increase your risk of developing fungal nail infections. Walking barefoot in public showers, pools, and locker rooms exposes your feet to environments where fungi flourish. Wearing damp socks or tight-fitting shoes creates the warm, moist conditions these organisms need to thrive. People with compromised immune systems, diabetes, or circulation problems face higher risks, as do those who frequently damage their nails through sports or other activities. Age also plays a role – older adults typically have slower-growing nails and reduced blood circulation, making them more susceptible to fungal invasion.
The Progression: From Slight Discoloration to Serious Damage
Fungal nail infections rarely resolve without intervention. What begins as a small yellow spot typically evolves through predictable stages if left untreated. In early phases, the discoloration may be dismissed as minor or purely cosmetic. As months pass, the infection penetrates deeper, causing the nail to thicken, become brittle, and develop a distorted shape. The yellow color often darkens to brown or even black in advanced cases. Ultimately, the nail may separate from the nail bed completely – a condition called onycholysis – creating additional spaces for dirt and bacteria to accumulate. This progression doesn’t just affect appearance; it can lead to pain, difficulty wearing shoes, and increased risk of secondary bacterial infections.
Medical Conditions That Turn Toenails Yellow
While fungal infections commonly cause yellow toenails, various underlying medical conditions can also trigger this distinctive discoloration. These conditions typically affect multiple body systems and produce yellow nails as one symptom among many. Recognizing when yellow toenails might signal a more serious health issue can be crucial for early intervention and appropriate treatment.
Yellow Nail Syndrome: More Than Just Discolored Nails
Yellow Nail Syndrome: Key Characteristics
• Thick, yellow, slow-growing nails with excessive curvature
• Absent cuticles and detachment from nail beds
• Often accompanied by respiratory problems including bronchiectasis
• Frequently involves lymphedema (swelling due to lymphatic system issues)
• Rare condition, typically affecting adults between 40-70 years of age
Yellow Nail Syndrome (YNS) represents a rare but significant medical condition where the yellowing of nails serves as an important diagnostic clue. Unlike fungal infections, YNS causes all twenty nails to turn yellow simultaneously, with distinctive characteristics including extremely slow growth and an exaggerated side-to-side curvature. The condition occurs when the lymphatic vessels responsible for fluid drainage develop abnormally, leading to problems that extend far beyond nail appearance.
Most YNS patients experience respiratory issues including chronic cough, bronchiectasis (damaged airways), sinusitis, and pleural effusions (fluid around the lungs). Lymphedema, a condition characterized by swelling in the arms or legs due to lymphatic system blockage, frequently accompanies the nail changes. While the exact cause remains unclear, YNS has been associated with autoimmune disorders, certain medications, and malignancies, making it important to investigate thoroughly when suspected.
Diabetes and Its Effects on Nail Health
Diabetes significantly impacts circulation throughout the body, including blood flow to your extremities. This reduced circulation can cause toenails to yellow, thicken, and grow abnormally. For diabetics, maintaining healthy toenails isn’t just about aesthetics – it’s about preventing serious complications. The combination of poor blood flow, nerve damage, and compromised immune function makes even minor nail problems potentially dangerous.
High blood sugar levels associated with diabetes can also promote fungal growth, making diabetics especially vulnerable to fungal nail infections. The condition often creates a dangerous cycle: diabetes makes fungal infections more likely, while infections increase inflammation and further compromise circulation. Any toenail changes in people with diabetes warrant prompt medical attention, as they may indicate poor glucose control or signal the beginning of more serious foot complications.
Psoriasis and Related Skin Conditions
Nail psoriasis affects approximately 50% of people with psoriasis and up to 80% of those with psoriatic arthritis. This inflammatory condition doesn’t just impact the skin – it can dramatically alter nail appearance, causing yellowish-brown discoloration, pitting, ridging, and thickening. The changes occur because psoriasis accelerates the growth cycle of skin cells, including those that form the nail bed.
Unlike fungal infections that typically start at the nail’s edge, psoriatic nail changes often begin with small pits in the nail surface, eventually progressing to more significant discoloration and structural changes. The nail may separate from the bed (onycholysis), allowing debris to accumulate underneath, which compounds the yellow appearance. Treatment typically focuses on managing the underlying psoriasis through medications that moderate immune system activity rather than targeting the nails directly.
Respiratory and Lymphatic System Problems
Chronic respiratory conditions like bronchitis, sinusitis, and pleural effusions can sometimes manifest as yellow toenails, particularly when associated with lymphatic system dysfunction. When the body’s drainage and filtering system malfunctions, fluid buildup and inflammation can impact even seemingly unrelated areas like toenails. These systemic conditions often cause distinctive nail changes, including slowed growth, increased curvature, and a thick, yellow appearance that affects most or all nails simultaneously. For more information on similar nail changes, you can explore the definitive guide on onychomycosis.
While the exact mechanism remains unclear, researchers believe lymphatic drainage problems may disrupt the delicate balance of nutrients, oxygen, and waste removal necessary for healthy nail growth. For some patients, yellow toenails may actually precede respiratory symptoms by months or even years, potentially serving as an early warning sign of developing respiratory issues. When yellow toenails appear alongside respiratory symptoms such as chronic cough, shortness of breath, or recurring sinus problems, a thorough medical evaluation becomes essential for proper diagnosis and treatment. For those seeking more information on managing nail issues, this definitive guide on onychomycosis may provide valuable insights.
Everyday Habits That Cause Yellow Toenails
Not all yellow toenails stem from infections or medical conditions. Sometimes, our daily habits and choices lead to discoloration that, while concerning in appearance, may be relatively harmless. Understanding these common causes can help you determine whether your yellow toenails require medical attention or simple lifestyle adjustments.
Nail Polish Problems: When Beauty Products Stain
Regular use of dark-colored nail polish without a protective base coat ranks among the most common causes of yellow toenails. The pigments in polish, particularly reds, oranges, and darker shades, can penetrate the nail plate over time, leaving a yellowish stain that persists even after polish removal. This discoloration typically affects the nail’s surface layer and appears more uniform than the patchy yellowing seen with fungal infections.
Formaldehyde and other chemicals in nail products can also react with the keratin in your nails, causing a chemical yellowing that deepens with repeated applications. Gel and acrylic nails pose additional risks, as the removal process often damages the nail surface, making it more porous and susceptible to staining. Giving your nails regular “breathing periods” without polish and always using a quality base coat can significantly reduce polish-related yellowing.
Smoking and Nicotine Staining
Smokers frequently develop yellow fingers and toenails due to nicotine and tar deposits. These substances have a remarkable ability to penetrate the nail plate, causing a distinctive yellowish-brown discoloration that’s difficult to remove. The staining typically affects all nails relatively uniformly and often accompanies yellowing of the fingers and surrounding skin.
Beyond surface staining, smoking restricts blood flow throughout the body, including to the extremities. This reduced circulation can slow nail growth and impair the body’s natural healing processes, making smokers’ nails more vulnerable to fungal infections and other problems. The combination of direct staining and compromised circulation creates a double threat to nail health that often persists until smoking cessation.
Trauma and Injuries to the Toenail
Physical trauma to toenails—whether from a single significant injury or repetitive minor impacts—commonly causes yellowing and other color changes. Activities like running, hiking, or wearing too-tight shoes can create what’s known as “runner’s toe” or “tennis toe,” where repeated microtrauma leads to bleeding under the nail (subungual hematoma). As the blood breaks down, it often takes on a yellowish appearance that grows out with the nail.
More serious injuries can disrupt the nail matrix—the area where nail growth begins—resulting in permanent changes to nail color and structure. The nail may thicken, develop ridges, or grow irregularly in addition to yellowing. Traumatic nail injuries also create entry points for fungi and bacteria, increasing infection risk. While minor trauma-related yellowing typically resolves as the nail grows out, significant injuries may require medical attention to prevent complications and promote proper healing.
Aging: Natural Changes in Nail Color and Texture
As we age, our nails naturally undergo various changes, including a tendency toward yellowing. This age-related discoloration results from several factors: slower nail growth, decreased circulation to the extremities, and cumulative exposure to environmental elements. The nail plate often becomes thicker and more brittle while developing subtle yellowing that affects all nails relatively uniformly.
The natural aging process causes the production of keratin—the protein that forms nails—to slow and change in composition, contributing to color and texture alterations. While these changes don’t necessarily indicate disease, they can make older nails more vulnerable to fungal infections and other problems. Regular maintenance becomes increasingly important with age, as thickened nails are harder to trim properly and may cause discomfort if not managed correctly.
5 Natural Treatments for Yellow Toenails
Before turning to prescription medications, many people find success treating yellow toenails with natural remedies, particularly when the yellowing stems from mild to moderate fungal infections. These treatments harness the power of natural antifungal and antimicrobial compounds to combat infections while supporting overall nail health. For a comprehensive understanding of nail fungus treatment strategies, it’s important to note that while results typically take time and consistency, these approaches offer gentler alternatives with fewer side effects than pharmaceutical options.
1. Tea Tree Oil Applications
Tea tree oil stands as one of the most researched natural remedies for fungal nail infections. This essential oil contains powerful compounds like terpinen-4-ol that penetrate the nail plate to combat fungal organisms at their source. Studies have shown that consistent application can significantly reduce infection severity and improve nail appearance over several months.
For best results, dilute pure tea tree oil with a carrier oil like coconut or olive oil at a 1:1 ratio to prevent skin irritation. Apply directly to affected nails using a cotton swab or clean brush twice daily, allowing it to fully absorb before covering with socks or shoes. Patience is key – this treatment typically requires 3-6 months of consistent use before showing substantial improvement.
2. Apple Cider Vinegar Soaks
Apple cider vinegar creates an acidic environment hostile to fungal growth while helping restore the nail’s natural pH balance. The acetic acid in vinegar possesses both antifungal and antibacterial properties that can inhibit pathogen growth and help clear existing infections. Regular soaks can also soften thickened nails, allowing topical treatments to penetrate more effectively.
Prepare a foot bath by mixing equal parts apple cider vinegar and warm water, then soak affected feet for 15-20 minutes daily. After soaking, thoroughly dry your feet – especially between toes – as moisture promotes fungal growth. For enhanced effectiveness, some practitioners recommend adding a few drops of tea tree or oregano oil to the soak. Consistent daily treatment for several weeks typically yields noticeable improvements in nail color and texture.
3. Oregano Oil Treatment Protocol
Oregano oil contains carvacrol and thymol, compounds with potent antifungal properties that research suggests may be as effective as some pharmaceutical treatments against certain fungal species. This powerful essential oil penetrates the nail plate to reach embedded fungi that topical treatments sometimes miss. Its strong antimicrobial action helps eliminate infection while supporting healthy new nail growth.
Due to its potency, oregano oil must be diluted before application – typically mixing 2-3 drops with a teaspoon of carrier oil like olive or coconut oil. Apply this mixture to affected nails twice daily using a cotton swab, focusing on the nail bed and surrounding tissue. Some users report a warming or tingling sensation, which is normal, but discontinue use if significant irritation occurs. A consistent 3-6 month treatment protocol often produces substantial improvement in nail appearance and health.
4. Garlic-Based Remedies
Garlic has been used medicinally for centuries due to its powerful antimicrobial properties. The compound allicin, released when garlic is crushed, demonstrates significant antifungal activity against various pathogens including those responsible for nail infections. Beyond fighting fungus directly, garlic appears to strengthen the immune system, helping your body combat infection more effectively.
Create a simple garlic treatment by crushing 2-3 cloves and mixing with olive oil to form a paste. Apply directly to affected nails, cover with a bandage, and leave on for 30 minutes before rinsing. Alternatively, garlic oil can be purchased ready-made and applied to nails twice daily. The pungent smell presents the main drawback, but many users find the therapeutic benefits outweigh this temporary inconvenience. For best results, combine external applications with adding fresh garlic to your diet to support immune function from within. For more information on effective treatments, check out this strategic treatment roadmap for nail fungus.
5. Coconut Oil for Gentle Healing
Coconut oil offers a gentler approach to treating yellow toenails, particularly beneficial for those with sensitive skin or when yellowing stems from causes other than severe fungal infection. The medium-chain fatty acids in coconut oil, especially lauric acid, possess antimicrobial properties that help inhibit fungal growth while moisturizing and strengthening brittle, damaged nails. Its penetrating nature allows it to reach deep into nail tissues, delivering nourishment and therapeutic compounds where needed.
For daily treatment, warm a small amount of virgin coconut oil between your fingers until liquid, then massage thoroughly into affected nails and surrounding skin. The oil creates a protective barrier that prevents further damage while allowing nails to breathe and heal. Many practitioners recommend applying coconut oil after bathing when nails are most receptive to moisture and nutrients. While results develop more gradually than with stronger remedies, consistent application over several months typically improves nail appearance and resilience significantly. For those dealing with chronic infections, exploring long-term treatment solutions might be beneficial.
Medical Treatments When Home Remedies Aren’t Enough
When natural approaches fail to resolve yellow toenails, professional medical treatments offer more aggressive solutions. These interventions become particularly necessary for severe or persistent fungal infections, yellow nail syndrome, or when underlying medical conditions contribute to nail discoloration. Medical treatments typically work faster than home remedies but may carry additional risks and side effects that should be carefully considered.
Prescription Antifungal Medications
Prescription-strength antifungal medications represent the most effective treatment for fungal-related yellow toenails. These medications work systematically to eliminate fungal infections from within, rather than just treating the nail surface. Oral antifungals like terbinafine (Lamisil) and itraconazole (Sporanox) circulate through the bloodstream and penetrate the nail bed, attacking fungi at their source. These medications typically require 6-12 weeks of treatment and may need liver function monitoring due to potential side effects.
Medical-grade topical solutions containing ciclopirox or efinaconazole provide an alternative for those unable to take oral medications. These prescription solutions must be applied daily to affected nails, usually for 48 weeks or longer. While they work more slowly than oral medications, they offer a safer option for elderly patients or those with liver concerns. The long treatment duration highlights why early intervention remains crucial for managing fungal nail infections effectively.
Topical Solutions vs. Oral Medications
| Treatment Type | Effectiveness | Treatment Duration | Side Effects | Best For |
|---|---|---|---|---|
| Prescription Topical Solutions | Moderate (35-65% cure rate) | 9-12 months | Minimal; local irritation possible | Early infections; patients with liver concerns |
| Oral Terbinafine | High (70-80% cure rate) | 6-12 weeks | Potential liver issues, rash, taste disturbances | Severe/extensive infections |
| Oral Itraconazole | Moderate-High (60-70% cure rate) | 12 weeks (pulse therapy) | Liver concerns, heart rhythm issues, drug interactions | Infections resistant to terbinafine |
| Oral Fluconazole | Moderate (40-50% cure rate) | 6-9 months (weekly dosing) | Fewer liver issues; headache, nausea possible | Patients who can’t tolerate other orals |
Laser Therapy Options
Laser treatment represents a newer approach to treating fungal nail infections that cause yellowing. This non-invasive procedure uses specific wavelengths of light to penetrate the nail and destroy fungal organisms without damaging surrounding tissue. The primary advantages include no systemic side effects, no drug interactions, and relatively quick treatment sessions lasting about 30 minutes. Multiple sessions are typically required, spaced several weeks apart, to achieve optimal results.
Clinical studies on laser effectiveness show mixed results, with success rates varying widely between 30-70% depending on the specific technology used and infection severity. The treatment works best for mild to moderate infections and often produces visible improvement in nail appearance even before complete fungal elimination. Cost represents the main drawback, as laser therapy typically isn’t covered by insurance and can range from $500-1200 for a full treatment course. For best results, many practitioners recommend combining laser therapy with topical antifungals and thorough hygiene practices.
When Surgery Becomes Necessary
In severe cases where medications and other treatments fail, surgical intervention may become necessary to address yellow, damaged toenails. Nail avulsion – the complete or partial removal of the affected nail – allows direct treatment of the nail bed and elimination of severely infected tissue. This procedure is typically performed under local anesthesia and may be temporary (allowing a new nail to grow) or permanent (preventing regrowth in cases of recurring severe infection). For more information on treatments, you can explore this guide on toenail fungus treatment solutions.
For the most extreme cases of fungal infection or nail deformity, matrixectomy may be recommended. This procedure removes part of the nail matrix (growth center), preventing problematic portions of the nail from regrowing. Modern techniques use chemical treatments, laser, or radiofrequency rather than surgical excision, reducing recovery time and complications. While these procedures solve the immediate problem, preventive measures remain essential to avoid reinfection of new nail growth or adjacent toenails.
Fungal vs. Medical Conditions: How to Tell the Difference
Determining whether yellow toenails stem from fungal infection or underlying medical conditions significantly impacts treatment approach and success. While both can cause similar discoloration, subtle differences in appearance, progression pattern, and associated symptoms can help distinguish between these causes. Accurate identification often requires professional evaluation, but understanding key differences can guide you toward appropriate care.
Visual Clues in Nail Appearance
Fungal infections typically begin at the nail’s tip or edge, creating distinct patches of yellow, white, or brown discoloration that gradually spread toward the base. The affected nail often thickens unevenly, develops a crumbly texture at the edges, and may separate from the nail bed. This progression usually affects one or several nails rather than all simultaneously, with the big toenail most commonly targeted.
In contrast, medical conditions like Yellow Nail Syndrome cause more uniform yellowing that frequently affects all twenty nails (fingers and toes). The yellowing appears more consistent throughout the nail plate rather than patchy. Nails associated with systemic conditions often exhibit excessive curvature, slower growth, and may lack lunulas (the white half-moons at the nail base). Psoriatic nails typically show distinctive pitting, ridging, and oil spots beneath the nail surface along with yellowing, while diabetes-related changes include uniform thickening and yellowing associated with poor circulation.
Associated Symptoms to Watch For
Accompanying symptoms provide crucial context for interpreting yellow toenails. Fungal infections rarely cause symptoms beyond the nail itself, though advanced cases may create tenderness or mild pain. The surrounding skin typically remains normal unless secondary bacterial infection develops. Itching, redness, or flaking between toes may indicate athlete’s foot occurring alongside the nail infection.
When yellow toenails stem from systemic medical conditions, they typically appear alongside distinctive symptom clusters. Yellow Nail Syndrome frequently accompanies respiratory problems like chronic cough, sinusitis, or breathing difficulties, along with lymphedema (swelling) in the extremities. Psoriasis-related nail changes usually occur in people with visible skin plaques elsewhere on the body. Diabetes-related yellowing often accompanies other foot issues including numbness, tingling, slow-healing wounds, or skin temperature changes. These accompanying symptoms often provide essential clues that help distinguish between fungal and medical causes of nail discoloration.
Tests Your Doctor Might Recommend
Definitive diagnosis of yellow toenail causes typically requires laboratory confirmation. For suspected fungal infections, your doctor may take nail clippings or debris for microscopic examination and fungal culture to identify the specific organism involved. This process helps determine the most effective treatment approach, as different fungi respond differently to various medications. Newer PCR (polymerase chain reaction) tests can detect fungal DNA more quickly and accurately than traditional cultures but aren’t yet universally available.
When medical conditions are suspected, more comprehensive testing becomes necessary. Blood tests can assess for diabetes, thyroid dysfunction, inflammatory markers, and other systemic issues. Chest X-rays or pulmonary function tests may be ordered if respiratory symptoms accompany nail changes, particularly when Yellow Nail Syndrome is suspected. In some cases, nail biopsies provide definitive diagnosis for conditions like psoriatic nail disease. These diagnostic procedures help guide appropriate treatment by addressing the underlying condition rather than just the nail symptoms.
Prevention Strategies to Keep Toenails Healthy
Preventing yellow toenails proves far easier than treating them once established. A proactive approach to nail health can save significant time, expense, and discomfort by avoiding the conditions that lead to discoloration and damage. These preventive strategies focus on creating an environment where fungi and other pathogens struggle to survive while supporting optimal nail growth and resilience.
Daily Foot Hygiene Essentials
Maintaining meticulous foot hygiene forms the cornerstone of yellow toenail prevention. Wash feet daily with mild soap, paying special attention to the spaces between toes where moisture can accumulate. After washing, dry thoroughly – using a separate towel for feet prevents spreading potential infections to other body areas. Consider using a clean, absorbent cotton cloth specifically for drying between toes where standard towels might miss moisture.
Trim toenails straight across rather than in curved shapes to prevent ingrown nails that create entry points for infection. Keep nails at a moderate length – too short increases injury risk while too long invites debris accumulation and breakage. Filing rough edges with an emery board after trimming reduces snags that can lead to nail damage. For those with diabetes or circulatory issues, professional nail care from a podiatrist offers the safest approach to maintenance.
The Right Footwear Makes a Difference
Your choice of shoes significantly impacts toenail health and coloration. Select breathable footwear made from natural materials like leather or canvas that allow air circulation and moisture evaporation. Shoes should provide adequate room in the toe box – approximately half an inch between your longest toe and the shoe’s end prevents pressure and trauma that can damage nails. Rotating between multiple pairs allows shoes to dry completely between wearings, reducing the damp environment fungi need to thrive.
Socks play an equally important role in preventing yellow toenails. Choose moisture-wicking materials like cotton, wool, or specialized synthetic blends rather than pure synthetics that trap perspiration. Change socks daily or more frequently if feet become damp during activities. For those with particularly sweaty feet, consider changing socks midday or using moisture-absorbing foot powders to maintain dryness. Never reuse socks without washing, as this can reintroduce potential pathogens to clean feet.
Nail Salon Safety Tips
While professional pedicures can help maintain healthy toenails, they can also spread infections if proper sanitization isn’t practiced. Choose reputable salons that visibly sterilize tools between clients using hospital-grade autoclaves rather than simply soaking instruments in disinfectant solution. Tools should be removed from sealed packages in your presence, or better yet, bring your own pedicure kit to eliminate cross-contamination risk. Observe whether foot baths are thoroughly cleaned and disinfected between customers – pipes and jets require special attention as they frequently harbor bacteria and fungi.
During your salon visit, request that cuticles be gently pushed back rather than cut, as damaged cuticles create entry points for infection. Decline aggressive cleaning under nails with sharp instruments that can damage the nail bed. When selecting polish, opt for high-quality brands less likely to cause staining, and always request a clear base coat to prevent direct contact between colored polish and the nail surface. Allow adequate drying time between polish layers to prevent trapped moisture that can promote fungal growth beneath the polish.
Dietary Changes That Support Nail Health
The nutrients you consume directly impact nail strength, growth rate, and resistance to discoloration and infection. Protein serves as the building block of healthy nails – aim for lean sources like poultry, fish, beans, and legumes to support keratin production. Biotin (vitamin B7) plays a crucial role in nail health; found in eggs, nuts, and whole grains, this nutrient strengthens brittle nails and promotes normal growth patterns. Zinc and iron contribute to nail resilience and proper coloration – incorporate oysters, pumpkin seeds, spinach, and lean red meat to maintain optimal levels.
Hydration status significantly affects nail appearance and health. Drink sufficient water daily (typically 8-10 cups for most adults) to keep nails properly moisturized from within. Consider reducing sugar consumption, as high blood glucose levels create favorable conditions for fungal growth while compromising immune function. Probiotic-rich foods like yogurt, kefir, and fermented vegetables support beneficial gut bacteria that enhance immune response against potential nail pathogens. These dietary adjustments not only improve nail appearance but contribute to overall health and resistance to infections throughout the body. For a comprehensive approach, explore this strategic treatment roadmap for nail fungus.
When to See a Doctor About Yellow Toenails
While many cases of yellow toenails respond well to home care, certain situations warrant professional medical attention. Knowing when to seek help can prevent complications, identify underlying health concerns, and ensure you receive the most effective treatment for your specific condition. Early intervention often leads to faster resolution and reduces the risk of permanent nail damage.
Generally, you should consult a healthcare provider if yellow toenails persist despite several weeks of consistent home treatment, or if they’re accompanied by pain, spreading inflammation, or changes in surrounding skin. Immediate medical attention becomes necessary when infection appears to spread beyond the nail or if you notice pus, increasing pain, or red streaks extending from the affected area – signs of a potentially serious bacterial infection requiring prompt treatment.
Warning Signs That Require Immediate Attention
- Severe pain, throbbing, or pulsating in the affected toe
- Red streaks extending up from the toe toward the foot or leg
- Fever or chills occurring alongside nail changes
- Pus or discharge from around the nail
- Significant swelling, warmth, or redness beyond the immediate nail area
- Sudden spread of discoloration to multiple nails simultaneously
- Complete nail detachment or substantial bleeding under the nail
- New nail changes in people with diabetes, circulation disorders, or immune suppression
Specialists Who Treat Nail Problems
Several types of healthcare professionals specialize in treating yellow toenails, each offering different expertise. Dermatologists specialize in skin, hair, and nail disorders, making them excellent resources for diagnosing and treating fungal infections and nail changes related to skin conditions like psoriasis. Podiatrists focus specifically on foot health, offering comprehensive care for toenail problems alongside other foot-related concerns. For yellow nails potentially linked to systemic conditions, primary care physicians coordinate care and refer to appropriate specialists including endocrinologists (for diabetes), pulmonologists (for respiratory conditions), or rheumatologists (for autoimmune disorders).
When selecting a specialist, consider their specific expertise with your suspected condition, insurance coverage, and appointment availability. Many patients benefit from starting with their primary care provider, who can conduct initial evaluation and direct to appropriate specialists if needed. For those with diabetes or circulatory problems, regular podiatric care should be part of standard healthcare regardless of whether nail discoloration is present, as early detection of foot problems prevents serious complications.
What to Expect During Your Appointment
A medical appointment for yellow toenails typically begins with a thorough history covering when you first noticed the discoloration, any treatments you’ve tried, related symptoms, underlying health conditions, and current medications. The provider will examine not just the affected nails but also surrounding skin, other nails, and potentially other body areas to identify patterns suggesting specific causes. Be prepared to remove all nail polish before your appointment to allow proper examination.
Diagnostic procedures may include nail clippings for laboratory analysis, which involves taking small samples from the affected nail for fungal testing. Some providers use dermoscopy – examination with a special magnifying device – to visualize subtle nail changes not apparent to the naked eye. Based on findings, your provider will develop a treatment plan tailored to the underlying cause of your yellow toenails and may recommend follow-up visits to monitor progress. Bring a list of questions to your appointment and take notes on recommended treatments, as proper adherence to the treatment protocol significantly impacts success rates.
Your Path to Clear, Healthy Toenails
Restoring yellow toenails to their natural, healthy state requires patience, consistency, and the right approach based on underlying causes. Improvement typically occurs gradually as new, healthy nail grows from the base to replace discolored portions – a process that takes 6-18 months depending on individual growth rates. Rather than expecting overnight results, look for subtle signs of progress: clearer nail emerging from the cuticle, reduced thickening, and improved texture. Combining appropriate medical treatments with preventive measures and nutritional support offers the most comprehensive approach to nail restoration and long-term health. Remember that maintaining results requires ongoing attention to foot hygiene, proper footwear, and addressing underlying health conditions that might contribute to recurrence.
Frequently Asked Questions
Yellow toenails generate numerous questions from those experiencing this common but concerning condition. The following answers address the most frequently asked questions, providing clear guidance based on current medical understanding. While these responses offer general information, remember that individual cases may vary, and personalized medical advice remains essential for persistent or severe nail problems.
Can yellow toenails spread to other people?
When caused by fungal infections, yellow toenails can potentially spread to others through direct contact or shared surfaces. The fungi responsible thrive in warm, moist environments like shower floors, pool decks, and shared footwear. They spread when fungal spores from an infected person contact another person’s skin or nails, particularly if there are tiny cuts or separations between the nail and nail bed that allow entry.
To prevent transmission, avoid sharing personal items like shoes, socks, nail clippers, or towels with someone who has a fungal nail infection. In household settings, disinfect shower floors regularly and consider wearing shower shoes if a family member has an infection. Public spaces present higher transmission risks – always wear protective footwear in locker rooms, public showers, and around swimming pools. For more information on preventing nail fungus transmission, check out this guide.
Yellow toenails caused by medical conditions like Yellow Nail Syndrome, psoriasis, or aging are not contagious and cannot spread to others through contact. When in doubt about whether your yellow toenails pose a contagion risk, consult a healthcare provider for proper diagnosis and guidance on appropriate precautions.
How long does it take to cure yellow toenails?
Recovery time for yellow toenails varies significantly depending on the underlying cause, treatment approach, and individual factors like age and overall health. Fungal infections typically require the most patience – complete resolution often takes 6-18 months as infected nail must grow out completely and be replaced by healthy new growth. Prescription oral medications may show visible improvement within 3-6 months but require continuing treatment until the nail grows out fully. Natural remedies and topical treatments generally work more slowly, often taking 9-12 months or longer for complete results, though gradual improvements may become visible earlier. For a comprehensive understanding of the strategic treatment roadmap for nail fungus, consider reviewing expert guides.
Are certain people more likely to get yellow toenails?
Several factors increase susceptibility to yellow toenails, particularly those caused by fungal infections. Older adults face higher risk due to slower nail growth, reduced circulation, and compromised immune function that comes with aging. People with diabetes, circulatory disorders, or immune system weaknesses experience significantly higher rates of fungal nail infections. Those who frequent public swimming pools, locker rooms, or communal showers encounter more exposure to nail pathogens. Athletes, especially runners, often experience nail trauma that creates entry points for infection while generating conditions favorable for fungal growth. Occupation also plays a role – those whose jobs require wearing occlusive footwear for extended periods (like construction workers, military personnel, and healthcare professionals) face increased risk due to warm, moist environments created inside shoes. For more information on effective treatment options, you can explore this guide to toenail fungus treatments.
Can I wear nail polish while treating yellow toenails?
Generally, medical professionals recommend avoiding nail polish during treatment for fungal-related yellow toenails. Polish creates a sealed environment that traps moisture and blocks medication penetration, potentially extending treatment time and reducing effectiveness. The solvents in polish removers can also damage nails and irritate surrounding tissues, further compromising treatment outcomes. If appearance concerns make going polish-free difficult, discuss with your healthcare provider whether medicated nail polishes containing antifungal ingredients might be appropriate for your situation – these specialized products allow some cosmetic coverage while continuing to address the underlying infection.
Will my yellow toenails ever return to normal color?
In most cases, yellow toenails can return to normal color and appearance with appropriate treatment and patience. Fungal infections typically show gradual improvement as new, healthy nail grows from the base, eventually replacing the discolored portion completely. Staining from polish usually grows out within 3-6 months after discontinuing the staining product. Even nail changes associated with some medical conditions may show improvement when the underlying condition is properly managed. However, long-standing severe fungal infections or significant structural changes to the nail matrix may result in permanent alterations to nail appearance. The key to maximal improvement lies in accurate diagnosis, appropriate treatment, consistent preventive measures, and realistic expectations about the time required for complete nail renewal.
For comprehensive support in addressing foot health concerns including yellow toenails, consider consulting with podiatric specialists at ToeWellness Podiatry Clinic, where personalized treatment plans combine medical expertise with natural approaches for optimal nail restoration and long-term foot health.

 Nail Fungus Cures Instant Cures for Painful Nails and Fungus
Nail Fungus Cures Instant Cures for Painful Nails and Fungus