Key Takeaways
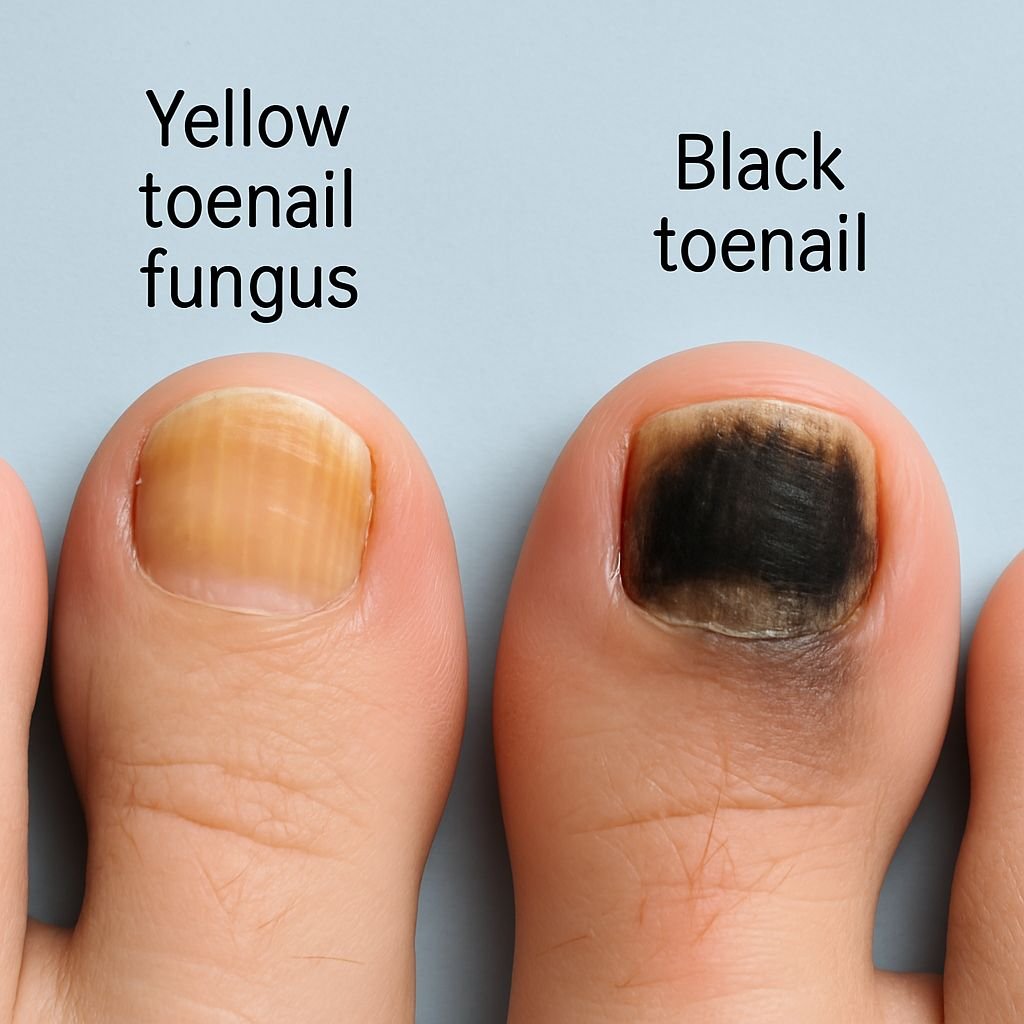
- Yellow toenail fungus indicates a common dermatophyte infection, while black discoloration may signal non-dermatophyte molds or other serious conditions requiring prompt medical attention.
- Toenail fungus affects 14% of the global population, with many people mistaking early symptoms for normal aging of the nail.
- Different colors of toenail fungus require different treatment approaches – yellow fungus typically responds to standard antifungals while black fungal infections may need specialized care.
- Visual diagnosis alone isn’t reliable – laboratory testing is essential to distinguish between fungal types and rule out serious conditions like melanoma that can also cause black nails.
- Early intervention significantly improves treatment outcomes, with complete nail healing typically taking 6-18 months as the infected nail grows out.
Toenail Fungus Colors: What Your Infected Nails Are Telling You
Discolored toenails often signal an underlying infection. When your once-clear nails begin changing color, the specific hue offers vital clues about what organism has taken up residence under your nail bed. Understanding these color variations isn’t just about aesthetics—it’s essential for proper treatment and preventing further complications.
Fungal nail infections, or onychomycosis, affect approximately 14% of the general population, with rates increasing significantly among older adults. The most common culprits behind these infections are dermatophytes, but other organisms like yeast and non-dermatophyte molds can also invade your nails, each leaving their distinctive color signature. While yellow discoloration represents the most commonly encountered fungal nail infection, black or dark discoloration presents a more complex diagnostic challenge that requires careful attention.
These infections typically develop slowly, allowing many people to dismiss early symptoms as normal aging or cosmetic issues until the infection becomes more severe and difficult to treat. By recognizing the specific characteristics of different colored toenail infections, you can seek appropriate treatment earlier and improve your chances of complete recovery.
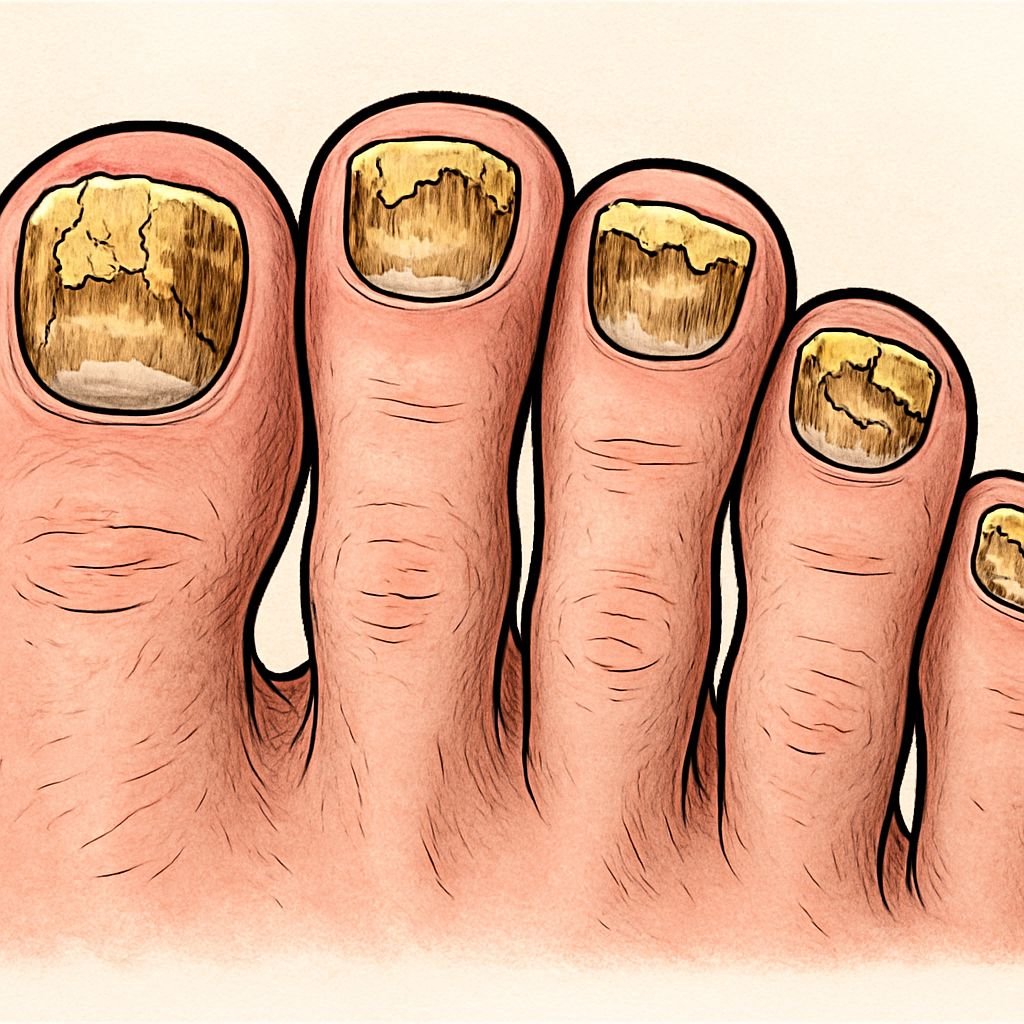
Yellow Toenail Fungus: The Most Common Type
Yellow discoloration represents the most prevalent form of toenail fungus, typically caused by dermatophyte fungi like Trichophyton rubrum. This fungus thrives in the warm, moist environment inside shoes, gradually working its way beneath your nail. The infection usually begins at the nail’s edge, creating a yellowish streak that slowly spreads toward the nail base. As the condition progresses, the entire nail may take on a uniform yellow-brown appearance, accompanied by thickening and brittleness.
What Causes Yellow Discoloration in Fungal Infections
Yellow nail discoloration occurs when dermatophyte fungi digest keratin, the primary protein in your nails. This metabolic process produces waste products that accumulate and stain the nail. Additionally, the fungi cause the nail to thicken as cellular debris builds up between the nail plate and nail bed. This combination of metabolic byproducts and structural changes creates the characteristic yellow-brown appearance. The intensity of the yellow color often corresponds to infection severity, with deeper yellow or amber tones indicating a more established infection that has penetrated deeper into nail tissues.
Distal and Lateral Subungual Onychomycosis: The Main Culprit
Distal and lateral subungual onychomycosis (DLSO) represents the most common form of yellow toenail fungus, accounting for about 85% of cases. This infection begins at the nail’s free edge or sides, creating the typical yellow streaking pattern that gradually spreads toward the cuticle. DLSO is characterized by hyperkeratosis—an abnormal thickening of the nail bed—and often causes the nail to separate from its bed (onycholysis). Unlike some other forms of onychomycosis, DLSO progresses relatively slowly, sometimes taking months or years to involve the entire nail. This slow progression often leads people to delay seeking treatment until the infection is well-established and more difficult to eradicate.
Early vs. Advanced Stages of Yellow Fungus
Recognizing yellow toenail fungus in its early stages significantly improves treatment outcomes. Initially, you might notice subtle yellow streaks at the nail’s edge, minimal thickening, and perhaps slight brittleness at the nail’s free margin. The nail still maintains much of its natural transparency and attachment to the nail bed during this phase. Left untreated, these early signs evolve into more pronounced symptoms as the infection matures.
Advanced yellow fungal infections transform the entire nail, creating a thickened, opaque, brittle structure with a distinctly yellow or yellow-brown color throughout. The nail surface may become irregular and crumbly, with debris accumulating underneath. Many patients also report a slight odor as the infection progresses. At this stage, the nail may become painful when pressure is applied, particularly when wearing shoes. Complete resolution at this advanced stage typically requires longer treatment courses and may even necessitate temporary or permanent nail removal in severe cases.
Black Toenail Fungus: When to Worry
Black or dark discoloration in toenails demands immediate attention, as it can indicate several different conditions ranging from benign fungal infections to potentially serious medical issues. Unlike the more common yellow toenail fungus, black discoloration often represents either a different class of infecting organisms or a serious complication of long-standing infection. The distinctive dark appearance occurs when pigment-producing organisms colonize the nail or when blood accumulates under the nail due to trauma or pressure.
Determining whether black nail discoloration stems from fungal infection rather than other causes represents a crucial diagnostic step. A subungual hematoma (blood under the nail) typically appears after obvious trauma, while melanoma (a serious form of skin cancer) often creates an irregular pattern of pigmentation. Fungal causes of black nails tend to create more uniform discoloration and are usually accompanied by other classic signs of nail fungus, including thickening, brittleness, and altered texture.
True Fungal Black Nails vs. Other Medical Causes
Black toenail discoloration requires careful assessment to determine its true cause. True fungal black nails typically develop from non-dermatophyte molds like Scytalidium, Scopulariopsis, and Aspergillus species, which produce melanin-like pigments that stain the nail. These infections often begin as small dark spots that gradually expand to cover larger portions of the nail. Unlike traumatic black nails which grow out over time, fungal black discoloration persists and may worsen if left untreated.
Several serious medical conditions can mimic the appearance of black toenail fungus. Subungual melanoma, though rare, presents as a dark streak or irregular black area under the nail and demands immediate medical evaluation. Bacterial infections, particularly Pseudomonas, can create greenish-black discoloration often mistaken for fungus. Chronic microtrauma from ill-fitting shoes can cause persistent blood accumulation that appears black. Distinguishing between these conditions is vital, as misdiagnosis and inappropriate treatment can delay proper care for potentially serious issues.
Non-Dermatophyte Molds: The Black Nail Culprits
Non-dermatophyte molds account for approximately 10-15% of fungal nail infections and are particularly associated with black discoloration. These environmental fungi typically enter through damaged nails and thrive in warm, moist conditions. Unlike dermatophyte fungi which specialize in keratin digestion, these molds are opportunistic invaders that often cause superficial infections. Species like Aspergillus niger produce distinctive black pigments as metabolic byproducts, directly staining the nail. These infections often prove more resistant to standard antifungal treatments, requiring specialized approaches and longer treatment durations.
The prevalence of non-dermatophyte mold infections varies significantly by geographic region, with higher rates in tropical and subtropical areas where environmental conditions favor their growth. Individuals with compromised immune systems, diabetes, or peripheral vascular disease face increased risk for these challenging infections. Professional testing becomes particularly important with suspected non-dermatophyte mold infections, as these organisms may require different treatment protocols than standard yellow fungal infections.
When Black Nails Require Immediate Medical Attention
Certain patterns of black toenail discoloration warrant urgent medical evaluation. A dark streak that extends from the cuticle to the nail tip, especially if it’s changing in appearance or accompanied by pigmentation of the surrounding skin, requires prompt assessment to rule out melanoma. Black discoloration accompanied by significant pain, drainage, or surrounding skin redness may indicate a severe infection requiring immediate treatment. Similarly, black nails in individuals with diabetes, circulation problems, or compromised immunity represent higher-risk situations that shouldn’t be self-diagnosed or treated at home.
Even when fungal infection seems the likely cause, professional evaluation ensures proper diagnosis and treatment. Many patients mistakenly self-treat for fungal infections when their black nail discoloration stems from other causes. This delay in appropriate care can allow underlying conditions to progress and potentially cause permanent damage. When in doubt, consult a healthcare provider, especially for black nail discoloration that appears suddenly, changes rapidly, or doesn’t respond to initial treatment approaches.
How Doctors Diagnose Different Toenail Fungus Types
Accurate diagnosis forms the cornerstone of effective toenail fungus treatment. While the color and appearance provide important diagnostic clues, definitive identification requires professional evaluation and laboratory testing. Medical professionals typically begin with a thorough visual examination, noting the pattern of discoloration, nail thickness, brittleness, and whether the infection appears to originate from the nail edge, surface, or base. This initial assessment helps narrow down potential causes but rarely provides enough information for a definitive diagnosis, particularly with black nail discoloration which has numerous possible origins.
Visual Examination and Lab Tests
Professional diagnosis typically begins with dermoscopy—examination using a specialized magnifying device that reveals subtle patterns invisible to the naked eye. This technique helps distinguish between fungal infection, trauma, and potential melanoma by highlighting specific color patterns and nail structure changes. Following visual assessment, your healthcare provider may take nail clippings or debris samples for laboratory analysis. The gold standard for fungal identification involves both direct microscopy with potassium hydroxide (KOH) preparation and fungal culture. KOH preparation provides rapid results by dissolving keratin to reveal fungal elements, while culture identifies the specific organism causing the infection, though it may take weeks to yield results.
Distinguishing Between Mold and Fungus
Laboratory testing plays a crucial role in differentiating between dermatophyte fungi (causing typical yellow infections) and non-dermatophyte molds (often responsible for black discoloration). Polymerase chain reaction (PCR) testing offers faster, more specific identification than traditional culture methods, detecting fungal DNA directly from nail samples. Histopathological examination using periodic acid-Schiff (PAS) staining provides another diagnostic approach, particularly valuable when distinguishing between fungal infection and other nail disorders.
The distinction between dermatophyte fungi and non-dermatophyte molds significantly influences treatment approaches. Dermatophytes typically respond well to standard antifungal medications, while non-dermatophyte molds often require combination therapies or alternative treatments. Without proper laboratory identification, treatment may target the wrong organism, leading to poor results and persistent infection. This diagnostic precision becomes especially important with black nail discoloration, where accurate identification directly impacts treatment success.
Treatment Options Based on Fungal Color and Type
Effective toenail fungus treatment requires a tailored approach based on the specific infecting organism, extent of infection, and patient factors such as overall health and medication tolerance. Yellow fungal infections caused by dermatophytes typically respond to standard antifungal medications, while black mold infections often require more specialized approaches. Treatment success depends not only on using the right medication but also on addressing underlying factors that contribute to fungal growth, such as moisture, compromised immunity, or nail trauma. A comprehensive treatment plan typically combines medication with environmental modifications and proper foot care techniques.
Prescription Treatments for Yellow Fungal Infections
Oral antifungal medications like terbinafine (Lamisil) and itraconazole (Sporanox) represent the most effective treatment for extensive yellow toenail fungus. These medications work by disrupting fungal cell membrane formation, with terbinafine achieving cure rates of 70-80% for dermatophyte infections. Treatment typically continues for 6-12 weeks, though the visible improvement continues for months afterward as the healthy nail grows out. Topical prescription solutions like ciclopirox (Penlac) or efinaconazole (Jublia) provide alternatives for milder infections or patients unable to take oral medications, though they require longer treatment periods of up to 48 weeks and generally achieve lower cure rates than oral therapy.
Specialized Approaches for Black Fungal Infections
Black toenail fungus caused by non-dermatophyte molds often requires modified treatment approaches due to inherent resistance to standard antifungals. For these infections, combination therapy frequently yields better results than monotherapy. A common approach combines oral terbinafine or itraconazole with topical antifungals containing ingredients effective against molds, such as ciclopirox or amorolfine. Treatment duration typically extends longer than for yellow fungal infections, often requiring 3-6 months of oral therapy and up to 12 months of topical treatment. In particularly resistant cases, medical professionals may recommend chemical or surgical nail removal followed by direct application of antifungal agents to the exposed nail bed. For more information on the differences between toenail mold vs fungus, consult expert resources.
Over-the-Counter Solutions: What Actually Works
For mild to moderate yellow toenail fungus, several over-the-counter options may provide benefit, though they typically work more slowly than prescription alternatives. Undecylenic acid (found in Fungi-Nail) and tolnaftate-based products show modest effectiveness against dermatophytes when applied consistently for several months. Tea tree oil stands out among natural remedies, with studies showing its antifungal properties against both dermatophytes and some non-dermatophyte molds. For maximum effectiveness, OTC treatments should be applied after thoroughly cleaning and gently filing the nail surface to improve penetration.
However, most over-the-counter treatments show limited efficacy against established infections, particularly those causing black discoloration or significant nail thickening. Research indicates that while these products may improve appearance and slow progression, complete cure rates remain below 20% when used as standalone therapy. They work best for very early infections or as supplementary treatments alongside prescription options. For black fungal infections specifically, over-the-counter products rarely provide adequate treatment, making professional care particularly important.
When Nail Removal Becomes Necessary
In cases of severe infection, particularly with extensive black discoloration or significant nail damage, temporary or permanent nail removal may become necessary. This approach eliminates the infected tissue entirely and allows direct application of antifungal agents to the nail bed. Nonsurgical removal using urea-containing ointments dissolves the nail gradually over several weeks, while surgical removal provides immediate access to the nail bed but requires local anesthesia and longer recovery. Following removal, the exposed nail bed receives direct antifungal treatment for several weeks to months, significantly increasing cure rates for otherwise resistant infections. For more information on different types of nail fungus, you can refer to this guide on nail fungus.
Preventing Toenail Fungus Before It Starts
Prevention remains significantly easier than treatment when it comes to toenail fungus. Creating an environment hostile to fungal growth represents your best defense against both yellow and black toenail infections. This preventative approach becomes especially important for individuals with previous infections, as recurrence rates can reach 50% without ongoing preventive measures. Consistently implementing proper foot hygiene, appropriate footwear choices, and avoiding high-risk environments substantially reduces your infection risk.
Those with compromised immunity, diabetes, or circulation problems should be particularly vigilant about prevention, as they face both higher infection rates and more complicated treatment courses. Regular professional foot examinations help identify potential issues before they develop into full-blown infections, particularly for high-risk individuals. Many people find that incorporating preventive measures into their daily routine provides long-term protection against these troublesome infections.
Daily Hygiene Practices That Make a Difference
Proper foot hygiene forms the cornerstone of fungal infection prevention. Thoroughly wash and completely dry your feet daily, paying special attention to the spaces between toes where moisture tends to accumulate. Keep nails short and straight across to prevent injury that creates entry points for fungi. Apply antifungal powder or spray to feet and inside shoes regularly if you’ve had previous infections or frequently visit high-risk environments.
Manage foot perspiration with moisture-wicking socks made from natural fibers or specialized synthetic materials designed to keep feet dry. Change socks whenever they become damp, particularly after exercise or on hot days. Consider using antiperspirant products specifically formulated for feet if excessive sweating remains problematic. These simple daily practices significantly reduce the warm, moist conditions that favor fungal growth and colonization.
Footwear Selection and Care
Your choice of footwear plays a crucial role in preventing toenail fungus. Select shoes made from breathable materials that allow air circulation and moisture evaporation. Avoid wearing the same pair of shoes on consecutive days, allowing each pair to dry completely between wearings. Disinfect shoes regularly with UV shoe sanitizers, antifungal sprays, or by washing machine-washable footwear on hot cycles. If you’ve experienced previous infections, consider dedicated shoe inserts with antifungal properties.
Reserve occlusive footwear like rubber boots or vinyl shoes for short-term use, as these materials trap moisture against your feet. Wear protective footwear in public showers, locker rooms, and pool areas to minimize exposure to environmental fungi. Select athletic shoes specifically designed for your activities, as proper fit and function reduce the risk of nail trauma that creates entry points for infection. These footwear practices create significant barriers against both yellow and black toenail fungus organisms.
High-Risk Environments to Avoid
Certain environments harbor particularly high concentrations of fungal organisms. Public swimming pools, locker rooms, communal showers, and spa footbaths represent common sources of fungal exposure. When visiting these locations, wear protective footwear and avoid barefoot contact with potentially contaminated surfaces. Similarly, nail salons with inadequate sanitation practices pose infection risks through contaminated tools. Choose facilities that properly sterilize equipment between clients or bring your own sanitized tools.
Home environments can also harbor fungal organisms. Regularly disinfect shower floors, bathroom mats, and other areas where bare feet frequently contact surfaces. If a household member has an active infection, implement separate bathmats and towels until the infection resolves. Wash potentially contaminated fabrics in hot water with antifungal additives like tea tree oil or vinegar to reduce fungal spore survival and transmission. These environmental precautions significantly reduce your exposure to both dermatophyte and non-dermatophyte organisms.
Recovery Timeline: What to Expect While Healing
Healing from toenail fungus requires patience, as visible improvement often lags behind the elimination of the infection itself. Most patients begin to notice subtle changes within the first 6-8 weeks of treatment, though these improvements may be limited to the new growth at the nail base rather than the already-infected portions. The most visible early sign typically involves clearer, more normal-appearing new growth emerging from the cuticle. Complete resolution depends on the growth rate of your nails, the extent of the original infection, and how consistently you follow the treatment protocol.
Understanding realistic timeframes helps maintain treatment motivation through what can be a lengthy recovery process. Yellow fungal infections typically show faster visible improvement than black infections caused by non-dermatophyte molds. Throughout recovery, continuing preventive measures remains essential, as reinfection can occur even as the nail improves. Many healthcare providers recommend continuing some preventive treatments even after apparent cure to minimize recurrence risk. For more details on effective strategies, explore this strategic journey to clear nails.
Visible Signs of Improvement
The first visible sign of successful treatment typically appears as clear, normal-colored nail growing from the cuticle. This healthy new growth gradually pushes forward, replacing the infected portion as the nail grows. For yellow infections, you may notice the discolored area receding toward the nail tip rather than expanding toward the cuticle. The nail’s texture often improves early in treatment, with decreased brittleness and crumbling even before color normalizes completely. Thickened nails may become noticeably thinner within 2-3 months of consistent treatment.
For black nail infections, improvement often manifests first as a lightening of the dark pigmentation, progressing from black to brown or gray before eventually clearing. The distinct border between infected and healthy nail becomes more apparent as treatment progresses. In both yellow and black infections, debris beneath the nail typically decreases, and any associated odor diminishes or disappears entirely. These progressive improvements serve as important motivation to continue treatment through the full recommended course.
How Long Until Complete Nail Replacement
Complete nail replacement, where the infected nail has grown out entirely and been replaced by healthy tissue, typically takes 6-18 months depending on the specific toenail affected and individual growth rates. The big toenail grows most slowly, requiring approximately 12-18 months for complete replacement, while smaller toenails may clear within 6-9 months. This timeframe reflects the natural growth rate of nails rather than any deficiency in treatment effectiveness, which is why patience becomes so essential during the recovery period. For more information on the causes of toenail color changes, you can check out this WebMD article.
Take Control of Your Foot Health Today
Don’t allow toenail fungus to progress unchecked—early intervention dramatically improves treatment outcomes and reduces complication risks. If you notice yellow streaking, black discoloration, or any suspicious changes in your toenails, seek professional evaluation to determine the specific cause and most appropriate treatment approach. Remember that while the color provides important diagnostic clues, definitive identification requires proper testing to distinguish between different fungal species and rule out other potential causes, particularly for black nail discoloration.
By combining appropriate medication, consistent preventive practices, and patience through the recovery process, you can overcome even established fungal nail infections. Your journey to healthier nails starts with recognizing the specific signs of infection and taking prompt action to address them. PureFeet’s specially formulated natural antifungal solutions can help support your treatment plan with proven botanical ingredients that target both yellow dermatophyte and black non-dermatophyte infections. For more information on understanding the symptoms and remedies, check out this guide on toe nail fungus symptoms and cures.
Frequently Asked Questions
Below are answers to common questions about black and yellow toenail fungus, providing clarification on crucial aspects of these conditions that many patients find confusing. For those seeking effective solutions, consider exploring effective approaches for toenail fungus treatment.
Can toenail fungus spread to other parts of my body?
Yes, toenail fungus can spread to other nails, the surrounding skin, and even fingernails if transferred through direct contact. Dermatophyte fungi causing yellow nail infections commonly spread to cause athlete’s foot or other dermatophyte infections elsewhere on the body. The risk of spread increases when you touch or manipulate infected nails and then contact other body areas without washing your hands. This self-spread occurs most commonly during nail trimming or filing.
To prevent spreading the infection, wash hands thoroughly after touching affected nails, use separate nail tools for infected and healthy nails, and disinfect tools after each use. Treat all affected areas simultaneously rather than addressing each infection separately. People with compromised immunity should be particularly careful about preventing spread, as fungal infections can become more widespread and difficult to control in these individuals.
Why did my yellow toenail fungus turn black?
A yellow fungal infection that turns black may indicate several possibilities. Most commonly, this color change suggests a secondary infection with non-dermatophyte molds that produce dark pigments, essentially representing a mixed infection with multiple organisms. Prolonged infection can also lead to debris accumulation and nail damage that appears darker over time. In some cases, bleeding beneath the nail from pressure or trauma can create black discoloration that overlays the existing yellow fungal infection. For more information on treatment options, you can explore effective approaches for toenail fungus treatment.
This color transition warrants professional evaluation, as treatment approaches may need adjustment to address the changing infection profile. The emergence of black coloration in a previously yellow infection may indicate increasing resistance to current treatments or deteriorating nail health requiring more aggressive intervention. Your healthcare provider might recommend additional testing to identify any new organisms and modify your treatment plan accordingly. For more information on nail fungus, you can explore this guide on different types of nail fungus.
Is black toenail fungus more dangerous than yellow fungus?
Black toenail fungus isn’t inherently more dangerous than yellow fungus, but it often presents greater treatment challenges and requires more careful differential diagnosis. Non-dermatophyte molds causing black discoloration typically show greater resistance to standard antifungal medications, potentially resulting in longer treatment courses and lower cure rates. The primary concern with black nail discoloration lies in ensuring it truly represents fungal infection rather than more serious conditions like melanoma that also create dark pigmentation under the nail. For more information on diagnosis, check out this nail fungus diagnosis guide.
Both yellow and black fungal infections can lead to permanent nail damage if left untreated, particularly in individuals with compromised circulation or immunity. Both types also have similar potential for spreading to other nails or skin areas. The key difference lies not in their inherent “danger” but in the diagnostic precision required for black discoloration and the potentially more complex treatment approaches needed for non-dermatophyte mold infections.
Can I treat different colored toenail fungus with the same medication?
Different colored toenail fungus often requires tailored treatment approaches based on the specific infecting organism. Yellow fungal infections caused by dermatophytes typically respond well to standard antifungal medications like terbinafine and itraconazole. Black fungal infections caused by non-dermatophyte molds often show resistance to these standard treatments, requiring combination approaches, longer treatment durations, or alternative medications with broader activity against molds.
Using the wrong treatment approach based solely on over-the-counter availability rather than proper diagnosis can lead to treatment failure and worsening infection. This highlights the importance of professional evaluation and laboratory testing to identify the specific organism before beginning treatment. Some newer broad-spectrum antifungals show activity against both dermatophytes and non-dermatophyte molds, but these typically require prescription and should be used under medical supervision for optimal results.
How can I tell if my black toenail is fungus or a bruise?
Distinguishing between fungal infection and subungual hematoma (bruising under the nail) requires careful observation of several factors. Bruising typically appears suddenly following trauma, while fungal discoloration develops gradually over weeks or months. Bruised nails generally maintain their normal thickness and texture, while fungal infections usually cause thickening, brittleness, and altered surface texture. As a bruise grows out, you’ll see a clear line of demarcation moving forward with nail growth, while fungal discoloration tends to expand rather than simply grow out.
If the dark area remains stationary as the nail grows, suspect fungus; if it moves forward with nail growth, it’s more likely a bruise. Bruising typically creates a more uniform purple-black color, while fungal discoloration may appear more irregular or patchy. When uncertainty exists, professional evaluation provides the most reliable assessment, as dermoscopy and other specialized examination techniques can typically distinguish between these conditions definitively.
Remember that both conditions can occasionally occur simultaneously—trauma that causes bruising can also create entry points for fungal organisms. If a presumed bruise doesn’t grow out as expected or develops other fungal characteristics like thickening or brittleness, reevaluation becomes necessary. Similarly, if a black discoloration appears in multiple toes without history of trauma, fungal infection becomes more likely than coincidental bruising of several nails.
Taking charge of your foot health means recognizing potential problems early and seeking appropriate care rather than relying solely on self-diagnosis. When in doubt about the cause of nail discoloration, consult a healthcare professional for proper evaluation and treatment recommendations. Your diligence today prevents more significant problems tomorrow.
Black and yellow toenail fungus can be quite concerning due to their unsightly appearance and potential health implications. Understanding the differences between these types of fungal infections is crucial for effective treatment. Black toenail fungus often results from trauma or injury to the nail, while yellow toenail fungus is typically caused by a fungal infection. For those seeking treatment options, exploring home treatment vs professional therapy can provide valuable insights into managing these conditions effectively.

 Nail Fungus Cures Instant Cures for Painful Nails and Fungus
Nail Fungus Cures Instant Cures for Painful Nails and Fungus