Key Takeaways
- Visual signs of nail fungus include yellowing, thickening, and brittleness, but professional testing is needed for accurate diagnosis
- Dermatologists use multiple testing methods including KOH preparations and fungal cultures to confirm nail fungus infections
- Self-diagnosis risks treating the wrong condition, as psoriasis and other disorders can mimic fungal infection symptoms
- Lab testing costs typically range from $50-$200 depending on the method, but are essential for effective treatment
- The NailWell Fungus Test Kit offers convenient at-home sample collection with laboratory-grade analysis for those seeking professional results without an immediate doctor visit
That yellowish, thickened nail might be fungus—or it could be something else entirely. Without proper testing, you’re simply guessing at a treatment that may waste your time and money. Let’s cut through the confusion and explore how professionals diagnose nail fungus with certainty, giving you the knowledge to take effective action.
Nail fungus affects approximately 10% of the general population and up to 50% of people over age 70. Despite its prevalence, many sufferers attempt self-diagnosis and treatment without understanding what they’re dealing with. The team at NailWell Fungus Test Kit has analyzed thousands of samples and found that nearly 30% of suspected “fungal infections” are actually other conditions requiring completely different treatments.
Nail Fungus Warning Signs: How to Spot the Problem
Before diving into testing methods, it’s important to recognize the potential signs that might warrant professional evaluation. While visual symptoms alone aren’t definitive, they serve as important indicators that something isn’t right with your nails.
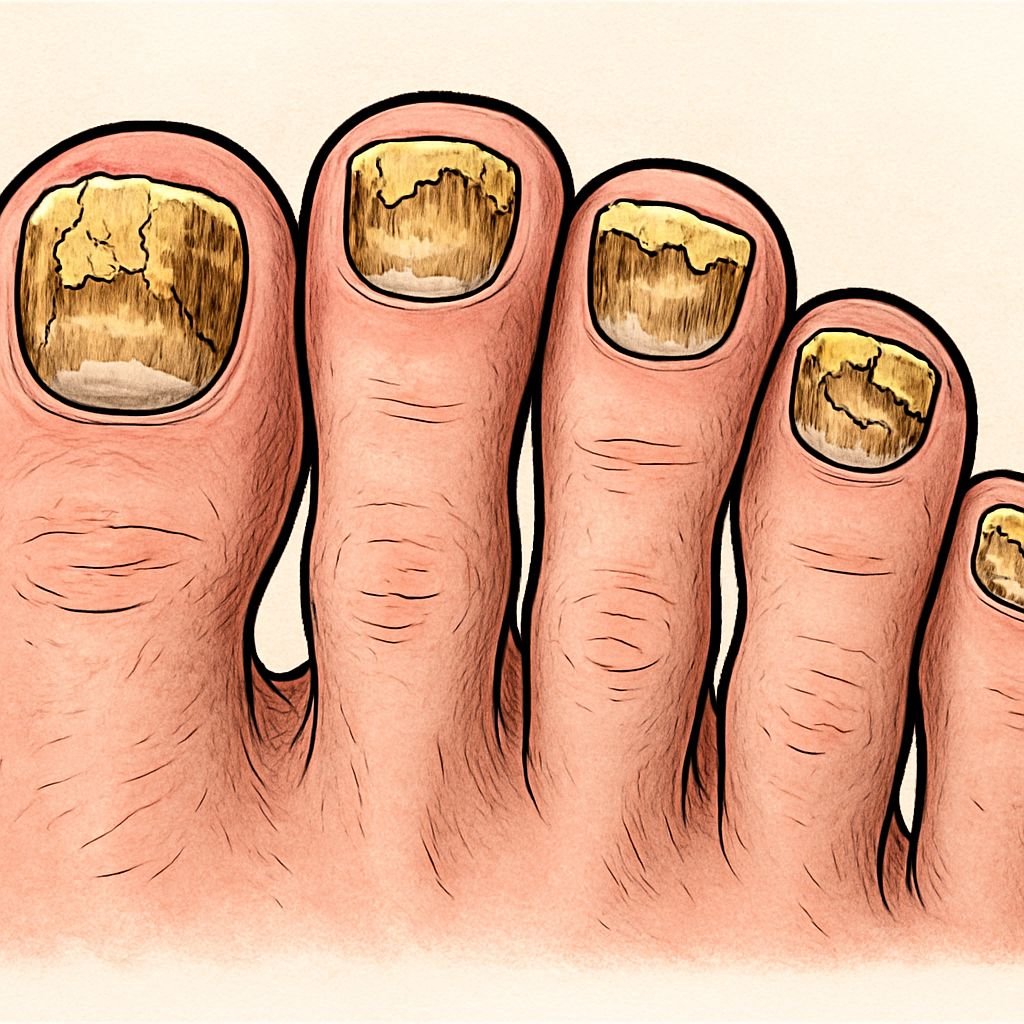
Discolored or Thickened Nails: The First Red Flag
The most common initial sign of nail fungus is discoloration. Your nail might develop yellow, white, or brown patches that gradually spread. As the infection progresses, nails typically become thickened, distorted, and brittle. This thickening occurs because the fungus causes debris to build up under and within the nail plate, creating that characteristic rough, thickened appearance that many sufferers find embarrassing.
Fungal infections often begin at the tip or side of the nail and slowly work their way toward the cuticle. This progression pattern—from nail edge inward—is one clue that dermatologists look for when making an initial visual assessment. When multiple nails show similar patterns of discoloration and thickening, the likelihood of fungal infection increases.
Beyond Appearance: Pain, Odor, and Spreading Infection
Beyond visual changes, nail fungus can create discomfort. Thickened nails may become painful when pressure is applied, such as when wearing shoes or performing daily activities. Some people experience a slightly foul odor emanating from the affected nails, particularly as debris accumulates. If left untreated, the infection can spread from one nail to another or even to surrounding skin, causing athlete’s foot in cases involving toenails.
The progression pattern matters too. Fungal infections typically don’t improve on their own—they gradually worsen without proper treatment. If you notice your symptoms steadily advancing over weeks or months, this persistence suggests a fungal pathogen rather than a temporary injury or reaction.
Distinguishing Fungus from Other Nail Conditions
Several conditions can mimic fungal infections, making self-diagnosis problematic. Psoriasis often affects nails, causing pitting, discoloration, and separation from the nail bed that looks remarkably similar to fungus. Bacterial infections, contact dermatitis, and even certain systemic diseases can produce nail changes that the untrained eye might mistake for fungus.
Traumatic injuries to nails can cause discoloration and thickening that persists for months as the nail grows out. Unlike fungal infections, however, these traumatic changes don’t spread to other nails and generally show a clear demarcation between affected and normal nail as growth occurs. The distinction between these lookalike conditions is precisely why laboratory testing becomes so crucial for proper treatment.
Condition Comparison: Nail Fungus vs. Common Mimics
Nail Fungus: Progressive discoloration, thickening, crumbling edges, multiple nails may be affected, doesn’t improve without treatment
Psoriasis: Pitting, salmon-colored patches, may affect skin elsewhere on body
Trauma: History of injury, doesn’t spread to other nails, grows out with time
Bacterial Infection: Often painful, may have pus, warmer to touch than fungal infections
Professional Diagnosis Methods That Get Results
When it comes to nail fungus, guesswork isn’t enough. Professional testing methods have been developed specifically to identify fungal pathogens with precision, allowing for targeted treatment approaches. These diagnostic techniques range from simple in-office procedures to sophisticated laboratory analyses.
Visual Examination by Healthcare Providers
The diagnostic journey typically begins with a thorough visual examination by a dermatologist or podiatrist. These specialists have evaluated thousands of cases and can often make preliminary assessments based on the characteristic patterns of fungal infections. They’ll examine the color, texture, and distribution of changes across your nails, looking for telltale signs like proximal spreading, subungual debris, and onycholysis (separation of the nail from the nail bed).
During this examination, healthcare providers will also look for clues that might suggest alternative diagnoses. They’ll ask about your medical history, occupation, hobbies, and previous treatments you’ve attempted. While this visual assessment provides valuable information, responsible practitioners rarely rely on visual diagnosis alone—they’ll confirm their suspicions with one or more laboratory tests.
KOH Preparation: The Quick First Test
The potassium hydroxide (KOH) preparation is typically the first laboratory test performed when nail fungus is suspected. This relatively simple procedure involves collecting nail clippings or debris from under the nail and placing them on a microscope slide with potassium hydroxide solution. The KOH dissolves keratin in the sample, making fungal elements more visible under a microscope.
During microscopic examination, the healthcare provider looks for branching fungal filaments called hyphae or small round fungal spores. The presence of these structures strongly supports a fungal infection diagnosis. KOH preparation can be completed during your office visit, providing same-day preliminary results in many cases.
While this test offers quick results and is relatively inexpensive (typically $50-75), it has limitations. KOH preparation cannot identify the specific type of fungus causing the infection, and false negatives can occur if the sample doesn’t contain enough fungal elements. Despite these limitations, it remains a valuable first-line diagnostic tool.
Fungal Culture: Gold Standard for Accurate Identification
For more definitive diagnosis, healthcare providers often order a fungal culture. This test involves placing nail samples on special growth media designed specifically for fungi. The samples are then incubated for up to several weeks, allowing any fungal organisms present to grow and multiply.
Fungal cultures offer two significant advantages over KOH testing. First, they can identify the specific type of fungus causing the infection—whether it’s a dermatophyte (the most common cause), yeast, or non-dermatophyte mold. Second, cultures can detect viable fungi even when they’re present in very small numbers, reducing false negatives.
The downside of fungal cultures is the waiting period. While some fast-growing fungi might be identified within a week, cultures are typically monitored for up to four weeks before being declared negative. This delay can be frustrating when you’re eager to begin treatment, but knowing exactly what organism you’re dealing with enables your healthcare provider to select the most effective medication.
PCR Testing: Advanced DNA Detection
Polymerase Chain Reaction (PCR) testing represents the cutting edge of nail fungus diagnostics. This molecular technique detects fungal DNA in nail samples, offering both speed and precision that traditional methods can’t match. PCR can identify the specific fungus species within 1-3 days, compared to the weeks required for culture growth.
PCR testing is particularly valuable for patients who have already begun antifungal treatment, as it can detect fungal DNA even when viable organisms aren’t present. This makes it useful for confirming infections in cases where cultures might yield false negatives. The technology also requires smaller nail samples, making the collection process more comfortable for patients with limited nail tissue available. For those considering alternatives, learn more about fungal toenail surgery alternatives.
The primary drawback of PCR testing is cost, which typically ranges from $150-200. However, many patients find the additional expense worthwhile when weighed against the time saved and the precision of results. Some insurance plans now cover PCR testing for nail fungus, recognizing its value in guiding effective treatment.
Histopathology: When Other Tests Are Inconclusive
In challenging cases where KOH preparations and cultures yield unclear results, healthcare providers may recommend histopathological examination. This procedure involves taking a small biopsy of the nail bed or nail plate and examining thin sections under a microscope after special staining procedures that highlight fungal elements.
Histopathology is particularly useful for distinguishing between fungal infections and conditions that mimic them, such as psoriasis or lichen planus. The microscopic examination can reveal characteristic patterns of tissue disruption and inflammation that help confirm or rule out various diagnoses. For more information on fungal infections, you can visit the Cleveland Clinic’s guide on toenail fungus.
While highly accurate, histopathology is generally reserved for complex cases due to its invasive nature and higher cost. Most nail fungus cases can be diagnosed effectively using the less invasive methods described earlier.
At-Home Sample Collection: Is It Reliable?
The growing demand for convenient healthcare solutions has led to the development of at-home nail fungus testing kits. These kits allow you to collect nail samples in the privacy of your home and mail them to a laboratory for professional analysis. While not a replacement for comprehensive medical care, they offer a practical first step for those unable to visit a healthcare provider immediately. For more advanced cases, consider exploring professional therapy options to ensure effective treatment.
The NailWell Fungus Test Kit has revolutionized access to laboratory testing by providing medical-grade collection tools and detailed instructions that help ensure viable samples. When properly collected and promptly shipped, these samples can yield results comparable to those obtained in clinical settings, giving patients valuable information before deciding on treatment approaches.
Mail-In Lab Tests: How They Work
At-home nail fungus testing kits typically include sterilized collection tools, sample containers, detailed instructions, and prepaid shipping materials. Users collect small nail clippings or debris following specific guidelines, then seal the samples and mail them to the laboratory. Within 3-7 days of receiving your samples, the laboratory performs professional testing—usually KOH examination, PCR, or both—and provides results electronically or by mail. For more information on effective treatments, check out these effective approaches for toenail fungus treatment.
Limitations of Self-Collection Methods
While convenient, at-home collection has inherent limitations compared to clinical collection. Sample quality varies significantly based on the user’s ability to follow instructions precisely. Taking samples from the wrong area of the nail or insufficient sample quantity are common issues that can lead to inconclusive results.
The delay between collection and laboratory processing may affect sample viability, particularly for culture-based tests. Environmental contamination is another concern, as non-sterile home conditions might introduce organisms that weren’t actually present in the nail. For a deeper understanding of these issues, explore our guide on home treatment vs. professional therapy.
Interpretation of results without professional guidance presents another challenge. While reputable testing services provide detailed explanations, these cannot replace the nuanced interpretation offered by healthcare providers who can consider your complete medical picture.
Despite these limitations, at-home testing can serve as a useful screening tool, especially for individuals with limited access to specialty care or those seeking preliminary information before committing to in-person appointments.
- Advantages of at-home testing include convenience, privacy, and lower initial cost
- Professional laboratory analysis provides reliable results comparable to clinical testing
- At-home collection is best viewed as a first step, not a complete replacement for medical care
- Results should ideally be discussed with a healthcare provider who can recommend appropriate treatment
- Some insurance plans now cover mail-in laboratory testing when ordered by a healthcare provider
What to Expect During Your Nail Fungus Test
The testing process itself can feel mysterious if you’ve never experienced it before. Understanding what to expect helps reduce anxiety and ensures you’re properly prepared. Whether you’re visiting a healthcare provider or using an at-home collection kit, the basic principles remain similar.
Preparation Steps Before Your Appointment
For the most accurate test results, avoid using antifungal treatments for at least one week before sample collection. These medications, even over-the-counter creams, can suppress fungal growth enough to cause false negative results without actually curing the infection. Similarly, nail polish and artificial nails should be completely removed at least 24-48 hours before testing to prevent chemical interference with diagnostic procedures.
If you’re seeing a healthcare provider, bring a list of all treatments you’ve previously tried, including home remedies and prescription medications. Note how long you’ve had symptoms and whether they’ve changed or spread over time. This information helps your provider interpret test results within the context of your complete clinical picture.
The Sample Collection Process
Nail fungus testing requires physical samples from your affected nails. For most tests, this involves collecting nail clippings and/or debris from under the nail. The healthcare provider typically uses specialized tools like small curettes or nail clippers to gather material from the most likely areas to contain fungal elements—usually the area where the healthy nail meets the affected portion.
The sample collection process is generally quick, taking just a few minutes per affected nail. While you might experience mild discomfort during collection, especially if your nails are painful or sensitive due to the infection, the procedure shouldn’t be painful. Your provider will focus on collecting material from the most severely affected nails, as these are most likely to yield definitive results.
Waiting Period and Result Timeline
After sample collection, the waiting begins. The time to results varies dramatically depending on which testing method is used. KOH preparations can provide preliminary results during the same office visit, typically within 15-30 minutes. PCR testing usually delivers results in 1-3 business days after the laboratory receives your samples. Fungal cultures take the longest, requiring 2-4 weeks of incubation to confirm negative results, though positive results may be available sooner if rapid fungal growth occurs.
Your healthcare provider should clearly communicate how and when you’ll receive results. Many practices now use patient portals to deliver test results electronically, while others may schedule follow-up appointments or phone calls to discuss findings. If you’ve used an at-home collection kit, results are typically delivered via email or through the testing company’s secure online platform.
Understanding Your Test Results
Receiving your test results is just the beginning—understanding what they mean is equally important. Lab reports can be confusing with their technical language and numerical values, but learning to interpret them empowers you to participate actively in treatment decisions. For more detailed information on conditions like nail fungus, you can visit the Cleveland Clinic’s resource on toenail fungus.
Reading Lab Reports: Positive vs. Negative Results
A positive result confirms the presence of fungal elements in your nail sample. Lab reports typically specify whether fungal hyphae (filaments), spores, or both were identified. The report may also indicate the relative quantity of fungal elements observed, using terms like “rare,” “few,” “moderate,” or “numerous.” These quantitative assessments can help gauge infection severity but don’t necessarily predict treatment difficulty.
A negative result indicates that no fungal elements were detected using the testing method employed. However, a single negative result doesn’t definitively rule out fungal infection. False negatives occur in approximately 5-15% of cases due to sampling errors, inadequate specimen quantity, or previous use of antifungal products. If clinical suspicion remains high despite negative results, your healthcare provider may recommend additional testing using different methods.
Common Fungal Culprits and Their Treatment Implications
When fungal culture or PCR testing is performed, your results will likely identify the specific organism causing your infection. Dermatophytes (particularly Trichophyton rubrum and Trichophyton mentagrophytes) cause approximately 80% of nail fungus infections and generally respond well to standard antifungal treatments. Candida species, a type of yeast, more commonly affect fingernails and may require different treatment approaches than dermatophyte infections.
Non-dermatophyte molds like Scopulariopsis, Fusarium, and Aspergillus represent approximately 10-15% of nail fungus cases and often prove more resistant to standard treatments. Identifying these organisms through culture or PCR testing is crucial because they may require combination therapy or alternative medications. Knowing exactly what you’re dealing with allows for targeted treatment that addresses your specific pathogen rather than a one-size-fits-all approach.
When to Request Additional Testing
If your initial test results are negative but your symptoms persist or worsen, don’t hesitate to request additional testing. Consider asking for a different type of test than was initially performed—for example, if KOH preparation was negative, a fungal culture or PCR test might provide more definitive results. Repeat testing is particularly important if you’ve been using antifungal treatments that might have suppressed but not eliminated the infection. Learn more about home treatment vs professional therapy to understand your options better.
For challenging cases, consultation with a dermatologist or podiatrist specializing in nail disorders can be invaluable. These specialists have extensive experience interpreting test results in the context of clinical presentations and can recommend advanced diagnostic techniques when standard approaches yield inconclusive results. Remember that accurate diagnosis is the foundation for effective treatment—it’s worth the extra effort to get it right.
When Self-Diagnosis Goes Wrong
The internet is filled with home remedies and over-the-counter solutions for supposed nail fungus, but treating without proper diagnosis is a gamble that rarely pays off. Many people waste months or even years applying ineffective treatments to conditions that weren’t fungal infections in the first place. This misguided approach not only wastes time and money but may actually worsen the underlying condition. For effective solutions, consider exploring professional therapy options instead of relying solely on home treatments.
Risks of Treating Without Proper Testing
Treating a misdiagnosed condition can mask symptoms while allowing the true problem to progress. For example, applying antifungal treatments to nails affected by psoriasis might temporarily reduce secondary infections but won’t address the underlying inflammatory condition. This delay in proper treatment can lead to permanent nail damage or spread to surrounding tissues.
Many antifungal medications, especially oral prescriptions, carry potential side effects including liver stress, skin reactions, and interactions with other medications. Exposing yourself to these risks without confirming a fungal infection through testing is unnecessary and potentially harmful. Even over-the-counter treatments can cause contact dermatitis or allergic reactions that complicate your condition and make accurate diagnosis more difficult when you eventually seek professional care.
Conditions Commonly Mistaken for Nail Fungus
Nail psoriasis affects approximately 50% of people with psoriasis and frequently mimics fungal infections with symptoms like pitting, discoloration, thickening, and separation from the nail bed. The key difference is that psoriasis often affects multiple nails symmetrically and may be accompanied by skin lesions elsewhere on the body. Only laboratory testing can reliably distinguish between these conditions, and treatments differ dramatically.
Lichen planus, contact dermatitis, bacterial infections, and even certain cancers can present with nail changes similar to fungal infections. Traumatic injuries to nails can cause persistent discoloration and thickening that looks remarkably similar to fungus but requires no antifungal treatment. These conditions require their own specific treatments, which is why professional diagnosis through proper testing is so crucial before beginning any therapeutic regimen.
Perhaps most concerning, melanoma (a type of skin cancer) sometimes presents as a dark streak or discoloration in the nail that might be mistaken for fungal infection. This dangerous misdiagnosis could delay life-saving treatment. When in doubt about any unusual nail changes, particularly those involving dark discoloration, professional evaluation is essential.
Next Steps After Diagnosis
Once you’ve confirmed nail fungus through laboratory testing, it’s time to develop a treatment plan tailored to your specific situation. The diagnosis process provides valuable information that guides treatment selection, including the type of fungus involved, infection severity, and whether multiple nails are affected. Armed with this knowledge, you and your healthcare provider can select the most appropriate intervention with the highest likelihood of success. For more on treatment options, explore prescription treatments for toenail fungus.
Treatment Options Based on Test Results
For confirmed dermatophyte infections (the most common type), treatment options include topical solutions like ciclopirox (Penlac) or efinaconazole (Jublia), oral medications such as terbinafine (Lamisil) or itraconazole (Sporanox), or combination approaches. The specific fungal species identified through testing helps determine which medication will be most effective. For example, Trichophyton rubrum typically responds well to terbinafine, while some non-dermatophyte molds may require alternative approaches like combination therapy or longer treatment durations.
The extent and severity of infection, documented during diagnosis, influences whether topical treatments alone are sufficient or if oral medication is necessary. Mild, superficial infections limited to the nail tips might respond to topical solutions, while infections involving the nail matrix or multiple nails typically require oral therapy. For particularly resistant cases, your provider might recommend nail avulsion (removal) followed by topical treatment applied directly to the nail bed.
Follow-Up Testing to Confirm Treatment Success
Successful treatment doesn’t just mean improved nail appearance—it means complete eradication of the fungal infection. Follow-up testing after completing your treatment regimen confirms whether the fungus has been eliminated or if additional therapy is needed. This post-treatment testing is particularly important because nails grow slowly, and visual improvement lags behind actual fungal clearance by months.
Most healthcare providers recommend follow-up testing 3-6 months after completing treatment. This timing allows sufficient opportunity for the medication to work while catching any persistent infection before it causes significant regrowth of visibly affected nail. If follow-up tests remain positive despite treatment, your provider might recommend a different medication, longer treatment duration, or combination therapy based on your specific fungal strain and infection characteristics.
Your Action Plan for Healthy Nails
Addressing nail fungus requires a comprehensive strategy that extends beyond just getting tested. First, seek professional testing through your healthcare provider or a reputable at-home testing service like NailWell Fungus Test Kit. Commit to completing the full course of treatment recommended based on your results—even if visual improvement occurs earlier. Implement preventive measures like keeping feet dry, wearing breathable shoes, using antifungal powder in shoes, and never sharing nail tools. Schedule follow-up testing after treatment completion to confirm the infection is fully resolved. Finally, maintain vigilance through regular self-examination, catching any recurrence early when it’s easier to treat.
Frequently Asked Questions
Many patients have common questions about nail fungus testing that deserve clear, straightforward answers. Understanding these practical aspects helps you navigate the diagnostic process more confidently and make informed decisions about your care.
How much do nail fungus lab tests cost?
The cost of nail fungus testing varies by method and provider. KOH preparations typically cost $50-75 when performed in a medical office. Fungal cultures range from $75-150, while PCR testing generally costs $150-200. These prices reflect the laboratory fees only and don’t include the office visit or professional consultation fees that might apply. At-home collection kits with laboratory analysis typically range from $85-150, depending on the testing methods included.
Insurance coverage for nail fungus testing varies widely between plans. Many insurance providers cover diagnostic testing when ordered by a healthcare provider and deemed medically necessary. However, coverage for at-home collection kits is less common unless they’re specifically prescribed by your provider. Always check with your insurance company regarding coverage before proceeding with testing.
Nail Fungus Testing Cost Comparison
When considering nail fungus diagnosis and treatment, it’s important to compare costs across different testing methods and healthcare providers.
KOH Preparation: $50-75
Fungal Culture: $75-150
PCR Testing: $150-200
At-Home Collection Kit: $85-150
Histopathology: $150-300
Consider that while testing represents an upfront cost, it potentially saves money long-term by preventing wasted expenditure on inappropriate treatments. Knowing exactly what you’re dealing with allows for targeted therapy rather than a trial-and-error approach that might include unnecessary or ineffective products.
Can I get accurate results if I’ve been using antifungal cream?
Recent use of antifungal products significantly reduces test sensitivity by suppressing fungal growth without completely eliminating the infection. For optimal results, discontinue all antifungal treatments (prescription and over-the-counter) for at least 7-14 days before sample collection if medically feasible. If stopping treatment isn’t possible due to severe symptoms, inform your healthcare provider or note it on your at-home collection form so this factor can be considered when interpreting results. In cases where treatment cannot be paused, PCR testing offers an advantage because it detects fungal DNA even when viable organisms are suppressed by medication.
How long does nail fungus testing take?
The time from sample collection to results varies by testing method. KOH preparations provide immediate results during your office visit, typically within 15-30 minutes. PCR testing delivers results in 1-3 business days after laboratory receipt. Fungal cultures take longest, requiring 2-4 weeks for complete results, though positive findings may be reported earlier if growth is observed. When using at-home collection kits, add 2-3 days for shipping time to these estimates.
The testing timeline should factor into your treatment decisions. If you have severe symptoms requiring immediate intervention, your healthcare provider might recommend starting empirical treatment based on clinical appearance while awaiting definitive test results. This approach balances the need for prompt symptom relief with the importance of eventual diagnostic confirmation.
Remember that early, accurate diagnosis through proper testing is the foundation of effective nail fungus treatment. The temporary inconvenience of the testing process is far outweighed by the long-term benefits of targeted therapy based on confirmed results. Contact your healthcare provider or the NailWell Fungus Test Kit team today to begin your journey toward healthier nails with confidence and clarity.

 Nail Fungus Cures Instant Cures for Painful Nails and Fungus
Nail Fungus Cures Instant Cures for Painful Nails and Fungus