Key Takeaways
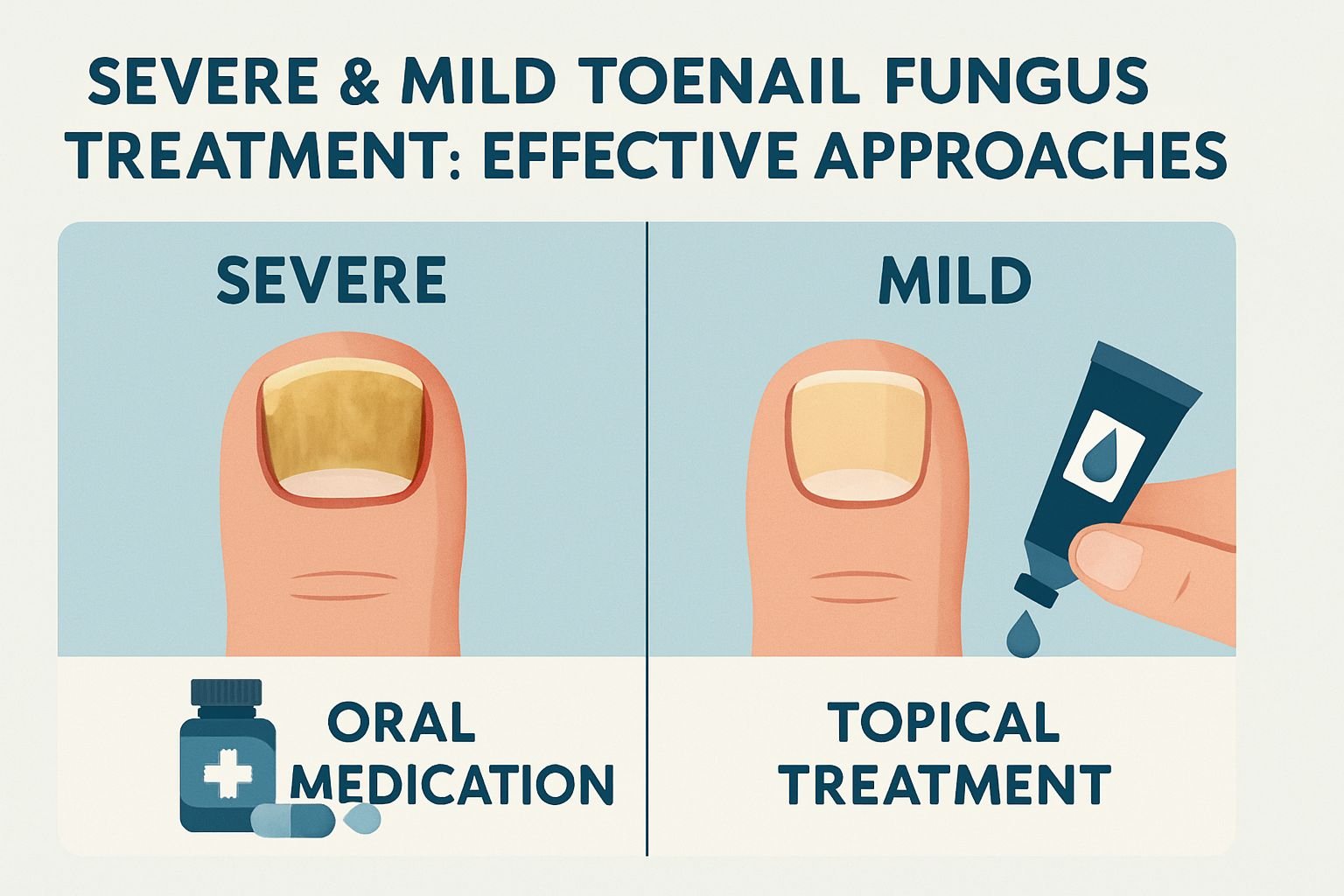
- Toenail fungus treatment varies significantly between mild and severe cases, with mild cases often responding to over-the-counter options while severe infections typically require prescription medications.
- Oral antifungal medications like terbinafine and itraconazole offer the highest cure rates (up to 70%) for severe fungal nail infections but come with potential side effects.
- Natural remedies including vinegar soaks, tea tree oil, and proper foot hygiene can effectively manage mild cases or serve as complementary treatments.
- Treatment timelines are lengthy, typically requiring 3-6 months for topical treatments and 6-12 months to grow a completely new, healthy nail.
- Prevention strategies like keeping feet dry, wearing breathable footwear, and practicing good foot hygiene are essential to avoid recurrence, which affects up to 50% of successfully treated cases.
Toenail fungus affects approximately 10% of the general population, with that number jumping to 50% in adults over 70. Finding the right treatment approach depends entirely on the severity of your infection and your overall health status.
Whether you’re dealing with a minor discoloration or a severely thickened, crumbling nail, there are evidence-based solutions available. At Nature’s Healing Path, we’ve researched the most effective conventional and natural approaches to help you finally clear this persistent condition.
Recognizing Toenail Fungus: From Mild to Severe Cases
Toenail fungus (onychomycosis) progresses through distinct stages, and identifying where you fall on this spectrum is crucial for selecting the appropriate treatment. The infection typically begins at the nail edge and slowly advances toward the cuticle, changing appearance as it progresses.
Early intervention significantly improves treatment outcomes. Research shows that treating fungal infections when they affect less than 50% of the nail results in success rates nearly twice as high compared to advanced cases.
- Mild cases: Slight discoloration (white or yellow spots), minimal thickening
- Moderate cases: Noticeable yellowing/browning across more than half the nail, moderate thickening, some brittleness
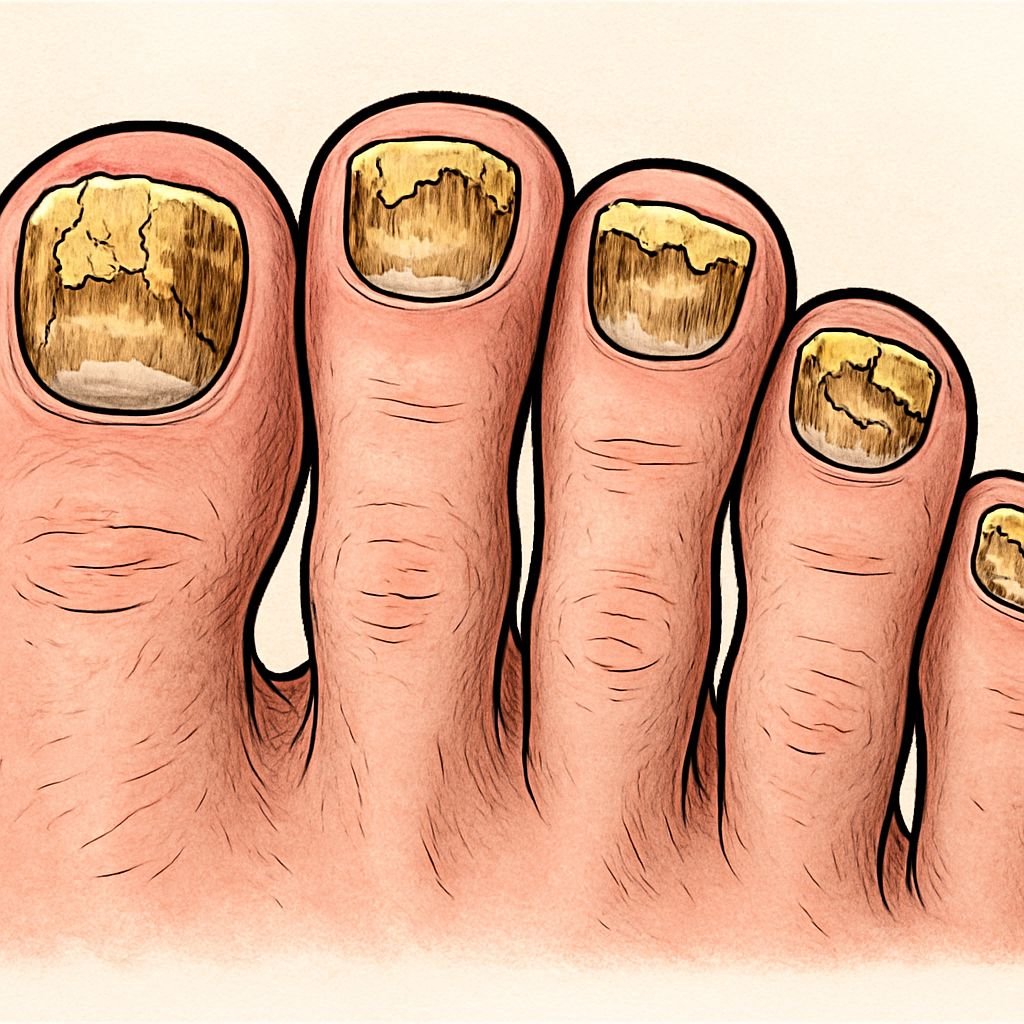
- Severe cases: Complete discoloration, significant thickening, crumbling nail edges, separation from nail bed, potential pain and odor
- Complicated cases: Spreading to multiple nails, surrounding skin infection (athlete’s foot), history of failed treatments
Visual Signs Your Toenail Has a Fungal Infection
The most recognizable signs of toenail fungus include progressive discoloration, typically beginning as white or yellow spots that eventually spread across the entire nail. As the infection advances, nails become thicker, more brittle, and may develop a distorted shape. This thickening occurs because the fungus triggers the nail to produce more keratin—the protein that forms nails—as a protective response.
Differences Between Mild and Severe Infections
Mild toenail fungus typically affects less than 50% of the nail and presents primarily as a cosmetic issue with minimal structural changes. These early-stage infections often respond well to topical treatments and diligent foot care practices.
Severe infections, by contrast, involve extensive nail involvement with significant thickening, discoloration throughout the entire nail, and structural deterioration. At this advanced stage, the nail may separate from the nail bed (onycholysis), develop ragged, crumbling edges, and occasionally cause discomfort when pressure is applied. The robust fungal colony established in severe cases creates a formidable barrier that topical treatments struggle to penetrate effectively.
- Treatment difficulty: Mild infections typically respond within 3-6 months; severe infections may require 12+ months of consistent treatment
- Treatment approach: Mild cases often respond to topical options; severe cases generally require oral medications
- Recurrence risk: Higher in severe cases (30-50%) compared to mild cases (10-20%)
When Fungus Becomes More Than a Cosmetic Issue
While often considered merely a cosmetic concern, untreated toenail fungus can develop into a legitimate health risk for certain populations. The thickened, distorted nails can create pressure points within shoes, leading to discomfort and potentially dangerous secondary infections, particularly for individuals with diabetes or compromised immune systems.
For people with diabetes, even minor foot injuries can escalate into serious complications due to reduced circulation and nerve function. A fungal infection creates entry points for bacteria, potentially triggering cellulitis—a spreading skin infection that can be dangerous without prompt treatment. Studies show diabetic patients with onychomycosis have a significantly higher risk of developing foot ulcers, with one study finding a 1.6 times greater risk compared to diabetics without fungal nail infections.
Why Toenail Fungus Happens and Who’s Most at Risk
Toenail fungus develops when dermatophytes—organisms that feed on keratin (the protein in nails and skin)—find their way underneath your toenail. These microscopic invaders thrive in warm, moist environments, which is why toenails are particularly vulnerable compared to fingernails.
The infection typically begins after exposure to contaminated surfaces like pool decks, public showers, or gym locker rooms. The fungus enters through tiny cuts or separations between your nail and nail bed that you might not even notice. Once established, the confined space between your nail and nail bed creates the perfect protected environment for fungal colonization.
Several factors significantly increase your susceptibility to developing toenail fungus. Age plays a crucial role, with adults over 60 experiencing infections at rates nearly seven times higher than younger individuals. This age-related vulnerability stems from naturally slower nail growth, reduced circulation to extremities, and a lifetime of potential nail trauma that creates entry points for fungi.
Common Causes of Fungal Nail Infections
The primary culprits behind toenail fungus are dermatophytes—specifically Trichophyton rubrum, which accounts for over 90% of cases. These organisms specialize in breaking down keratin, the protein that forms your nails. Less commonly, yeasts (like Candida) and molds may cause similar infections, particularly in people with compromised immune systems.
The infection cycle typically begins when your feet come into contact with fungal spores in warm, moist environments. Public swimming pools, shower floors, and locker rooms are notorious transmission points. The fungus enters through microscopic breaks in the skin or spaces between your nail and nail bed. Once established, the confined, protected space under your nail provides an ideal environment for fungal proliferation.
Lifestyle Factors That Increase Your Risk
Your daily habits significantly impact your vulnerability to toenail fungus. Consistently wearing tight, non-breathable footwear creates the warm, moist environment that fungi thrive in—essentially turning your shoes into incubators. Athletes and regular gym-goers face elevated risk due to frequent exposure to communal spaces combined with repetitive foot trauma and sweat-soaked footwear.
Poor circulation resulting from sedentary lifestyle choices reduces the delivery of infection-fighting cells to your extremities. This circulatory deficit, combined with reduced nail growth rates as we age, creates the perfect storm for fungal colonization. Studies show that individuals who wear occlusive footwear for 8+ hours daily have nearly double the infection rate compared to those who regularly allow their feet to breathe.
Medical Conditions That Make You More Susceptible
Certain health conditions dramatically increase your vulnerability to fungal nail infections. Diabetes stands out as a primary risk factor, with studies showing diabetic patients are 2.77 times more likely to develop onychomycosis compared to non-diabetics. This increased susceptibility stems from impaired circulation, elevated blood glucose levels that feed fungi, and peripheral neuropathy that prevents awareness of early symptoms.
Immune-compromising conditions—including HIV/AIDS, organ transplantation requiring immunosuppressants, and autoimmune disorders—create an environment where typically manageable fungal exposures can rapidly progress to established infections. Additionally, peripheral vascular disease restricts blood flow to extremities, limiting your body’s natural ability to fight early-stage infections before they become entrenched.
Prescription Treatments for Severe Toenail Fungus
Prescription Medication Comparison
Terbinafine (oral): 70% cure rate, 6-12 week course, potential liver strain
Itraconazole (oral): 65% cure rate, pulse therapy option, drug interactions
Ciclopirox (topical): 35% cure rate, 48 weeks of application, minimal side effects
Tavaborole (topical): 31% cure rate, better nail penetration, expensive
For those considering different options, it’s important to understand the differences between home treatment vs. professional therapy.For severe or resistant toenail fungus infections, prescription treatments offer the highest success rates. These medical-grade solutions utilize potent antifungal compounds that target the infection at its source. When over-the-counter options have failed or when the infection covers more than 50% of the nail, these stronger interventions become necessary.
The choice between oral and topical prescription options involves weighing efficacy against potential side effects. Your doctor will consider factors including your age, liver function, medication interactions, and infection severity when recommending the most appropriate treatment pathway. Complete resolution requires patience—even with prescription treatments, you’re committed to a months-long process as infected nail grows out and healthy nail replaces it.
Oral Antifungal Medications: The Most Effective Option
Oral antifungal medications represent the gold standard for treating severe toenail fungus, offering success rates of 60-75% compared to 20-35% for topical options. These medications work systemically, circulating through your bloodstream and reaching the nail bed from underneath—a significant advantage over topical treatments that struggle to penetrate the nail plate. The most commonly prescribed oral antifungals include terbinafine (Lamisil) and itraconazole (Sporanox).
Terbinafine typically requires a 12-week course of daily tablets and works by interfering with fungal cell membrane formation. It demonstrates particularly strong efficacy against the dermatophyte species that cause most toenail infections. Itraconazole offers the option of “pulse therapy”—one week of medication followed by three weeks without—which some patients find more manageable and potentially reduces side effect risks.
While effective, oral antifungals require liver function monitoring through blood tests before and during treatment. These medications may interact with other drugs including statins, anticoagulants, and certain antidepressants. The complete visual transformation of your nail may take 9-12 months as healthy nail slowly grows in, even though the fungus itself is eliminated much earlier in the treatment process.
Prescription-Strength Topical Solutions
Prescription topical antifungals provide targeted treatment directly to the infected nail while minimizing systemic side effects. These solutions contain higher concentrations of active ingredients than their over-the-counter counterparts, with formulations specifically designed to enhance penetration through the nail plate. Popular options include ciclopirox 8% (Penlac) and efinaconazole 10% (Jublia).
These medications require diligent application—typically daily for up to 48 weeks—and often include specific instructions like periodic nail debridement to maximize effectiveness. While convenience and safety profile represent advantages of topical treatments, they demonstrate significantly lower cure rates (25-45%) compared to oral options, particularly for infections involving the nail matrix or lunula (the white half-moon at the base of your nail).
Laser Treatment: What to Expect and Success Rates
Laser therapy presents an emerging option for toenail fungus that works by creating precisely targeted heat that destroys fungal structures while preserving surrounding tissue. This technology typically requires 3-4 sessions spaced weeks apart, with each painless treatment lasting approximately 10 minutes. The procedure generates controlled warming sensations without requiring anesthesia or recovery time.
Clinical evidence on laser effectiveness shows mixed results, with studies reporting improvement rates between 30-70%. The significant variation stems from differences in laser types, treatment protocols, and how “success” is defined. The FDA has cleared several devices for “temporary increase in clear nail” rather than complete fungal elimination, highlighting the modest expectations for this approach. For more information on toenail fungus treatment, you can visit the Cleveland Clinic’s website.
The primary advantages of laser treatment include the absence of systemic side effects and drug interactions. However, the substantial out-of-pocket cost (typically $800-$1,200 for a treatment series) and limited insurance coverage represent significant barriers for many patients. This option may be most appropriate for individuals who cannot tolerate oral medications or have experienced previous treatment failures.
When Surgical Removal Becomes Necessary
In rare cases where severe toenail fungus resists multiple treatment attempts or causes significant pain, surgical nail avulsion (complete removal) may become necessary. This procedure involves removing the entire nail plate under local anesthesia, allowing direct application of antifungal agents to the exposed nail bed or complete eradication of the severely infected nail.
Partial nail avulsion targets only the affected portion while preserving healthy nail, offering a less invasive alternative in appropriate cases. Following removal, an antifungal medication is typically applied to the exposed nail bed to eliminate remaining fungal elements, with the understanding that complete nail regrowth takes 12-18 months.
Natural and Over-the-Counter Solutions for Mild Cases
For mild toenail fungus infections that affect less than 50% of the nail, non-prescription approaches often yield satisfactory results. These accessible treatments balance reasonable effectiveness with minimal risk, making them ideal first-line options for early-stage infections.
While over-the-counter solutions typically work more slowly than prescription medications, they offer significant advantages: affordability, availability without doctor visits, and minimal side effect concerns. For optimal results, combine these treatments with the hygiene practices discussed later in this article.
Top 5 OTC Antifungal Products Worth Trying
The most effective over-the-counter treatments for toenail fungus contain ingredients clinically proven to combat fungal growth. Undecylenic acid (found in Fungi-Nail) creates an inhospitable environment for fungal reproduction with a 10-12% concentration. Studies show it effectively treats mild cases when applied consistently for 3-6 months.
Tolnaftate (in products like Tinactin) offers broad-spectrum antifungal activity and works particularly well for surrounding skin infections that often accompany nail fungus. Clotrimazole (Lotrimin) and miconazole (Desenex) inhibit ergosterol synthesis in fungal cell membranes, essentially compromising the organism’s structural integrity. For best results, these products should be applied to clean, dry nails twice daily. Learn more about prescription treatments for toenail fungus to explore other effective options.
Snakeroot extract, derived from plants in the sunflower family, has demonstrated effectiveness comparable to prescription ciclopirox in small studies. This natural antifungal compound requires thrice-weekly application for one month, twice-weekly application for the second month, and weekly application for a third month to achieve optimal results.
Essential Oils That Fight Fungal Infections
Several essential oils demonstrate promising antifungal properties for mild toenail infections. Tea tree oil stands out with substantial research supporting its effectiveness against Trichophyton rubrum—the fungus responsible for most nail infections. A 2013 study published in the Journal of Family Medicine and Primary Care found that twice-daily application of 100% tea tree oil resolved fungal infection in 18% of participants after six months, with 56% showing partial improvement.
Oregano oil contains thymol and carvacrol, compounds with documented antifungal properties. Studies indicate these components disrupt fungal cell membranes and inhibit growth. For application, these potent oils must be diluted with carrier oils like coconut or olive oil (typically 2-3 drops essential oil per teaspoon of carrier oil) to prevent skin irritation. Learn more about DIY oregano oil toenail fungus treatment methods.
Other essential oils showing antifungal promise include thyme oil, lavender oil, and clove oil. The effectiveness of these natural remedies increases when used consistently over several months and when combined with proper nail hygiene practices. For those interested in exploring more about these natural solutions, check out the best essential oil blends for nail fungus.
The Vinegar Soak Method: How to Do It Right
Vinegar soaks leverage the natural antifungal properties of acetic acid to create an acidic environment that inhibits fungal growth. This home remedy has accumulated considerable anecdotal support, though clinical studies remain limited. The optimal approach involves creating a solution of one part white vinegar to two parts warm water.
For maximum effectiveness, soak affected feet for 20 minutes daily, thoroughly drying between toes afterward. The process works gradually by altering the pH of your nail bed to make it less hospitable to fungal organisms. Some practitioners recommend adding a few drops of tea tree oil to enhance the antifungal properties of the soak.
Consistency is crucial—studies suggest daily soaking for at least three months provides the best chance of improvement. This method works well as a complementary approach alongside other treatments rather than as a standalone solution for anything beyond very mild cases.
When to Upgrade from Home Remedies to Medical Care
While home remedies and over-the-counter treatments offer reasonable options for mild cases, recognizing when to seek professional care prevents wasted time on ineffective approaches. If you’ve consistently applied non-prescription treatments for three months without noticeable improvement, it’s time to consult a healthcare provider for more potent options. For more information on transitioning from home treatment to professional therapy, explore the benefits of seeking medical care.
Similarly, if your infection worsens despite treatment—spreading to additional nails or causing increased pain, thickening, or nail separation—professional evaluation becomes necessary. Those with diabetes, peripheral vascular disease, or compromised immune systems should bypass home remedies entirely and seek medical treatment at the first sign of infection to prevent serious complications.
Daily Habits That Speed Up Healing and Prevent Reinfection
The success of any toenail fungus treatment—whether prescription or over-the-counter—depends heavily on complementary self-care practices. These daily habits create an environment where treatments can work more effectively and reduce the risk of reinfection, which affects up to 50% of successfully treated cases. For those interested in understanding more about effective treatments, you can explore rapid toenail fungus treatment options.
Incorporating these practices not only accelerates your current treatment’s effectiveness but establishes long-term habits that significantly reduce your vulnerability to future fungal infections. Many patients find that maintaining these routines becomes second nature after a few weeks. For those seeking additional natural remedies, exploring essential oil blends for nail fungus can be a beneficial addition to their routine.
Proper Foot Hygiene Techniques
Effective foot hygiene forms the foundation of successful fungal treatment. Wash feet daily with gentle soap, paying special attention to the spaces between toes where moisture accumulates. After washing, dry feet meticulously, using a separate towel from the one used for the rest of your body to prevent spreading the infection.
Apply an antifungal powder containing miconazole or tolnaftate to dry feet before putting on socks. This creates an additional protective barrier against fungal growth throughout the day. Change socks immediately if they become damp from sweat or external moisture, as fungal organisms thrive in humid environments.
Consider using moisture-wicking socks made from materials like bamboo, wool, or specialized synthetic fibers rather than cotton, which retains moisture against the skin. These advanced fabrics draw perspiration away from your skin, creating a drier environment that discourages fungal proliferation. For more insights, check out this article on toenail health for athletes.
The Right Way to Trim Infected Nails
Proper nail maintenance significantly impacts treatment effectiveness. Keep nails trimmed straight across and slightly shorter than the tip of your toe to reduce pressure and trauma. File down thickened areas gently with a disposable emery board after showering when the nail is softer—this improves topical treatment penetration by reducing the barrier thickness. For more information on effective treatments, explore the best prescription treatments for toenail fungus.
Disinfect nail tools after each use by soaking them in 70% isopropyl alcohol for 10 minutes or using a UV sanitizing device. Never share these tools with others, as this creates a direct transmission route for fungal organisms. Consider using disposable emery boards and replacing them weekly to eliminate cross-contamination risk.
Footwear Choices That Help Eliminate Fungus
Your shoes create the environment your feet live in for most of the day, making footwear selection crucial for treatment success. Choose breathable shoes made with mesh, canvas, or leather uppers that allow air circulation. Avoid synthetic materials that trap heat and moisture, creating perfect fungal incubators.
Alternate between at least two pairs of shoes daily, allowing each pair to thoroughly air out for 24 hours between wearings. This simple rotation reduces moisture accumulation by up to 40% according to dermatology research. During treatment, consider applying an antifungal spray or powder containing tolnaftate or miconazole to shoes before wearing them.
Open-toed footwear or sandals provide the maximum ventilation when appropriate for the setting and weather. At home, going barefoot allows maximum air exposure—but only if you don’t have diabetes or circulation issues, and only on clean surfaces that won’t reinfect your nails. For those dealing with persistent issues, exploring home treatment vs. professional therapy options can be beneficial.
Treatment Timeline: What to Expect During Recovery
Toenail fungus treatment requires patience—visible improvement occurs gradually as healthy nail grows in to replace infected portions. Understanding the typical timeline helps maintain motivation during the lengthy treatment process. For most people, complete resolution takes 6-12 months, reflecting the slow growth rate of toenails (approximately 1mm per month).
The infection itself may be eliminated much earlier, but the visual evidence remains until the damaged nail grows out fully. This disconnect between fungal death and visible improvement explains why many people abandon treatment prematurely, mistakenly believing it isn’t working when the biological process simply requires more time to manifest visibly.
Why Toenail Fungus Takes So Long to Clear
The stubborn nature of toenail fungus stems from several biological factors. Toenails grow exceptionally slowly—about 1-2mm per month compared to fingernails at 3-4mm—meaning even after the fungus is neutralized, the damaged nail takes 6-12 months to be completely replaced with healthy growth. This slow renewal process creates a frustrating lag between successful treatment and visible improvement.
Additionally, the nail plate’s dense keratin structure creates a formidable barrier that limits treatment penetration, particularly for topical medications. This protective shield that effectively keeps chemicals out of your nail also unfortunately keeps antifungal compounds from reaching the infection site efficiently. The nail bed’s limited blood supply further complicates treatment by reducing the delivery of oral medications and immune cells to the infection site.
Visible Signs of Improvement to Watch For
The first visible sign of successful treatment typically appears as a section of clear, healthy nail growth emerging from the cuticle. This healthy growth indicates the fungus is no longer active in the nail matrix (the area where new nail forms). Gradually, this clear growth advances forward, pushing the discolored, infected portion toward the tip of your toe.
Around months 3-4, you may notice the boundary between healthy and infected nail becoming more distinct, with the infected portion appearing more brittle. The previously yellow or brown discoloration may begin to fade slightly, though complete clarity won’t return until the entire infected portion grows out. Thickness typically improves gradually, with the new growth showing normal thickness while the older infected portion remains thickened. For those exploring natural remedies, consider trying DIY oregano oil treatments to support healthy nail growth.
How to Tell If Your Treatment Is Working
Beyond visual cues, several indicators suggest your treatment is effectively combating the fungal infection. Reduced nail brittleness represents an early positive sign, as the new growth emerging from your cuticle maintains structural integrity instead of crumbling. This improved strength often precedes visible color changes by several weeks. For more information on effective treatments, explore best prescription treatments for toenail fungus.
Documentation helps objectively track progress that might otherwise be difficult to perceive. Take monthly photos of the affected nails against the same background with consistent lighting. This creates a visual record that often reveals subtle improvements not noticeable day-to-day. Your healthcare provider may take nail clippings for periodic testing to verify the fungal burden is decreasing, providing biochemical confirmation that complements visual assessment.
Preventing Future Fungal Infections
Successfully treating toenail fungus represents only half the battle—preventing recurrence requires ongoing vigilance. Studies show recurrence rates of 10-50% within one year of successful treatment, highlighting the importance of preventive strategies. These preventive measures require minimal effort yet provide significant protection against future infections.
Most prevention strategies focus on creating an environment where fungal organisms cannot easily establish themselves. By incorporating these practices into your regular routine, you substantially reduce your vulnerability to reinfection while simultaneously improving overall foot health.
Creating an Environment Where Fungus Can’t Thrive
Fungi require specific conditions to flourish, and modifying your daily habits can create an inhospitable environment for these organisms. Keep feet clean and thoroughly dry, paying particular attention to the spaces between toes where moisture naturally accumulates. Consider using a hairdryer on the cool setting to ensure complete drying after showers.
Rotate your footwear to ensure each pair dries completely between uses, as shoes typically require 24+ hours to fully dry internally. For additional protection, use ultraviolet shoe sanitizers that kill up to 99.9% of fungal spores and bacteria within your footwear. These devices typically require 30-60 minutes of exposure per shoe and provide an additional layer of prevention for vulnerable individuals.
Protective Measures for Public Spaces
Public swimming pools, locker rooms, showers, and similar environments represent primary exposure points for fungal organisms. Wear water-friendly sandals or shower shoes in these locations to create a protective barrier between your feet and potentially contaminated surfaces. Studies show this simple practice reduces infection risk by up to 80% in communal settings.
Supplements That Boost Your Resistance to Fungal Infections
Several nutritional approaches may enhance your natural resistance to fungal infections. Probiotics containing Lactobacillus and Bifidobacterium species support your immune system’s ability to recognize and combat fungal invaders. Research indicates these beneficial bacteria may help maintain the balance between healthy and harmful microorganisms on your skin and nails. For more insights on maintaining toenail health, explore toenail health for athletes and the benefits of different activities.
When to See a Doctor About Your Toenail Fungus
While mild fungal infections often respond well to home treatment, certain situations warrant professional medical evaluation. If you have diabetes, circulatory problems, or an immune system condition, consult your healthcare provider at the first sign of toenail changes rather than attempting self-treatment.
Similarly, if home treatments haven’t produced noticeable improvement after three months of consistent application, professional assessment can determine whether a stronger approach is needed. Early intervention by a healthcare provider significantly increases your chances of successful treatment with less aggressive measures. For more information on how professional therapy compares to home treatments, check out this article on home treatment vs professional therapy.
Red Flags That Require Medical Attention
Certain symptoms indicate your toenail fungus requires immediate professional care. Pain, increased warmth, redness extending beyond the nail itself, or discharge suggests the infection has spread beyond the nail or a secondary bacterial infection has developed. These complications require prompt medical evaluation to prevent serious consequences, particularly for individuals with diabetes or compromised immune function.
Choosing Between a Podiatrist and Dermatologist
Both podiatrists and dermatologists effectively treat toenail fungus, but their expertise differs slightly. Podiatrists specialize in comprehensive foot care and may offer particular expertise if your fungal infection involves surrounding tissues or is complicated by other foot conditions. Their training specifically addresses the biomechanical aspects of foot health that may contribute to recurring infections.
What to Expect at Your Appointment
During your initial consultation, the healthcare provider will examine the affected nails and likely take samples for laboratory confirmation of fungal infection. This testing distinguishes fungal infections from other conditions like psoriasis or traumatic injury that can mimic fungal symptoms. Based on infection severity, nail involvement percentage, medical history, and medication sensitivities, your provider will recommend a treatment plan tailored to your specific situation.
Frequently Asked Questions
Toenail fungus generates numerous questions due to its persistent nature and varied treatment approaches. The following questions address the most common concerns patients express when dealing with this condition.
Treatment Success Rates by Approach
Oral antifungals: 60-75% complete cure
Prescription topicals: 30-50% complete cure
Laser therapy: 30-60% improvement
OTC treatments: 15-30% complete cure
Natural remedies: 10-20% complete cureUnderstanding these success rates helps set realistic expectations and explains why healthcare providers often recommend combination approaches for stubborn infections. The relatively modest success rates even with prescription treatments highlight why prevention remains crucial.
Can I use the same treatment for fingernail and toenail fungus?
While fingernail and toenail fungus share similarities, important differences influence treatment approaches. Fingernails grow approximately twice as fast as toenails (3mm monthly versus 1.5mm), allowing for quicker visible improvement and shorter treatment duration. Fingernails also experience less trauma and confined environments than toenails, generally making them more responsive to treatment.
Most antifungal medications—both topical and oral—effectively treat both fingernail and toenail infections, though dosage adjustments may be necessary. However, fingernail infections more commonly involve Candida species rather than dermatophytes, potentially affecting medication selection. Your healthcare provider may recommend slightly different approaches based on the specific infection location and causative organism.
For mild cases, the same over-the-counter treatments often work for both finger and toenails, though fingernail infections typically resolve more quickly due to faster growth rates and better circulation. The preventive measures differ slightly—while toenail protection focuses on footwear and shower facilities, fingernail protection emphasizes minimizing prolonged water exposure and avoiding potential contamination from shared manicure tools.
Is it safe to get pedicures if I have toenail fungus?
Professional pedicures during active fungal infections pose several concerns: potential transmission to other clients, possible worsening of your infection through trauma during nail filing, and reduced effectiveness of your current treatment due to removal of topical medications. Most dermatologists recommend postponing professional pedicures until the infection resolves completely. If you do proceed with a pedicure, bring your own sterilized tools and inform the technician of your condition so they can take additional precautions.
Will my insurance cover laser treatment for toenail fungus?
Most insurance plans classify laser treatment for toenail fungus as cosmetic and therefore don’t provide coverage. Medicare and most private insurers typically cover oral and topical prescription treatments but exclude laser therapy despite its FDA clearance. The out-of-pocket cost for laser treatment averages $800-$1,200 for a complete treatment series of 3-4 sessions.
Some podiatrists offer financing plans to make this treatment more accessible. If you’re considering laser treatment, request a detailed breakdown of all costs involved and verify whether any portion might qualify for insurance reimbursement, particularly if you have diabetes or other conditions that elevate your risk of complications.
Can toenail fungus spread to other parts of my body?
Toenail fungus can indeed spread to other areas, most commonly to adjacent toenails, the skin between toes (athlete’s foot), and occasionally to fingernails through direct contact. The same fungal organisms responsible for nail infections opportunistically colonize skin when conditions permit. To prevent spread, avoid touching infected nails and then touching other body areas without handwashing, use separate towels for feet and body, and apply antifungal powder to surrounding skin as a preventive barrier.
How do I prevent spreading toenail fungus to family members?
Preventing household transmission requires consistent preventive measures. Never share footwear, socks, towels, or nail care tools with family members. Disinfect shower floors regularly with antifungal cleaners containing bleach or quaternary ammonium compounds. For shared bathrooms, consider using disposable shower mats or disinfecting permanent mats daily. Infected individuals should apply topical treatments as directed and contain nail clippings in sealed bags for immediate disposal.
Educate family members about transmission risks and encourage protective footwear in shared bathroom spaces. Studies show these simple precautions dramatically reduce household transmission rates, preventing the frustrating cycle of passing infections between family members.
If multiple family members develop symptoms, simultaneous treatment helps prevent reinfection cycles. Consider implementing a “shoes-on” or “slippers-only” policy for the infected individual within common household areas until the infection resolves.
Patient Experience Timeline
Weeks 1-4: Initial treatment begins, little visible change
Months 2-3: First signs of clear growth at cuticle
Months 4-6: Clear delineation between healthy/infected nail
Months 6-12: Progressive growth of clear nail
Month 12+: Complete replacement with healthy nailThis timeline helps patients maintain realistic expectations and recognize that apparent lack of progress in the early months doesn’t indicate treatment failure. The fungus may be effectively neutralized long before visual evidence appears.

 Nail Fungus Cures Instant Cures for Painful Nails and Fungus
Nail Fungus Cures Instant Cures for Painful Nails and Fungus