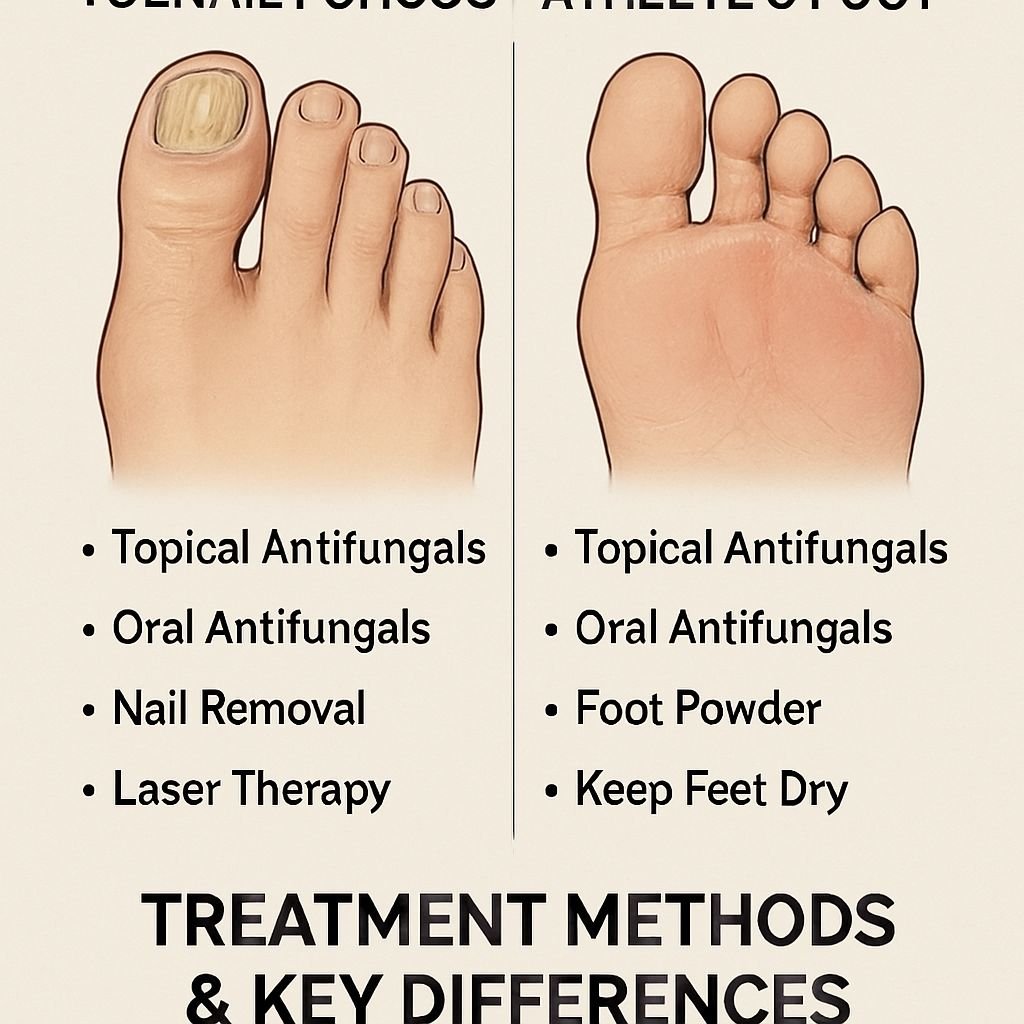
Key Takeaways – Toenail Fungus, Athlete’s Foot Treatment Methods & Key Differences
- Toenail fungus affects the nail bed causing discoloration and thickening, while athlete’s foot primarily impacts the skin with itching and scaling
- Though caused by similar fungi, these conditions require different treatment approaches – topical treatments work better for athlete’s foot while toenail fungus often needs more aggressive intervention
- Natural remedies like tea tree oil can be effective for both conditions when used consistently and properly
- Preventing reinfection requires daily hygiene practices, proper footwear, and environmental controls
- Those with diabetes or compromised immunity should seek professional care immediately for any foot fungal infection
What’s Really Causing Your Foot Fungus? Understanding Toenail Fungus vs. Athlete’s Foot
That itching, burning sensation or unsightly nail discoloration has you wondering what’s happening with your feet. Though both toenail fungus and athlete’s foot are fungal infections affecting the feet, they’re distinctly different conditions requiring specific treatments. Florida Foot and Ankle specialists explain that understanding the differences is crucial for effective treatment and prevention of these common but troublesome conditions.
Fungal infections thrive in warm, moist environments – exactly what your feet provide when trapped inside shoes all day. Both conditions are caused by dermatophytes, a group of fungi that feed on keratin found in nails and skin. However, they manifest differently, attack different parts of the foot, and respond to different treatment approaches.
What makes these conditions particularly frustrating is their persistence and tendency to recur if not properly addressed. The good news? With the right approach, both toenail fungus and athlete’s foot can be effectively managed and even eliminated. Let’s dive into the specifics of each condition to help you identify what you’re dealing with and how to treat it.
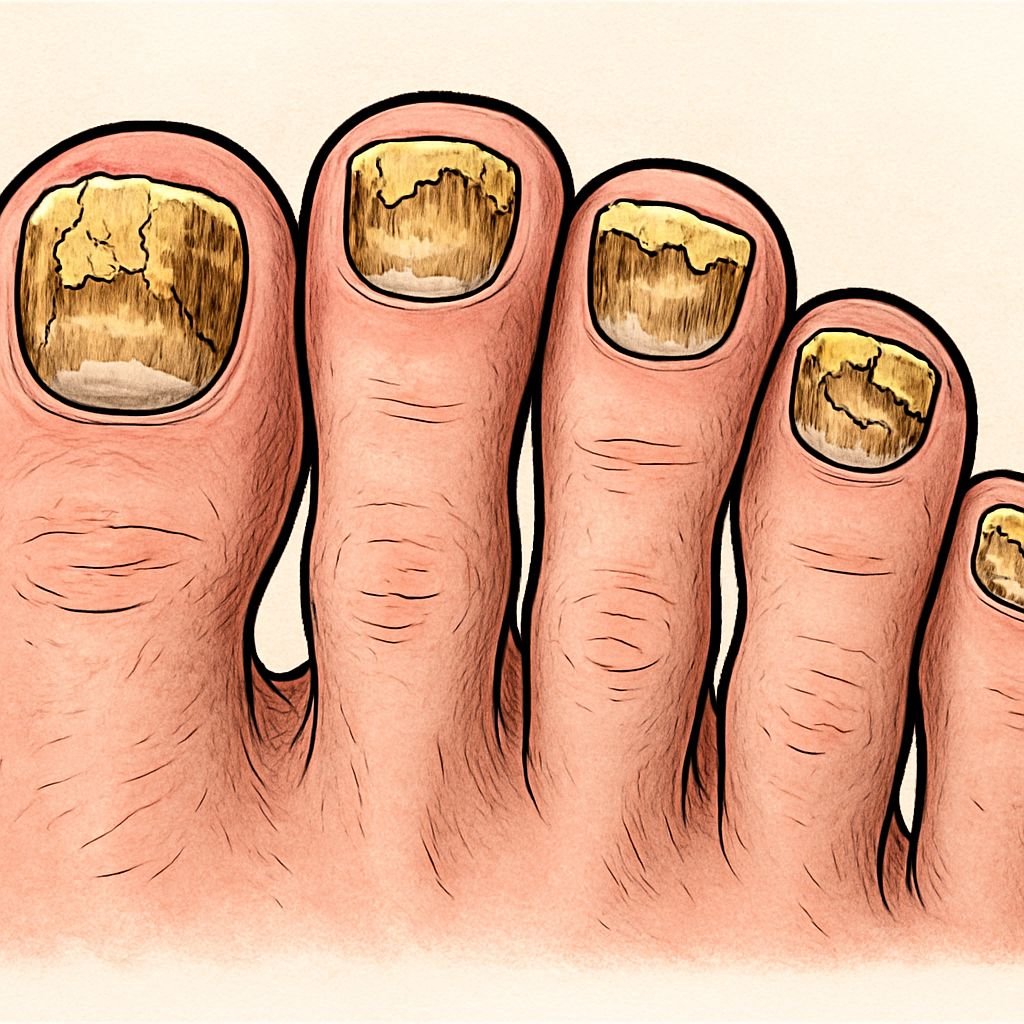
Toenail Fungus: Symptoms That Shouldn’t Be Ignored
Toenail fungus, medically known as onychomycosis, affects millions of people worldwide and becomes more common as we age. Unlike athlete’s foot which can develop quickly, toenail fungus typically starts subtly and progresses slowly, making early detection challenging. By the time many people notice the symptoms, the infection has often established a stronghold in the nail bed.
How Toenail Fungus Develops and Spreads
Toenail fungus typically begins when fungi enter through tiny cracks in the nail or the surrounding skin. These microscopic invaders find the warm, dark environment under your toenail particularly hospitable. Initially, the infection may appear as a small white or yellow spot under the nail tip, but as fungi multiply, they spread deeper into the nail bed.
The infection progresses gradually, often taking months or even years to fully develop. During this time, the fungi digest keratin – the protein that gives your nails their strength and structure. Without intervention, the infection can spread from one toenail to another or even to fingernails through direct contact or shared items like nail clippers.
Visual Signs: Yellow Discoloration, Thickening, and Crumbling
The most recognizable symptoms of toenail fungus are visual changes to the nail itself. As the infection progresses, you’ll notice your once transparent or pink nail taking on a yellowish or brownish hue. This discoloration typically starts at the tip of the nail and gradually works its way toward the cuticle as the infection spreads.
- Yellowing or whitish discoloration that gradually darkens to brown or black
- Thickening of the nail, making it difficult to trim
- Crumbling or ragged edges as the nail structure breaks down
- Distortion in nail shape, often with raised ridges or bumps
- Separation of the nail from the nail bed (onycholysis)
The severity of these symptoms varies significantly between individuals. Some may experience only mild discoloration with minimal thickening, while others develop severely distorted, thickened nails that cause significant discomfort and embarrassment. Without treatment, symptoms typically worsen over time rather than improve. For more information on effective remedies, check out this treatment remedies guide.
Pain and Discomfort: When Fungal Nails Become Problematic
While early-stage toenail fungus may be painless, advanced infections often cause discomfort that impacts daily life. As the nail thickens, it creates pressure against your shoe, leading to pain with each step. The distorted shape may cause the nail to dig into surrounding skin, creating additional tenderness and potential for bacterial infections.
For people with diabetes or compromised immune systems, toenail fungus represents more than a cosmetic concern – it’s a potential gateway to serious complications. The cracks and breaks in infected nails create entry points for bacteria, which can lead to cellulitis or other infections that spread beyond the foot. This is why prompt attention to any nail changes is especially important for these populations.
- Discomfort or pain when wearing shoes, especially tight-fitting ones
- Tenderness in the toe or surrounding skin
- Difficulty walking or engaging in physical activities
- Embarrassment about nail appearance, leading to avoidance of situations where feet are visible
Athlete’s Foot: More Than Just Itchy Skin
Athlete’s foot (tinea pedis) is significantly more common than toenail fungus, affecting up to 70% of people at some point in their lives. Unlike toenail fungus, athlete’s foot develops and spreads quickly, sometimes appearing within days of exposure to the fungus. The condition earned its name because it’s particularly common among athletes who frequently use communal showers and locker rooms, but anyone can develop this irritating skin infection.
This skin infection is highly contagious and can spread from person to person through direct contact or shared surfaces. You might pick up the fungi from walking barefoot in locker rooms, around swimming pools, or from sharing towels or shoes with an infected person. Once the fungi find their way onto your skin, the warm, moist environment inside your shoes creates perfect conditions for them to multiply rapidly.
While often dismissed as a minor inconvenience, untreated athlete’s foot can lead to more serious complications, including bacterial infections and the spread of fungus to the toenails. Understanding the symptoms and taking prompt action can help prevent these complications and provide quick relief from the irritating symptoms.
Common Locations and Appearance of Athlete’s Foot
Athlete’s foot typically begins between the toes, particularly the fourth and fifth toes, where moisture tends to accumulate most. This area provides the perfect environment for fungal growth – warm, dark, and often damp. The infection can spread to the soles and sides of the feet, and in severe cases, it may extend to the heels or even the palms of your hands if you touch the infected area and then touch other parts of your body.
The appearance of athlete’s foot varies depending on the type and severity of the infection. The most common form, interdigital athlete’s foot, presents as cracked, peeling, or scaly skin between the toes. Moccasin-type athlete’s foot affects the sole and sides of the foot with a thickened, scaly surface that may crack and cause pain when walking. The vesicular type, the least common but most severe, causes blisters filled with fluid to form on the foot, most often on the instep or sole.
The Telltale Itch, Burning, and Scaling
The hallmark symptom of athlete’s foot is intense itching, especially between the toes or on the soles of the feet. This itching often worsens after removing shoes and socks, as exposure to air can stimulate nerve endings in the affected skin. Many people describe a burning or stinging sensation accompanying the itch, particularly when the skin becomes cracked or develops small fissures. For a deeper understanding of how to combat these symptoms, consider exploring the science behind antifungal treatments.
Beyond the discomfort, visual symptoms include redness, scaling, and flaking of the skin. The affected areas may appear inflamed and slightly swollen, with dry, scaly patches that peel away to reveal tender skin underneath. Some people notice a white, soggy appearance between the toes where skin has been continually moist. Unlike toenail fungus which develops slowly, these symptoms can appear rapidly, sometimes within days of exposure to the fungus. For more information on effective treatments, explore the best prescription treatments for toenail fungus.
- Intense itching that often worsens at night
- Burning or stinging sensations in affected areas
- Redness and inflammation of the skin
- Dry, flaky, or scaly patches
- Small blisters that may ooze fluid
- Cracked or peeling skin, especially between toes
How Athlete’s Foot Can Lead to Toenail Infections
One of the most significant complications of athlete’s foot is its potential to spread to the toenails. The same fungi that cause athlete’s foot can migrate to the nail bed, especially if there are small cuts or separations between the nail and skin. Once established under the nail, the infection transforms from athlete’s foot to onychomycosis (toenail fungus), which is significantly more difficult to treat.
This progression often happens when athlete’s foot goes untreated for extended periods. The longer the fungi remain active on the skin, the greater the opportunity for them to spread to the nails. People who scratch infected areas may inadvertently transfer fungi to their nails through micro-abrasions created by scratching. This connection between the two conditions highlights why prompt treatment of athlete’s foot is essential not just for immediate relief, but also for preventing more persistent nail infections.
Key Differences Between Toenail Fungus and Athlete’s Foot
While both toenail fungus and athlete’s foot are caused by similar fungi, they differ significantly in how they present, progress, and respond to treatment. Understanding these distinctions is crucial for selecting the most effective approach to heal your particular condition. The differences extend beyond mere location, encompassing transmission patterns, development timelines, and treatment requirements.
Affected Areas: Skin vs. Nail Tissue
The most obvious difference between these two conditions is the tissue they affect. Athlete’s foot primarily targets the epidermis—the outermost layer of skin—especially in the spaces between toes and on the soles of feet. The infection remains relatively superficial, rarely penetrating beyond the upper skin layers. This surface-level nature makes it more responsive to topical treatments, as medications can directly reach the fungi.
Toenail fungus, by contrast, invades the nail plate and the nail bed beneath it. The hard, protective nail creates a barrier that shields the fungi from many treatments, making this condition notoriously difficult to eradicate. The infection penetrates deep into the nail matrix (the tissue that produces the nail), which explains why affected nails often grow out already infected. This fundamental difference in location largely accounts for why toenail fungus typically requires longer, more aggressive treatment approaches.
Clinical Comparison: Athlete’s Foot vs. Toenail Fungus
While examining patients, I notice athlete’s foot responds to treatment within weeks, whereas toenail fungus often requires months of consistent therapy. The nail’s protective barrier significantly impedes medication absorption, making fungal nail infections among the most persistent conditions I treat in my practice.
Transmission Methods and Risk Factors
Both conditions can be acquired from similar sources, but their transmission patterns differ slightly. Athlete’s foot is highly contagious and spreads easily in warm, moist environments like locker rooms, swimming pools, and communal showers. The fungi responsible can live on floors, towels, and shoes, making direct contact with contaminated surfaces a primary transmission route. Person-to-person transmission is also common, particularly in households where bathroom floors and shower stalls are shared.
Toenail fungus, while also transmissible, requires more specific conditions for infection to occur. The fungi typically need to find entry through small cuts or separations between the nail and nail bed. Risk factors for developing toenail fungus include increasing age, reduced blood circulation, diabetes, excessive sweating, and a history of athlete’s foot. Genetic factors may also play a role in susceptibility, as some families seem to have higher incidence rates than others.
- Athlete’s foot spreads rapidly through direct contact with contaminated surfaces
- Toenail fungus requires entry points like cuts or separations in the nail
- Sweaty feet increase risk for both conditions but affect transmission differently
- Immune function influences susceptibility to both infections
- Previous foot trauma increases risk specifically for toenail fungus
Timeline: How Quickly Each Condition Develops and Spreads
The development timeline represents another key difference between these conditions. Athlete’s foot can manifest quickly, sometimes appearing within days of exposure to the fungus. Symptoms typically develop rapidly, with itching, burning, and visible skin changes becoming apparent within a week or two of infection. Without treatment, the condition can spread across the foot and even to the other foot or hands through scratching and contact. For those dealing with toenail fungus, understanding treatment remedies can be crucial in managing the condition effectively.
Toenail fungus progresses much more slowly and insidiously. The initial infection may begin with a small white or yellow spot on the nail that’s easy to overlook. Over months or even years, this spot gradually expands as fungi colonize more of the nail. Many people don’t seek treatment until the infection has progressed significantly, with the nail becoming discolored, thickened, and distorted. This slow progression contributes to the challenge of treating toenail fungus, as by the time symptoms become obvious, the infection is often well-established.
6 Effective Home Remedies for Toenail Fungus
When facing the stubborn challenge of toenail fungus, many people prefer to start with natural approaches before moving to pharmaceutical options. Home remedies can be particularly effective for mild to moderate infections when used consistently. While these approaches generally take longer to produce results than prescription medications, they often come with fewer side effects and can be integrated into your daily routine with minimal disruption.
1. Tea Tree Oil Applications
Tea tree oil stands as one of the most researched natural antifungals, with multiple studies confirming its effectiveness against the dermatophytes responsible for toenail fungus. This powerful essential oil contains compounds like terpinen-4-ol that disrupt fungal cell membranes and inhibit growth. For maximum effectiveness, use 100% pure tea tree oil applied directly to affected nails twice daily with a cotton swab or dropper.
Consistency is crucial when using tea tree oil for nail fungus. Most users begin to see improvement after 3-6 months of regular application. To enhance absorption, consider lightly filing the nail surface before application and covering the treated nail with a bandage for several hours afterward. For those with sensitive skin, diluting tea tree oil with a carrier oil like coconut or olive oil (1:1 ratio) can prevent irritation while still delivering antifungal benefits.
2. Apple Cider Vinegar Soaks
Apple cider vinegar creates an acidic environment hostile to fungal growth while supporting the natural pH of healthy skin. Its acetic acid content works by penetrating the nail plate and inhibiting the adhesion and growth of fungal organisms. For an effective treatment, mix equal parts apple cider vinegar and warm water in a basin large enough to submerge your affected toes, then soak for 20-30 minutes daily.
These soaks work gradually by softening the nail plate, allowing the acidic components to reach deeper layers where fungi reside. Many users report noticing improved appearance after 2-3 weeks of daily soaks, though complete resolution typically requires several months of consistent treatment. For enhanced results, dry your feet thoroughly after soaking and apply an antifungal oil like tea tree or oregano to the affected nails.
3. Oregano Oil’s Antifungal Properties
Oregano oil contains powerful compounds like carvacrol and thymol that have demonstrated significant antifungal properties in numerous studies. These natural chemicals disrupt the cellular membranes of fungi, effectively killing them and preventing reproduction. For toenail fungus treatment, dilute pure oregano oil with a carrier oil like olive or coconut oil in a 1:3 ratio before applying to affected nails with a cotton swab.
Apply this mixture to affected nails twice daily, gently massaging it into and around the nail to ensure thorough coverage. Many users report a warming or tingling sensation after application, which is normal and indicates the active compounds are working. Oregano oil treatments typically require 3-6 months of consistent application to see significant improvement, though some people notice reduced discoloration within weeks.
This potent essential oil should always be diluted before use, as direct application can cause skin irritation or burning. Pregnant women should avoid oregano oil treatments entirely, as should those taking blood-thinning medications, since oregano oil may interact with these drugs.
4. Coconut Oil as a Natural Alternative
Coconut oil offers a gentler approach to treating toenail fungus, making it ideal for those with sensitive skin or who cannot tolerate stronger remedies. Its medium-chain fatty acids, particularly lauric acid, have documented antifungal properties that can penetrate the nail plate. For best results, apply organic, cold-pressed virgin coconut oil to affected nails after thoroughly cleansing and drying the area. Learn more about natural remedies and solutions for nail fungus.
Unlike more potent remedies, coconut oil can be applied liberally and as frequently as desired without risk of irritation. Many people incorporate it into their routine by massaging it into nails morning and night, then wearing cotton socks to prevent transfer to bedding. The oil’s moisturizing properties also help address the brittleness and cracking often associated with fungal infections, improving nail appearance while fighting the underlying infection.
While generally milder than other treatments, coconut oil works best for early-stage infections or as a complementary treatment alongside more potent antifungals. Some users enhance its effectiveness by mixing in a few drops of tea tree or oregano oil, creating a more powerful but still skin-friendly solution.
5. Garlic’s Powerful Antifungal Compounds
Garlic has been used medicinally for centuries, with modern research confirming its potent antimicrobial properties. Allicin, the compound responsible for garlic’s distinctive odor, exhibits strong antifungal activity against the organisms causing toenail fungus. Fresh garlic delivers the most potent treatment, as allicin is produced when garlic cloves are crushed or chopped. For more natural remedies, explore the best essential oil blends for nail fungus.
To create an effective treatment, crush several garlic cloves into a paste and apply directly to affected nails, covering with a bandage for 30 minutes before rinsing. For those concerned about the strong odor, mixing crushed garlic with coconut or olive oil creates a less pungent but still effective remedy. Apply this mixture daily, ideally before bed, allowing the compounds to work overnight while you sleep.
While garlic treatments can cause temporary skin irritation or burning sensations in some individuals, this approach offers a cost-effective alternative to commercial products. Consistent application typically shows nail improvement within 2-3 months, though complete clearing may take longer depending on the severity of the infection. For those interested in exploring more natural remedies, consider trying essential oil blends for nail fungus as another option.
6. Proper Nail Hygiene and Maintenance
Beyond applying antifungal substances, proper nail care forms the foundation of effective home treatment for toenail fungus. Keeping nails clean, dry, and properly trimmed creates an environment where fungi struggle to thrive while supporting your body’s natural defenses against infection. Trim nails straight across and file down thickened areas gently to allow topical treatments better access to infected areas.
Dedicated nail tools play a crucial role in treatment success. Use separate clippers and files for infected nails to prevent spreading the fungus to healthy nails, and disinfect these tools after each use by soaking in rubbing alcohol or a diluted bleach solution. Avoid painting infected nails with polish, as this traps moisture and creates ideal conditions for fungal growth.
- Keep nails short, dry, and clean at all times
- Use dedicated tools for infected nails
- Disinfect tools after each use
- Avoid nail polish on infected nails
- Wear moisture-wicking socks
- Allow feet to breathe whenever possible
5 Quick Relief Methods for Athlete’s Foot
Unlike toenail fungus which requires months of treatment, athlete’s foot often responds quickly to home remedies. These approaches not only alleviate the uncomfortable symptoms but can effectively eliminate the infection when used consistently. The key to success lies in creating an environment where fungi cannot survive while supporting your skin’s natural recovery process.
1. Salt and Vinegar Foot Baths
This simple yet effective remedy combines the antifungal properties of vinegar with salt’s exfoliating and drying effects. The acidic environment created by vinegar inhibits fungal growth, while salt helps remove dead skin cells and reduces moisture. Mix one cup of vinegar (white or apple cider) and half a cup of salt in a basin of warm water large enough to submerge your feet. For more information on the benefits of vinegar foot soaks, visit this vinegar foot soaks guide.
Soak feet for 15-20 minutes daily, then dry thoroughly, paying special attention to the spaces between toes. Many people notice immediate relief from itching and burning sensations after the first treatment, with visible improvement in skin condition within 3-5 days of consistent use. This remedy works particularly well for interdigital athlete’s foot, the most common form that affects the spaces between toes.
For enhanced effectiveness, follow each soak with a thorough application of antifungal powder to keep feet dry throughout the day. The combination of acidic treatment and moisture control creates a two-pronged approach that significantly speeds healing time.
2. Baking Soda Paste Applications
Baking soda offers multiple benefits for athlete’s foot treatment: it neutralizes odor, reduces moisture, and creates an alkaline environment unfavorable to fungal growth. Its mild abrasive quality also helps remove infected skin cells, accelerating the healing process. Create a thick paste by mixing baking soda with just enough water to form a spreadable consistency.
Apply this paste directly to affected areas, concentrating on spaces between toes and any particularly red or itchy spots. Allow the paste to dry completely before rinsing with cool water and thoroughly drying your feet. For maintenance, sprinkle dry baking soda in your shoes and socks to absorb moisture and prevent reinfection.
This remedy provides particularly effective relief for the burning and itching associated with athlete’s foot, often delivering noticeable symptom improvement within 24 hours of first application. For best results, apply the paste twice daily until all symptoms resolve, typically within 1-2 weeks for mild to moderate infections. For more information on effective treatments, check out this antifungal powder.
3. Aloe Vera’s Soothing Benefits
While primarily known for its soothing properties, aloe vera also possesses antifungal and anti-inflammatory qualities that make it valuable for athlete’s foot treatment. The plant’s gel contains compounds that inhibit fungal growth while simultaneously calming irritated skin and reducing redness. For treatment, use pure aloe vera gel applied directly to clean, dry feet, focusing on affected areas.
Aloe’s cooling effect provides immediate relief from the burning and itching associated with athlete’s foot, making it particularly beneficial for painful fissures or cracks in the skin. Apply the gel 3-4 times daily, allowing it to fully absorb before putting on socks or shoes. Many people notice significant comfort improvement within hours of first application, with visible healing of damaged skin within days.
While gentler than some other remedies, aloe works best for mild cases or as a complementary treatment alongside more potent antifungals. Its skin-healing properties make it especially valuable in the recovery phase, helping restore normal skin texture and appearance after the infection subsides.
4. Neem Oil for Persistent Infections
Derived from the neem tree, this potent botanical oil contains over 60 compounds with antifungal, antibacterial, and anti-inflammatory properties. Neem disrupts the life cycle of fungi, preventing them from reproducing while its azadirachtin content penetrates the skin to target fungi beneath the surface. For athlete’s foot treatment, apply diluted neem oil (mix 1 part neem oil with 10 parts carrier oil) directly to affected areas twice daily.
Neem oil’s power makes it particularly effective for stubborn or recurring athlete’s foot infections that haven’t responded to milder treatments. Its strong odor and potential for skin sensitivity means it should be used with caution, starting with a small test area before wider application. Despite these considerations, many users report significant improvement within a week of consistent use, even with infections that have persisted for months.
- Apply diluted neem oil directly to affected areas
- Use morning and night after washing and drying feet
- Continue application for 7-10 days after symptoms resolve
- Combine with foot soaks for enhanced effectiveness
- Store properly in a dark bottle away from direct sunlight
5. Essential Oil Blends for Itching Relief
A synergistic approach using multiple essential oils can provide powerful relief from athlete’s foot while addressing various aspects of the infection. Tea tree, lavender, peppermint, and eucalyptus oils each contribute unique benefits: tea tree kills fungi directly, lavender soothes irritation, peppermint cools itchy skin, and eucalyptus enhances penetration of the other oils. Create a blend by mixing 5 drops each of these oils with 2 tablespoons of coconut oil as a carrier.
Apply this blend to clean, dry feet twice daily, massaging gently to ensure even distribution. The cooling sensation from peppermint oil provides immediate itch relief, while the other components work to eliminate the underlying infection. This multi-oil approach addresses both symptoms and causes simultaneously, often providing visible improvement within 3-5 days.
The versatility of essential oil blends allows customization based on your specific symptoms and preferences. For predominantly itchy infections, increase the peppermint oil ratio; for particularly red or irritated skin, add more lavender. This personalized approach makes essential oil blends one of the most adaptable and effective home remedies for athlete’s foot.
When to Use Over-the-Counter Treatments
While natural remedies offer effective options for many people, over-the-counter (OTC) treatments provide a more standardized approach with proven active ingredients. These products typically work faster than home remedies and come in various formulations designed for different preferences and infection types. Consider switching to OTC options if home remedies haven’t produced improvement after two weeks of consistent use or if your symptoms are particularly severe.
Best Antifungal Creams for Athlete’s Foot
OTC creams containing clotrimazole, miconazole, or tolnaftate offer powerful relief for athlete’s foot, typically producing noticeable improvement within days of starting treatment. These azole antifungals work by disrupting the cell membranes of fungi, preventing them from reproducing while gradually eliminating existing organisms. For best results, apply a thin layer of cream to affected areas twice daily after thoroughly washing and drying your feet. For more information on effective treatments, check out this comprehensive guide on toenail fungus treatments.
Different active ingredients work better for different types of athlete’s foot. Clotrimazole generally proves most effective for interdigital infections (between toes), while tolnaftate works particularly well for the moccasin type that affects the soles. Miconazole offers good broad-spectrum coverage and often includes additional ingredients to relieve itching and inflammation. Most people see significant improvement within 7-10 days of consistent application, though treatment should continue for 1-2 weeks after symptoms resolve to prevent recurrence.
Topical Solutions for Early-Stage Toenail Fungus
For toenail fungus in its early stages, OTC solutions containing undecylenic acid or tolnaftate can effectively penetrate the nail plate to reach fungi in the nail bed. These liquid formulations typically come with brush applicators that allow precise application to affected nails without treating surrounding skin. Apply these solutions to clean, dry nails twice daily, allowing them to fully dry before putting on socks or shoes.
These products work best when the infection is limited to a small portion of the nail, typically less than 50% involvement. Filing the surface of affected nails before application significantly improves penetration and effectiveness. While results take time, many users report noticeable nail improvement within 8-12 weeks of consistent use, with continuing enhancement as the healthy nail grows out.
Combination Approaches for Better Results
Many healthcare providers recommend combining different treatment methods for faster, more complete resolution of fungal infections. For athlete’s foot, using an antifungal cream during the day and soaking feet in vinegar solution at night creates a comprehensive approach that targets fungi in different ways. Similarly, treating toenail fungus with both a topical solution and oral supplements like garlic or oregano oil capsules addresses the infection both externally and internally.
Environmental treatments form another important component of combination therapy. Using antifungal sprays or powders in shoes, washing socks in hot water with vinegar, and disinfecting shower floors all help prevent reinfection while active treatment progresses. This multi-faceted approach not only improves current infection outcomes but significantly reduces recurrence rates, which can be as high as 50% with single-method treatments.
Prescription Treatments: When Natural Remedies Aren’t Enough
Despite diligent application of home remedies and OTC treatments, some fungal infections prove particularly stubborn. When infections persist or worsen despite 2-3 months of consistent treatment, it’s time to consider prescription options. These more powerful interventions offer higher success rates but typically come with increased cost and potential for side effects.
Oral Antifungal Medications: Benefits and Side Effects
Prescription oral medications like terbinafine (Lamisil) and itraconazole (Sporanox) represent the most effective treatment for severe or resistant toenail fungus. These medications work systemically, reaching the nail bed through the bloodstream and attacking fungi from within. A typical treatment course lasts 6-12 weeks, though the medication continues working in the nail for months after you stop taking it.
Success rates for oral antifungals range from 70-80%, significantly higher than topical treatments alone. However, these medications require liver function monitoring through blood tests and may cause side effects ranging from headaches and digestive upset to rare but serious liver complications. Most healthcare providers reserve these treatments for extensive infections, those involving multiple nails, or cases where topical treatments have failed.
For those unable to take oral medications due to other health concerns or medication interactions, newer pulse-dosing regimens often provide effective alternatives with reduced side effect profiles. These protocols involve taking medication for one week per month over several months, lowering total drug exposure while maintaining efficacy.
Prescription-Strength Topicals
Between over-the-counter products and oral prescriptions lie prescription-strength topical treatments like ciclopirox (Penlac) and efinaconazole (Jublia). These solutions contain higher concentrations of antifungal agents specifically formulated to penetrate the nail plate more effectively than OTC alternatives. Application typically involves painting the solution onto affected nails daily, with treatment courses lasting up to 48 weeks.
These prescription topicals offer success rates of 35-50% for complete cure, with significantly higher rates of improvement. Their primary advantages include minimal systemic absorption and few side effects beyond occasional localized irritation. Many healthcare providers recommend these options for patients with moderate toenail fungus, those with contraindications to oral medications, or as part of a combination therapy approach.
Laser Therapy for Stubborn Toenail Fungus
For those seeking non-medication approaches to resistant toenail fungus, laser therapy offers an innovative alternative. These treatments use specific wavelengths of light to penetrate the nail and selectively target fungi without damaging surrounding tissue. The procedure is typically painless, requiring no anesthesia and allowing immediate return to normal activities afterward.
Most patients require 3-4 sessions spaced several weeks apart for optimal results. While the procedure itself takes only 20-30 minutes, visible improvement develops gradually as healthy nail grows out, typically becoming noticeable within 3-6 months. Success rates vary widely between different laser systems and providers, with complete cure rates ranging from 30-70% and significant improvement reported in up to 90% of cases.
The primary disadvantage of laser therapy remains its cost—typically $500-1200 per treatment series—which insurance rarely covers as it’s considered cosmetic by many plans. However, for those who cannot tolerate oral medications or have experienced treatment failures with other approaches, laser therapy provides a valuable option with minimal side effects and no drug interactions. For those seeking alternative solutions, exploring prescription treatments for toenail fungus might be beneficial.
- FDA-approved laser treatments specifically target fungal cells
- No recovery time needed after treatment
- Multiple sessions usually required for optimal results
- Can be combined with topical treatments for enhanced effectiveness
- Best results seen in people with good circulation to extremities
Prevention Strategies That Actually Work
After successfully treating a fungal foot infection, preventing recurrence becomes the primary concern. Fungi remain present in our environment, making reinfection possible without proper preventive measures. A comprehensive prevention strategy addresses multiple risk factors simultaneously, creating conditions where fungi struggle to reestablish themselves on your skin or nails.
Proper Footwear Selection and Rotation
Your choice of shoes significantly impacts your susceptibility to fungal infections. Opt for breathable materials like leather, canvas, or mesh that allow air circulation and moisture evaporation. Avoid plastic or rubber shoes that trap heat and sweat, creating ideal conditions for fungal growth. For athletic activities, choose shoes specifically designed for your sport with moisture-wicking properties and adequate ventilation.
Equally important is implementing a shoe rotation schedule. Wearing the same pair daily prevents shoes from fully drying between uses, creating a perpetually damp environment where fungi thrive. Alternating between at least two pairs allows each to dry completely, significantly reducing infection risk. For added protection, place shoes in sunlight periodically, as UV rays have natural antifungal properties that help sanitize footwear.
Daily Hygiene Practices That Make a Difference
Consistent foot hygiene forms the foundation of effective fungal prevention. Wash feet daily with soap and water, paying special attention to the spaces between toes where moisture accumulates. After washing, dry feet thoroughly, using a separate towel designated for feet only to prevent spreading fungi to other body parts. Apply antifungal powder or spray as a preventive measure, particularly before activities likely to cause sweating.
Sock selection plays a crucial role in prevention as well. Choose moisture-wicking materials like wool, specialized athletic blends, or cotton-synthetic blends rather than 100% cotton, which retains moisture. Change socks immediately after significant sweating, carrying spare pairs when engaging in athletic activities or during hot weather. For those with particularly sweaty feet, changing socks midday as a regular practice can dramatically reduce fungal infection risk.
Environmental Controls for Shared Spaces
Public spaces like locker rooms, swimming pools, and communal showers serve as common transmission sites for foot fungi. Always wear waterproof sandals or shower shoes in these environments, creating a barrier between your feet and potentially contaminated surfaces. Position yourself away from standing water when possible, as these areas typically harbor higher concentrations of microorganisms.
At home, regular disinfection of bathroom floors and shower stalls helps prevent family transmission. Use antifungal cleaning solutions containing bleach, vinegar, or commercial disinfectants weekly, paying particular attention to corners and crevices where moisture lingers. For households with an infected member, more frequent cleaning and designated bath mats for each person can prevent spreading the infection to others.
Dietary Changes to Strengthen Your Immune Response
Your diet directly impacts your body’s ability to resist and fight fungal infections. Focus on probiotic-rich foods like yogurt, kefir, and fermented vegetables, which support healthy gut flora and strengthen immune function. Include foods high in antifungal compounds such as garlic, onions, coconut oil, and oregano, which provide internal support against fungal overgrowth. Limiting refined sugars and simple carbohydrates further disadvantages fungi by reducing available fuel sources. For additional natural remedies, consider exploring vinegar foot soaks to enhance your body’s defense against fungal infections.
Certain nutritional supplements can enhance your natural defenses against fungal infections. Consider adding zinc, which supports skin healing and immune function, and vitamin D, which plays a crucial role in immune response regulation. For those with recurring infections, a comprehensive immune support formula containing vitamins C, E, and B-complex may provide additional protection by optimizing overall immune function. Additionally, understanding the science behind antifungal treatments can aid in selecting the right products for your needs.
When to See a Doctor: Red Flags You Shouldn’t Ignore
While many fungal foot infections respond well to home treatment, certain situations warrant professional medical attention. Recognizing these warning signs ensures you receive appropriate care before complications develop. Early intervention for serious infections not only improves outcomes but can prevent permanent nail or skin damage.
The timeframe for seeking professional care depends largely on your individual health status and the infection’s response to initial treatment. Generally, healthy individuals should consult a healthcare provider if self-treatment shows no improvement after 2-3 weeks, while those with compromised immunity or diabetes should seek professional care at the first sign of infection. For more information on effective treatments, you might consider exploring antifungal solutions that are scientifically proven to fight fungal infections.
Signs of Bacterial Infection
Fungal infections sometimes create skin breaks that allow bacteria to enter, resulting in secondary bacterial infections requiring different treatment approaches. Watch for increasing pain, swelling that extends beyond the original infection site, red streaks extending from the infection, or pus drainage. These symptoms indicate a potential bacterial component requiring antibiotic treatment.
Another concerning sign is rapidly worsening symptoms despite appropriate antifungal treatment. Fungi typically cause gradual changes, so sudden deterioration often signals bacterial involvement or an allergic reaction to treatment. Seek medical attention promptly if skin becomes unusually hot to touch, develops an unusual odor, or if you experience fever or chills in conjunction with your foot infection.
Fungal Infections in People with Diabetes or Compromised Immunity
People with diabetes face significantly higher risks from seemingly minor foot infections due to reduced sensation from neuropathy and compromised circulation. Even mild fungal infections can progress to serious complications if left untreated in diabetic individuals. If you have diabetes, consult your healthcare provider at the first sign of any foot infection rather than attempting home treatment.
Similarly, those with compromised immunity from conditions like HIV, cancer treatments, or immunosuppressive medications should seek professional care immediately for any foot infection. These individuals have reduced ability to contain and fight infections, allowing fungi to spread more rapidly and potentially enter the bloodstream. Professional monitoring and often stronger prescription treatments provide necessary protection for these vulnerable populations.
Treatment Resistance: When Nothing Seems to Work
Persistent infections that show no improvement despite several weeks of appropriate treatment require professional evaluation. This resistance may indicate misdiagnosis (as several skin conditions can mimic fungal infections), presence of resistant fungal strains, or underlying conditions preventing healing. A healthcare provider can perform laboratory testing to identify the specific organism involved and recommend targeted treatment based on those results.
Treatment failure sometimes occurs because the infection has spread more extensively than visible symptoms suggest. This is particularly common with toenail fungus, where fungi may have invaded the nail matrix or bone beneath without obvious external signs. In these cases, professional debridement (removal of infected tissue) combined with prescription treatments often proves necessary for resolution.
Heal Your Feet for Good: Maintaining Long-Term Foot Health
Achieving and maintaining healthy feet requires ongoing attention and care, particularly for those with a history of fungal infections. Beyond treating active infections, focus on creating an internal and external environment hostile to fungal growth. Incorporate foot inspection into your daily routine, checking for early signs of recurrence like slight discoloration, subtle texture changes, or mild itching that might otherwise go unnoticed. This vigilance allows for immediate intervention at the first sign of returning infection, when treatments prove most effective.
Frequently Asked Questions
Throughout my years helping patients overcome foot fungus issues, certain questions arise consistently. These common concerns reflect the confusion many people experience when dealing with these persistent conditions. Understanding these aspects of fungal infections can significantly improve your treatment success and prevent frustrating recurrences. For more detailed guidance, you can explore this treatment remedies guide.
Remember that while general guidelines apply to most cases, individual factors like overall health, medication use, and severity of infection can affect your specific treatment approach. When in doubt, consulting with a healthcare provider ensures you receive personalized guidance for your unique situation.
Can I get toenail fungus from a pedicure?
Yes, toenail fungus can be transmitted during pedicures if proper sanitation protocols aren’t followed. Choose reputable salons that sterilize tools between clients using medical-grade autoclaves or chemical disinfectants, not just UV sanitizers. Bring your own tools when possible, especially nail files and buffers which can harbor fungi even after surface cleaning. Additionally, request that technicians not push back or cut your cuticles, as these practices can create microscopic entry points for fungi to access your nail bed.
How long does it take to cure athlete’s foot completely?
Mild to moderate athlete’s foot typically resolves within 2-4 weeks of consistent treatment with appropriate antifungals. However, this timeline varies significantly based on the specific type of athlete’s foot, treatment method, and individual factors like immune function and foot moisture levels. Interdigital athlete’s foot (between toes) generally responds fastest, often showing improvement within days and resolving completely in 1-2 weeks with proper treatment.
Complete cure requires continuing treatment for 1-2 weeks beyond symptom resolution to eliminate remaining fungi and prevent immediate recurrence. Without this extended treatment period, seemingly cured infections often return rapidly as surviving fungi reproduce. For chronic or recurrent cases, maintenance therapy with weekly preventive treatments may be necessary for months to break the cycle of infection.
Is it possible to have both conditions at the same time?
Absolutely, and this combination occurs frequently. When both conditions exist simultaneously, they often feed into each other, creating a challenging cycle to break. Athlete’s foot can spread to the nails, causing toenail fungus, while infected toenails continuously release fungi that reinfect the surrounding skin. This dual infection requires a comprehensive treatment approach addressing both areas concurrently to prevent the “ping-pong effect” where one condition constantly reinfects the other.
Will my fungal infection return after treatment?
Recurrence rates for fungal infections range from 10-50% depending on the condition and preventive measures taken. The primary factors influencing recurrence include incomplete eradication of the original infection, continued exposure to environmental fungi, and individual susceptibility factors like excessive foot sweating or compromised immunity. Implementing consistent preventive practices significantly reduces recurrence risk, with studies showing that simple measures like daily antifungal powder application can decrease recurrence by up to 70% compared to no preventive care.
Can I exercise while treating a foot fungus infection?
You can continue exercising while treating fungal foot infections, but modifications help prevent worsening the condition. Choose breathable athletic shoes, change socks immediately after workouts, and allow shoes to dry completely between uses by alternating pairs. For water-based activities like swimming or water aerobics, wear water shoes to create a barrier between your feet and potentially contaminated surfaces. Apply antifungal powder before workouts to help absorb moisture, and reapply treatment immediately after showering following exercise.
Activities causing excessive pressure on infected toenails, like long-distance running or basketball, may need temporary modification if you’re experiencing nail pain. Consider lower-impact alternatives like cycling or swimming until the most painful phase resolves. Remember that maintaining physical activity supports overall immune function, potentially speeding healing when appropriate precautions are taken.

 Nail Fungus Cures Instant Cures for Painful Nails and Fungus
Nail Fungus Cures Instant Cures for Painful Nails and Fungus